Review Article
Volume 2 Issue 1 - 2018
A Review: Bone Marrow Homing Molecular Mechanisms of Stem Cells
University of Antwerpen, Antwerp, Belgium
*Corresponding Author: Alemu Aylate, University of Antwerpen, Antwerp, Belgium.
Received: February 23, 2017; Published: March 01, 2018
Abstract
Homing of hematopoietic stem cells (HSC) to their microenvironment niches in the bone marrow (BM) is a rapid and complex process occurring within hours with a critical role in repopulation of the bone marrow after transplantation. Thus, homing of HSC is a prerequisite for their repopulation and engraftment. It involves three consecutive steps: extravasation from peripheral blood through the BM endothelium, migration through stroma, and lodgement into niches. Migration of hematopoietic stem cells to the bone marrow is a highly regulated process that requires correct regulation of the expression and activity of various molecules including adhesion molecules, chemokines, cytokines and proteolytic enzymes.
Currently, hematopoietic stem cell transplantations are serving as the most powerful treatment modality for many hematopoietic malignancies. Indeed, successful hematopoietic recovery after transplantation depends on homing of hematopoietic stem cells to the bone marrow and subsequent lodging of those cells in specific niches in the bone marrow. CXCL12-CXCR4 signalling was demonstrated to play an essential role in the BM homing of HSCs. Likewise, a correct regulation of PI3K/PKB is crucial for migration of HSCs to the bone marrow after transplantation. This mini-thesis is a short review of recent literatures about the molecular mechanisms underlying adhesion, migration and bone marrow homing of hematopoietic stem cells.
Keywords: BM; HSCs; Homing; Molecular mechanisms
Introduction
Hematopoietic stem cells (HSCs) are the foundation of the vertebrate blood system. In mammals, hematopoiesis is a complex and highly ordered process in which a HSC gives rise to all differentiated blood cells. During adult life this process is closely linked to a specialized environment, called niches, in the bone marrow (BM) (Clements and Traver, 2013). However, aberrant regulation of hematopoiesis can result in the development of various forms of cancers, bone marrow failure, hereditary metabolic disorders and severe congenital immuno-deficiencies (Lapidot., et al. 2005).
Recently, emerging field of regenerative or gene HSC-based therapy become a huge potential for the cure of numerous congenital and acquired diseases. There has been a rapid surge in clinical trials involving HSC therapies that continued to demonstrate the importance of stem cells both in replacing damaged tissue and in providing extracellular factors capable of promoting endogenous cellular salvage and replenishment (Vanhee and Vandekerckhove, 2016).
Thus, hematopoietic stem cell transplantation has become the standard of care for the treatment of many hematologic malignancies, chemotherapy sensitive relapsed acute leukemias or lymphomas, multiple myeloma and for some non-malignant diseases such as aplastic anemia and immunodeficient states. But, successful hematopoietic recovery after transplantation depends on homing of transplanted hematopoietic stem cells to interact with their niches for re-establishment and repopulation to the recipient BM (Lapidot., et al. 2005).
Hence, homing is a phenomenon whereby transplanted hematopoietic cells can travel to and engraft or establish residence in the bone marrow that relies on intracellular signalling and interaction between chemokines, chemokine receptors, adhesion molecules, and proteases to promote HSC adhesion to micro-vessels (Lapidot., et al. 2005). Cells start rolling and firmly adhered to endothelial cells in the bone marrow sinusoids. Then cells migrate across endothelium matrix barrier to anchor and lodge to their specialized niches within the bone marrow compartments (Lo Celso and Fleming, 2009).
Indeed, HSC homing is the mirror image of mobilization. In homing, it involves sequential events that allow HSC to reach their niches within bone marrow. On the other hand, mobilization follows a reversal steps required for stem cell to come out of BM and enter the peripheral blood following administration of growth factors and/or chemotherapeutic agents.
