Research Article
Volume 2 Issue 5 - 2018
Percutaneous Figure-of-8, Tension-Band Suture Technique for Patella Fracture Fixation
1Simonian Sports Medicine Clinic
2Clinical Associate Professor, University of Washington, Department of Orthopaedic Surgery and Sports Medicine
2Clinical Associate Professor, University of Washington, Department of Orthopaedic Surgery and Sports Medicine
*Corresponding Author: Peter T Simonian, Simonian Sports Medicine Clinic, 729 N Medical Center Drive West, Suite 101 Clovis, CA 93611.
Received: October 15, 2018; Published: November 03, 2018
Abstract
Ten patients with patella fractures were successfully treated with a minimally invasive, percutaneous technique, utilizing a non-metallic suture, figure-of-8, tension band fixation construct. All patients achieved fracture union. No patient had displacement of the reduced fracture. No patient required fixation suture removal. All patients achieved acceptable range of motion. There were no post-operative complications. This fixation technique allowed for immediate mobilization in all cases.
Introduction
We previously described a case report of a transverse distal patella fracture successfully treated with a minimally invasive percutaneous technique, using a non-metallic suture, figure-of-eight, tension band construct [16]. Patella fractures are relatively common [2]. Surgical treatment goals should include preservation of the patella to the greatest possible extent, precise anatomic reduction of the joint surface by stable fixation, and restoration of the knee-extensor mechanism, thus allowing early mobilization [3, 10]. Posttraumatic osteoarthritis can result from articular incongruity [5].
A modified tension-band wiring technique [5, 11, 13 and 19] has been described for managing patella fracture fixation, with longitudinal Kirschner wires (K-wires) and 18-gauge stainless steel wire in a figure-of-eight pattern looped over the anterior surface of the patella, through an extensile incision. The tension-band technique biomechanically neutralizes tension forces anteriorly produced by the extensor mechanism at knee flexion and converts them into stabilizing compressive forces at the articular surface [19]. This technique has been further modified using either K-wires or cannulated screws with different stainless steel wire configurations. These tension-band techniques using metallic wires can result in symptomatic hardware, with reported rates up to 60% [10, 12 and 14]. For this reason, some have advocated the use of nonabsorbable sutures, such as braided polyester, lowering the rate of revision surgery secondary to symptomatic hardware [4,6,7,9,10 and 15].
Fiber Wire (Arthrex, Naples, FL, USA) has presented a significantly higher failure load than stainless steel wire. Furthermore, it was observed that, unlike stainless steel, Fiber Wire maintained its initial stiffness until failure [20]. A recent study demonstrated that a modified tension band using Fiber Wire sutures showed satisfactory clinical results with low incidence of complications and reoperations [4]. Ultra tape (Smith & Nephew, Andover, MA, USA) has similar strength with the added advantage of greater surface-contact area to minimize the chance of suture cutting through tendon. The Ultra tape also allows for lower profile suture knots when compared to Fiber Wire.
Traditionally, an extensile skin incision with a substantial soft tissues dissection sufficient for fracture and joint-surface visualization is normally utilized. Extensile incisions can be associated with postoperative adhesions [1], prolonged disability, and scarring [17]. The presence of lacerations or abrasions around the operative site may delay the surgery through a traditional midline incision [2]. Percutaneous surgical techniques, in contrast, preserve the vascular supply of patellar fragments, which may improve fracture consolidation. However, this treatment has been reported to be technically demanding and not applicable to all fracture patterns [18].
Surgical treatment of transverse patella fractures with this percutaneous technique utilizing cannulated screws with a tension band wiring technique, combining the advantages of rigid internal fixation and minimally invasive surgery, has shown to provide satisfactory clinical results and excellent knee functions, with less pain and low incidence of complications [8]. We report of a series of minimally displaced patella fractures treated with the combined advantages of both a minimally invasive percutaneous technique along and a non-metallic suture tension band.
Materials and Methods
We report a series of 10 patient’s average age 52.3 years (16-80 years) with unilateral patella fractures. The time from injury to surgical repair was an average of 16.36 days (2-37). Nine were female and one was male. All fractures were closed and the result of trauma. Six of the fractures were transverse and four were comminuted. The average fracture displacement was 2.5 cm (1-10cm).
