Case Report
Volume 2 Issue 2 - 2018
An Unusual Case Report of Septic Polyarthritis with Underlying Immunodeficiency Disorder
B.J Medical college, Ahmedabad
*Corresponding Author: Shubham Jain, B.J Medical college, Ahmedabad.
Received: May 29, 2018; Published: June 29, 2018
Abstract
Introduction: Although very frequently we come across cases of septic arthritis in clinical practice we present to you a case of 14 years old with disseminated staph aureus infection with multiple joint septic arthritis with underlying immuno deficiency disorder.
Case Report: A 12 year old female presented with high grade fever, swelling over right knee, dorsum of hand, which later progressed to right shoulder sonography of right knee suggested joint effusion which was followed by frank pus was drained by joint tapping following which patient was taken up for urgent arthrotomy of knee joint and I\D of abscess over dorsum of right hand followed by broad spectrum i.v antibiotics patient was then investigated for cause of septic arthritis which revealed disseminated staph aureus infection with underlying immunodeficiency disorder.
Conclusion: Septic arthritis is a sinister condition that can proceed at a rapid rate. However the correct diagnosis and prompt treatment of this serious condition is necessary as its complications can lead to permanent joint impairment and can even lead to death.
Keywords: Septic Arthritis; Disseminated Staph Aureus Infection; Immuno Deficiency Disorder
Introduction
Acute septic arthritis can occur at any age, but young children and elderly adults are most susceptible, especially if they have an already abnormal joint from previous trauma or from conditions such as hemophilia, osteoarthritis, or rheumatoid arthritis. Immune compromise for any reason and diseases such as cancer, diabetes, alcoholism, cirrhosis, and uremia increase the risk for infection. Usually, predisposing conditions are associated with particular types of causative organisms.
| Clinical factor | ||
| Age | Neonate | Staphylococcus aureus |
| <2 years | Haemophilus influenzae | |
| >2 years | Staphylococcus aureus | |
| Young adults | Neisseria gonorrhoeae, Staphylococcus aureus | |
| Elderly | Staphylococcus aureus (50%) streptococci, gram-negative bacilli |
|
| Prosthesis | Early- S. epidermidis | |
| Late- Gram-positive cocci, anaerobes | ||
| Medical Conditions | Injecting drug use: Atypical gram-negative bacilli (e.g., Pseudomonas species) | |
| Rheumatoid arthritis: S. aureus Systemic lupus erythematosus, sickle cell anemia: Salmonella species |
||
| Immunosupression | S. aureus, Mycobacterium species, fungi | |
Accurate diagnosis can be particularly challenging in patients with underlying immunodeficiency disorder. Septic arthritis occurs most frequently in adults; however, the most serious sequelae from infection occur in children, especially if a hip joint is involved, and treatment has been delayed. Age-dependent anatomical variables may be responsible for the serious complications in children, such as destruction of the epiphysis and associated osteonecrosis from increased intracapsular pressure and septic effusion.
Using immature models, Alderson., et al. provided evidence that trans epiphyseal vessels do exist and provide a direct connection between the physis and epiphyseal cartilage, supplying a route for bacteria to spread from an osteomyelitis focus in the metaphysis to the epiphysis and subsequently to the joint space.
The lower extremity weight bearing joints are predominantly affected (61% to 79%); however, any joint can be involved, and multiple joint infections do occur. A thorough examination to determine if there is monarticular or polyarticular infection is necessary before treatment is initiated. Inflammation of a single joint can be caused by numerous diseases (Box 17-1). Joint sepsis should be an early consideration, however, because failure to diagnose this condition promptly may result in irreversible joint damage or death.
Case Presentation
In November 2017 a 14 yr old female presented to civil hospital with 7 days history of high grade fever, swelling over dorsum of right hand, let knee swelling was warm, tender tense with all the characteristics of an inflammatory pathology. Radiography was insignificant. Routine investigations revealed significantly high counts, knee effusion was then aspirated following local part ultrasonography which also revealed significant joint effusion on aspiration frank pus was drained following which patient was taken for urgent arthrotomy of knee joint with thorough debridement , incision and drainage of abscess over dorsum of hand was done all pus collection was sent for culture and sensitivity , live probe assay (L.P.A gene analysis ) for tubercle bacilli LPA was negative ruling out T.B as a cause for suppuration.
Culture revealed staph aureus sensitive to most of 1st line antibiotics accordingly patient was put on respective i.v antibiotics despite which patient was not improving and started developing cough, swelling over right shoulder. X ray chest revealed disseminated military nodules.