Despite the central role these phenomena play in stem cell biology and cancer therapy, processes governing trafficking, migration and homing of HSC to the BM, and their egress from the marrow into the periphery, both at the molecular and cellular levels, remain poorly understood. Equally ambiguous at present, is the immediate fate of stem cells arriving in the BM shortly after transplantation. Therefore, this review present HSCs homing with a focus on most important aspects of recent insights into the molecular mechanisms underlying adhesion, migration and bone marrow homing.
Molecular Mechanisms Underlying Bone Marrow Homing Of Hscs
The Role of Adhesion molecules
Cell adhesion receptors including selectins, integrins and CD34 are thought to play a key role both in migration of HSCs during embryogenesis and retention of adult HSCs in the BM environment. Except L-selectin, both P-endothelial and E-endothelial selectin plays an important role in bone marrow homing of hematopoietic stem cells during initial tethering and rolling steps on BM micro-vessels (Xia and McDaniel, 2004; Pouget, 2014) (Figure 1).
The Role of Adhesion molecules
Cell adhesion receptors including selectins, integrins and CD34 are thought to play a key role both in migration of HSCs during embryogenesis and retention of adult HSCs in the BM environment. Except L-selectin, both P-endothelial and E-endothelial selectin plays an important role in bone marrow homing of hematopoietic stem cells during initial tethering and rolling steps on BM micro-vessels (Xia and McDaniel, 2004; Pouget, 2014) (Figure 1).
In the next step of trans-endothelial migration, however in contrast to fluid-phase P- and E-selectin, (Xia and McDaniel, 2004), adhesion of CD34+ hematopoietic progenitor cells to bone marrow derived endothelial cells under static conditions has been shown not to depend on E-selectin. Experiments performed to study the importance of E-selectin in trans-endothelial migration of human hematopoietic progenitor cells yielded contradictory results (Naiyer and Jo., et al. 1999).
Trans well experiments performed by Voermans and Rood (2000), for example, suggested that E-selectin is not important for trans-endothelial migration. Transplantation of lethally irradiated recipient mice deficient for both P-and E-selectin with wild type bone marrow cells resulted in reduced recruitment of hematopoietic progenitors to the bone marrow and enhanced levels of circulating hematopoietic progenitors, indicating that selectins indeed play an important role in bone marrow homing (Forde and Tye, 2007).
Similarly, heterodimeric transmembrane molecules called integrins that consists an α and β subunit that play an important role in HSC adhesion, trans-endothelial migration and regulation of bone marrow homing (Merzaban and Burdick, 2011). Zanjani., et al. (1999) demonstrated that CD49d/CD29 or α4β1 or Very late antigen-4 (VLA-4) played a central role in homing and engraftment of transplanted human cells to the BM of sheep foetuses and that migration of transplanted cells to foetal liver in lieu of the BM could be positively modulated with anti-β1 integrin antibody.
In vitro studies with blocking antibodies have, for example, shown that both CD49d/CD29 or α4β1 or VLA-4 and CD11a/CD18 or αLβ2 or lymphocyte function-associated molecule-1 (LFA-1), but not CD49e/CD29 or α5β1 or VLA-5, play an important role in adhesion of hematopoietic stem and progenitor cells to endothelial cells and subsequent trans-endothelial migration (Voermans and Rood, 2000; Peled and Kollet, 2000).
Furthermore, several studies have reported that α4β1/ligand interaction contributes to cellular tethering and rolling (Voermans and Rood, 2000). Additionally, it has been shown that the homing ability of normal donor cells decreases after treatment with anti-α4β1 (Ibbotson., et al. 2001). Further evidence suggesting the involvement of α4β1-integrin in the homing process is given in the points below (Burger and Spoo, 2003; Lapidot., et al. 2005):
- α4β1 is widely expressed in both stem and progenitor cells, exceeding expression of both L-selectin and β2-integrin taken together;
- α4β1 is constitutively active in HSC and progenitor cells;
- α 4β1 is usually inactive in committed cells.