Because of the minimal displacement, all 10 patients were surgically treated with our previously described percutaneous figure-of-8, tension band suture fixation [16]. Eight patients had a single figure-of-8 loop of either #5 Fiber Wire (Arthrex, Naples, FL, USA) or Ultra tape (Smith & Nephew, Andover, MA, USA). Two patients had two figure-of-8 suture loops for added fixation.
All 10 patients were treated with immediate weight bearing with a hinged knee brace locked in full extension for the first 6 weeks after surgery. Range of motion was started one week after surgery and was limited to no more than 90 degrees for the first six weeks. Limits on range of motion were discontinued after the first six weeks. All patients attended formal physical therapy two-times per week for a minimum of 12 weeks.
Technique
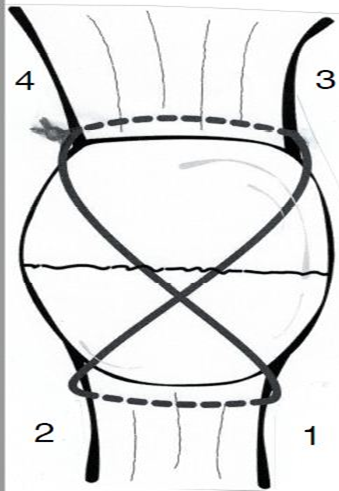
We previously described the minimally invasive percutaneous technique with a non-metallic figure-of-8 suture tension band [16]. Four small incisions were made, each measuring 3-5mm. Two on either side of the proximal patella tendon or two more on either side of the distal quadriceps tendon. Labeled 1-4 (Figure 1) [16].
We previously described the minimally invasive percutaneous technique with a non-metallic figure-of-8 suture tension band [16]. Four small incisions were made, each measuring 3-5mm. Two on either side of the proximal patella tendon or two more on either side of the distal quadriceps tendon. Labeled 1-4 (Figure 1) [16].
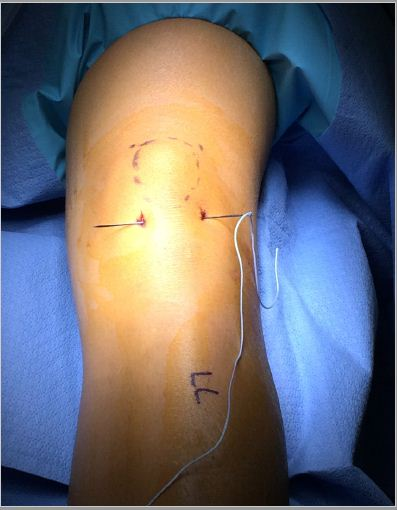
A large straight Keith needle is used to pass the suture starting from point 1 to 2, through the patella tendon at the inferior pole of the patella (Figure 2). The free suture end from point 2 is subcutaneously retrieved to point 3 with a Hewson suture passer (Smith and Nephew, Andover MA) (Figure 3). This free end of this suture is then passed from point 3 to 4 is with a straight Keith needle, through the quadriceps tendon at the superior pole of the patella (Figure 4). Finally, the other free suture end is retrieved from point 1 and delivered to point 4 (Figure 5). The free suture ends are then tensioned and tied at point 4 (Figure 6), completing the figure-of-8 tension band [16].
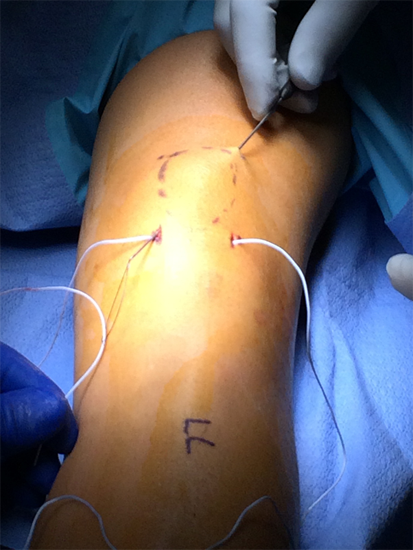
Figure 3: Hewson suture passer subcutaneous retrieval of the free suture end from
patella tendon, point 2, and delivering to the quadriceps tendon, point 3 [16].