HTCT thorax:
- Multifocal areas of abscess
- Multiple soft tissue nodules and cavitation’s
- Moderate pleural fluid
- Axillary lymph nodes
Diverting the attention back on tuberculosis as an etiology following which patient was put on empirical AKT cat I awaiting culture for tubercle bacilli simultaneously patient was also on i.v antibiotics for staph aureus patient was then investigated for disseminated infection in a 14 year old which revealed significantly decreased IgG levels 2.83gm\dl suggesting primary immunodeficiency disorder with disseminated staph aureus infection.
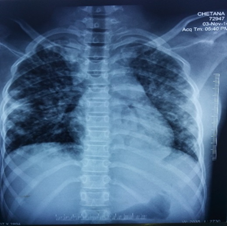
Figure 4: Chest Radiograph Showing Disseminated Millets like Picture, A Feature of Disseminated Staph Aureus Infection.
Discussion
Acute septic arthritis results from bacterial invasion of a joint space, which can occur through hematogenous spread, direct inoculation from trauma or surgery, or contiguous spread from an adjacent site of osteomyelitis or cellulitis. Despite in-depth research into the pathophysiology and treatment of acute septic arthritis, the morbidity and mortality are still significant, especially in patients at the extremes of age. The bacterial strain and the individual's immune system determine whether a septic joint or a less severe infection develops which clearly explains why this patient with immunodeficiency disorder developed fulminant and disseminated arthritis. The collagen receptors found on Staphylococcus aureus (the most common nongonococcal infecting cause of hematogenous septic arthritis) may play a role. Also, the lack of a limiting basement membrane in the capillaries of synovium may allow intravascular bacteria to reach the extravascular space of synovial tissue through gaps between capillary endothelial cells. In addition, synovial fibroblasts inhibit phagocytosis of bacteria.
Alderson., et al. provided evidence that Trans epiphyseal vessels do exist and provide a direct connection between the physis and epiphyseal cartilage, supplying a route for bacteria to spread from an osteomyelitis focus in the metaphysis to the epiphysis and subsequently to the joint space. Delay in diagnosis and failure to begin treatment promptly are the most common reasons for late complications of infection and hence a prompt diagnosis of septic joint arthritis should be made which can clinically be made by just aspirating the effused involved joint followed by microscopic examination of the fluid in this particular case we promptly diagnosed the patient with septic arthritis but still patient did not improve on appropriate antibiotics which further necessitated to investigate any other underlying condition and was found to be primary immunodeficiency disorder patient was suffering from patient then improved dramatically with combined antibiotics and immunoglobulins.
Conclusion
Patients who present to a clinic with a recent onset of joint effusion, pain, severe tenderness, global restriction of movement of the affected joint and with systemic features of infection, even if radiographs appear normal should be strongly suspected for septic arthritis and should be treated without any delay septic arthritis is a sinister condition that can proceed at a rapid rate. However the correct diagnosis and prompt treatment of this serious condition is necessary as its complications can lead to permanent joint impairment and can even lead to death.
References
- Kaandorp CJ., et al. “The outcome of bacterial arthritis: a prospective community-based study”. Arthritis & Rheumatism 40.5 (1997): 884-892.
- Nilsson IM., et al. “Role of the staphylococcal accessory gene regulator (sar) in septic arthritis”. Infection and Immunity 64.11 (1996): 4438–4443.
- Cunningham R., et al. “Clinical and molecular aspects of the pathogenesis of Staphylococcus aureus bone and joint infections”. Journal of Medical Microbiology 44.3 (1996): 157–164.
- Forrester DM and Feske WI. “Imaging of infectious arthritis”. Seminars in Roentgenology 31 (1996): 239–249.
- Hughes RA., et al. “Septic bone, joint and muscle lesions associated with human immunodeficiency virus infection”. British Journal of Rheumatology 31.6 (1992): 381–388.
- Pitkin AD and Eykyn SJ. “Covert multi-focal infective arthritis”. Journal of Infection 27 (1993): 297–300.
- Fink CW and Nelson JD. “Septic arthritis and osteomyelitis in children”. Clinics in Rheumatic Diseases 12 (1986): 423-435.
- Churman DJ and Smith RL. “Surgical approach to the management of septic arthritis”. Orthopedic Reviews 16.4 (1987): 241-245.
Citation:
Shubham Jain. “An Unusual Case Report of Septic Polyarthritis with Underlying Immunodeficiency Disorder”. Orthopaedic
Surgery and Traumatology 2.2 (2018): 314-318.
Copyright: © 2018 Shubham Jain. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.



































 Scientia Ricerca is licensed and content of this site is available under a Creative Commons Attribution 4.0 International License.
Scientia Ricerca is licensed and content of this site is available under a Creative Commons Attribution 4.0 International License.