Another important role in HSC homing has been assigned to intercellular adhesion molecule-1 (ICAM-1) and vascular cell adhesion molecule-1 (VCAM-1) (Figure 1). These two molecules have been shown to act as key factors in cell trafficking between blood and BM (Peled and Kollet, 2000). The main ligand of α4β1 in committed cells is VCAM-1. Therefore, it can be reasonably assumed that all functions are likely to be accomplished through their interactions (Xia and McDaniel, 2004).
Source: Caocci., et al. 2017
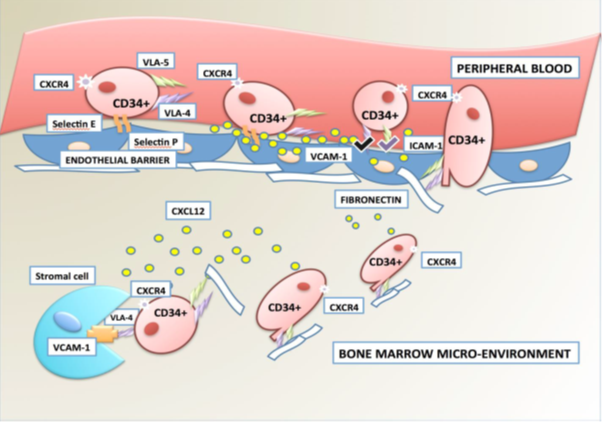
Figure 1: Migration and homing of HSCs into the bone marrow microenvironment. E- Endothelial and P- endothelial selectin were found to be important to cell movement (cell rolling) and promote weak HSC adhesion to bone marrow microvessels. The expression of the chemokine receptor CXCR4 on the HSC surface promotes cell activation via CXCL12 factor. Following stronger interaction between LFA-1/ICAM-1 and VLA-4/VCAM-1, HSCs arrest on the endothelial surface and migrate through basal lamina. The migration is also promoted by VLA-4 and VLA-5 interaction with fibronectin, present in the extracellular matrix.
Figure 1: Migration and homing of HSCs into the bone marrow microenvironment. E- Endothelial and P- endothelial selectin were found to be important to cell movement (cell rolling) and promote weak HSC adhesion to bone marrow microvessels. The expression of the chemokine receptor CXCR4 on the HSC surface promotes cell activation via CXCL12 factor. Following stronger interaction between LFA-1/ICAM-1 and VLA-4/VCAM-1, HSCs arrest on the endothelial surface and migrate through basal lamina. The migration is also promoted by VLA-4 and VLA-5 interaction with fibronectin, present in the extracellular matrix.
The Role of Chemoattractants in the migration of HSCs
Chemoattractant play an important role in directing migration of hematopoietic stem and progenitor cells to the bone marrow. Several studies have demonstrated that Stromal-derived factor-1 (SDF-1), also known as CX chemokine ligand 12 (CXCL12) (Tashiro and Tada, 1993) acts as a chemoattractant for hematopoietic stem and progenitor cells during their trans-endothelial migration (Broxmeyer and Orschell, 2005; Glass and Lund, 2011).
Chemoattractant play an important role in directing migration of hematopoietic stem and progenitor cells to the bone marrow. Several studies have demonstrated that Stromal-derived factor-1 (SDF-1), also known as CX chemokine ligand 12 (CXCL12) (Tashiro and Tada, 1993) acts as a chemoattractant for hematopoietic stem and progenitor cells during their trans-endothelial migration (Broxmeyer and Orschell, 2005; Glass and Lund, 2011).
Further investigation, utilizing a large panel of CC and CXC chemokines, suggested that the only chemokine capable of inducing migration of murine hematopoietic stem and progenitor cells appears to be SDF-1 (Liesveld and Rosell., 2001; Wright and Bowman, 2002). Although the chemokine receptors CCR3 and CCR9 were also expressed at mRNA level, their ligands could not induce migration (Wright and Bowman, 2002). Similarly, examination of a panel of chemokines and cytokines in trans-endothelial migration assays revealed that SDF-1 is also important for migration of human hematopoietic progenitors through a confluent layer of endothelial cells (Liesveld and Rosell, 2001).