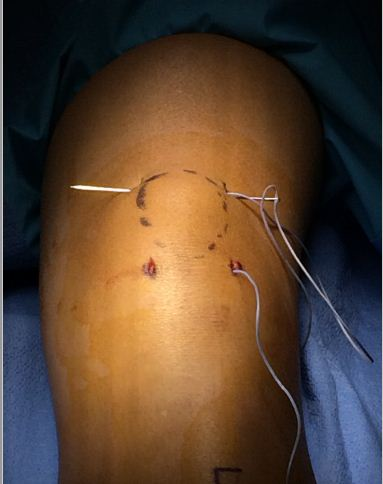
Figure 4: Keith needle placing the retrieved suture through
the distal quadriceps tendon, point 3 to 4 [16].
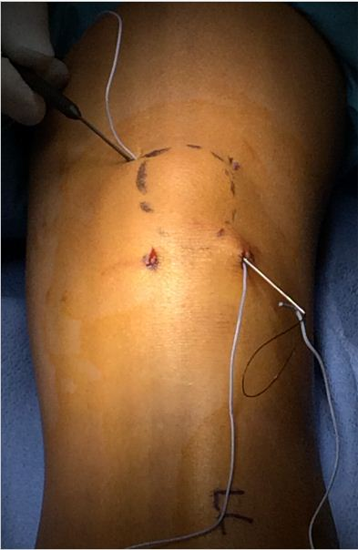
Figure 5: Hewson suture passer subcutaneous retrieval of
the free suture at the patella tendon, point 1 and deliver to
the quadriceps tendon, at point 4 [16].
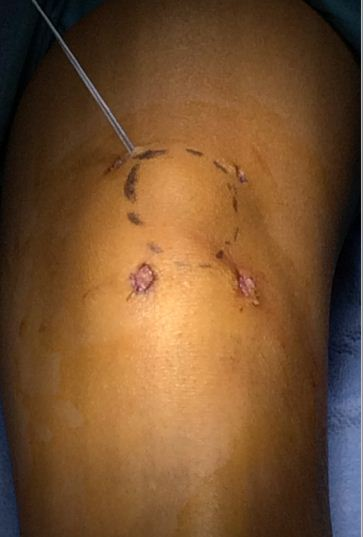
Figure 6: Sutures ready to tension and tie at point 4 with
figure-of-8 tension band complete. All adhesions released
through each of the four small incisions [16].
It is essential that small tenotomy scissor is placed into each of the four incisions freeing the bursa from the tension band suture. Once all skin adhesions were clearly released, the four small incisions were closed, each with a single nylon suture [16]. Intraoperative fluoroscopy was used to confirm reduction in cases of more significant displacement or comminution.
Results
All patients went on to heal without displacement. The average time to bone union was 14.7 weeks (11-24). No patient had symptomatic fixation and no patient required figure-of-8 suture loop or suture knot removal. All patients had a symmetric range of motion established within 10 degrees of the uninjured knee. There were no infections, wound complications, pre-patellar bursitis, or other post-operative complications.
The average time to final follow-up was on average 7.5 months (3-16). At final follow-up, there was no sign of post-traumatic arthritis. At final follow-up, no patient required a second surgery or further treatment for the healed patella fracture. All patients had acceptable range of motion, and there was no case of arthrofibrosis. All patients were able to obtain full extension and all patients were able to obtain flexion within 10 degrees of the contralateral knee.
Discussion
We previously describe a case report of a transverse distal patella fracture successfully treated with a minimally invasive percutaneous technique along with a non-metallic suture, figure-of-8 and tension band [16]. This series of 10 patients successfully utilized this same patella fixation technique with a variety of minimally displaced transverse fractures and one comminuted fracture. All patients achieved fracture union. No patient had displacement of the reduced fracture. No patient required fixation suture removal. All patients achieved acceptable range of motion with no cases of arthrofibrosis. There was no need for secondary surgery in all cases. There was no evidence of post-traumatic arthritis at final follow-up.
This series of 10 patients demonstrates both the advantages of suture fixation and the advantages of percutaneous fixation. The suture fixation minimize the chance of a second surgery to remove symptomatic metallic hardware. The percutaneous technique avoids wide surgical incisions which can be associated with a higher probability of postoperative adhesions [1], prolonged disability for work, as well as a skin scar formation [17]. The percutaneous surgical technique preserves the vascular supply of patellar fragments, which may improve fracture consolidation.