However, to a lesser extent, also other chemokines and cytokines, including CCL2 (MCP-1), CCL5 (RANTES), CXCL10 (IP-10), IL-8 and SCF could also induce trans-endothelial migration (Liesveld and Rosell., 2001). In addition, LTD4, a ligand for CysLT(1), a G protein-coupled receptor recognizing inflammatory mediator of the cysteinyl leukotriene family, which is highly expressed in hematopoietic progenitors, has been demonstrated to up-regulate α4β1 and αLβ2 dependent adhesion of hematopoietic progenitors and to induce chemotaxis and in vitro trans-endothelial migration (Bautz and Denzlinger, 2001; Boehmler and Drost, 2009).
Recently, a role for the proteolysis-resistant bioactive lipids sphingosine-1-phosphate and ceramide-1-phosphate in regulation of bone marrow homing has been suggested. Conditioning of mice for transplantation resulted in enhanced levels of these lipids in the bone marrow. In addition, both lipids appear to be chemoattractant for hematopoietic stem and progenitor cells (Kim and Wu, 2011).
The Role of SDF-1 in the bone marrow homing of HSCs
Stromal cell-derived factor (SDF-1) also known as CXC chemokine ligand (CXCL) 12 or pre-B-cell-growth stimulating factor [PBSF]) is a member of a large family of structurally related chemo-attractive cytokines and was first characterized as a growth-stimulating factor for the B cell precursor clone (Nagasawa, 2006). The primary physiologic receptor for SDF-1 or CXCL12 is CXCR4. Signalling of CXCL12-CXCR4 is essential in adult bone marrow to maintain the HSC pool and suggest that many HSCs are in contact with a small population of reticular cells expressing high amounts of CXCL12 (Tokoyoda., et al. 2004; Nagasawa, 2006). CXCL12 chemokine gradient, produced by BM niche cells, attracts transplanted HSCs, which first attach to and roll over the endothelium, followed by their penetration of the tissue via trans-endothelial migration.
Stromal cell-derived factor (SDF-1) also known as CXC chemokine ligand (CXCL) 12 or pre-B-cell-growth stimulating factor [PBSF]) is a member of a large family of structurally related chemo-attractive cytokines and was first characterized as a growth-stimulating factor for the B cell precursor clone (Nagasawa, 2006). The primary physiologic receptor for SDF-1 or CXCL12 is CXCR4. Signalling of CXCL12-CXCR4 is essential in adult bone marrow to maintain the HSC pool and suggest that many HSCs are in contact with a small population of reticular cells expressing high amounts of CXCL12 (Tokoyoda., et al. 2004; Nagasawa, 2006). CXCL12 chemokine gradient, produced by BM niche cells, attracts transplanted HSCs, which first attach to and roll over the endothelium, followed by their penetration of the tissue via trans-endothelial migration.
The concentration of (SDF-1 ligand which increases in the BM microenvironment after conditioning regimens plays an important role in HSC homing during transplantation (Lapidot., et al. 2005; Yin., 2006) (Figure 1). SDF-1 is a chemokine that interacts as a ligand with the G-protein coupled receptor CXCR4, promoting HSC quiescence and survival. The expression of the chemokine receptor CXCR4 on the HSC surface promotes migration and homing into or from the BM (Asri., et al. 2016).
For instance, mouse embryos knocked out for SDF-1 or CXCR4 show multiple lethal defects, as well as the absence of BM homing by HSCs. Activation of the CXCR4 receptor by SDF-1 is one of the transductional axes most studied in recent years because of its fundamental importance in regulating trafficking of HSCs to and from the BM. It has also been reported that CXCR4-depleted human cells are insensitive to mobilization with agonists or antagonists of the CXCR4 receptor (Liles., et al. 2003; Desmond and Dunfee., 2011).