There are limitations to this technique. The importance of a congruent anatomic reduction is of primary importance. Only certain fractures, that are minimally displaced, are amenable to this technique. In many cases, it could be argued that these same cases could be treated non-operatively. However, the advantage of surgical internal fixation is that it allows immediate mobilization, thus minimizing the risk of complications associated with prolonged immobilization.
The other limitation of the study was the limited time of follow-up, especially in how that might relate to the development of post-traumatic arthritis. Nevertheless, the significance of this study relates to the success of the introduction of this minimally invasive technique with no obvious morbidity or complication.
References
- Appel MH and Seigel H. “Treatment of transverse fractures of the patella by arthroscopic percutaneous pinning”. Arthroscopy 9.1 (1993):119–121.
- Bostrom A. “Fracture of the patella. A study of 422 patellar fractures”. Acta orthopaedica Scandinavica 143 (1972):1–80.
- Catalano JB., et al. “Open fractures of the patella: long-term functional outcome”. Journal of Trauma 39 (1995): 439–444.
- Camarda L., et al. “Fiber Wire tension band for patella fractures”. Journal of Orthopaedics and Traumatology 17.1 (2016): 75-80.
- Carpenter JE., et al. “Biomechanical evaluation of current patella fracture fixation techniques”. Journal of Orthopaedic Trauma 11.5 (1997): 351–356.
- Chatakondu SC., et al. “The use of no absorbable suture in the fixation of patellar fractures: a preliminary report”. Injury 29.1 (1998): 23–27.
- Chen CH., et al. “Transosseous suturing of patellar fractures with braided polyester—a prospective cohort with a matched historical control study”. Injury 44.10 (2013):1309–1313.
- Cho B. “Percutaneous Cannulated Screws with Tension Band Wiring Technique in Patella Fractures”. Knee Surgery & Related Research 25.4 (2013): 215-219.
- Gosal HS., et al. “Clinical experience of patellar fracture fixation using metal wire or non-absorbable polyester—a study of 37 cases”. Injury 32 (2001):129–135.
- Hung LK., et al. “Fractured patella: operative treatment using the tension band principle”. Injury 16.5 (1985): 343–347.
- John J., et al. “Tension-band wiring of transverse fractures of patella. The effect of site of wire twists and orientation of stainless steel wire loop: a biomechanical investigation”. International Orthopaedics 31.5 (2007): 703–707.
- Kumar G., et al. “Implant removal following surgical stabilization of patella fracture”. Orthopedics 33.5 (2010).
- Patel VR., et al. “Fixation of patella fractures with braided polyester suture: a biomechanical study”. Injury 31.1 (2000): 1–6.
- Petrie J., et al. “Complications of patellar fracture repair: treatment and results”. Journal of Knee Surgery 26.5 (2013): 309–312.
- Qi L., et al. “Double fixation of displaced patella fractures using bioabsorbable cannulated lag screws and braided polyester suture tension bands”. Injury 42.10 (2011):1116–1120.
- Simonian, PT., et al. “Percutaneous tension-band fixation for distal patella fracture fixation”. MOJ Orthopedics & Rheumatology 8.3 (2017): 00315.
- Smith ST., et al. “Early complications in the operative treatment of patella fractures”. Journal of Orthopaedic Trauma 11.3 (1997):183–187.
- Tandogan RN., et al. “Arthroscopic-assisted percutaneous screw fixation of select patellar fractures”. Arthroscopy 18.2 (2002):156–162.
- Weber MJ., et al. “Efficacy of various forms of fixation of transverse fractures of the patella”. Journal of Bone and Joint Surgery 62 (1980): 215–220.
- Wright PB., et al. “Fiber Wire is superior in strength to stainless steel wire for tension band fixation of transverse patellar fractures”. Injury 40.11 (2009):1200–1203.
Citation:
Lauren E Simonian., et al. “Percutaneous Figure-of-8, Tension-Band Suture Technique for Patella Fracture Fixation”. Orthopaedic
Surgery and Traumatology 2.5 (2018): 387-393.
Copyright: © 2018 Lauren E Simonian., et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.



































 Scientia Ricerca is licensed and content of this site is available under a Creative Commons Attribution 4.0 International License.
Scientia Ricerca is licensed and content of this site is available under a Creative Commons Attribution 4.0 International License.