SDF-1-CXCR4 interaction triggers chemotaxis via intracellular GTPase proteins (heterotrimeric G-proteins, typically Gαi subunits) (Papayannopoulou., et al. 2003). After binding to SDF-1, CXCR4 undergoes down-modulation and ubiquitination of the C-terminus (C-ter) by E3 ubiquitin ligase, in this way promoting receptor degradation or it’s recycling via the endosomal pathway (Marchese et al., 2003).
Other potential factors involved in the homing process are the extracellular nucleotides (eNTPs), such as adenosine triphosphate (ATP) and uridine triphosphate (UTP), recently described as having a fundamental role in the modulation of HSC migration in the presence of SDF-1. Since extracellular UTP improves HSC migration toward SDF-1 gradients, pre-treatment with eUTP, it is likely to increase homing of HSCs to the BM significantly as has been demonstrated in immunodeficient mice (Rossi., et al. 2007). The aforesaid eNTPs act through P2 nucleotide receptors (P2Rs); particularly P2YRs. These seven transmembrane-spanning receptors, also referred to as G-protein coupled receptors, activate their signal transduction pathway via activation of phospholipase C or activation/inhibition of adenylate cyclase (Di Virgilio., et al. 2001; Kollet and Dar, 2006).
Although the influence of SDF-1 on HSC chemotactic responses has been well established, its role in the different molecular pathways underlying the early stages of homing remains a highly discussed and contentious issue. Indeed, evidence has been produced of HSC homing to the BM independent of the SDF-1–CXCR4 axis (Brenner., et al. 2004; Kahn and Byk, 2004 ;). Several observations support this evidence. Adamiak (2015) and colleagues recently confirmed the involvement of the bioactive phosphosphingolipid sphingosine-1-phosphate (S1P) as a potent chemotactic factor for HSCs. They performed hematopoietic transplantation in mice deficient in BM-expressed sphingosine kinase 1 (Sphk1−/−), using HSCs from normal control mice as well as mice in which floxed CXCR4 (CXCR4fl/fl) had been conditionally deleted.
They found that homing and engraftment in the Sphk1−/− mice was defective after transplantation of CXCR4−/− BM cells, indicating that SIP expressed in the BM microenvironment was involved in the homing process. Thus, SIP levels in the BM are regulated by a balance in activity between type 1 SP-1 kinase (Sphk1) and S1P lyase, which has the role of degrading S1P (Ratajczak., et al. 2013). Since 2013, it has been observed that S1P is a potent chemoattractant for HSCs, much stronger than SDF-1 (Adamiak., et al. 2015).
In addition, it has also been suggested that HSC homing could be improved by inhibiting membrane-bound extracellular peptidase CD26 protein (DPPIV/dipeptidyl peptidase IV). Peptidase CD26 removes dipeptides from the amino terminus of proteins, and it is has been demonstrated that endogenous CD26 expression on donor cells downregulates homing and engraftment. Therefore, it can be reasonably assumed that by deleting or inhibiting CD26, it would be possible to increase HSC transplantation efficiency (Hattori and Heissig, 2002).
Besides the BM microenvironment, other individual genetic factors can have an impact on successful engraftment of HSCs. For example, HSC homing is influenced by several molecules involved in inflammatory and other signalling pathways of innate immune response (Orrù., et al. 2012). Ratajczak and his colleagues describe how innate immunity derived factors are external modulators of the SDF-1–CXCR4 axis. Because SDF-1 is extremely susceptible to degradation by proteolytic enzymes, its availability in biological fluids may be somewhat limited.
However, the authors observed that at a minimum near threshold doses, SDF-1 was still able to exert a robust chemotactic influence on engraftment. They showed that chemotactic responsiveness of HSCs to several different types of homing gradients could be modulated by ex vivo manipulations, using a strategy that takes advantage of a hematopoietic stem and progenitor cell (HSPC), a priming approach. Homing of HSPCs can be enhanced by ex vivo cell exposure to C3a (cleavage fragments of the third protein component of the complement cascade). (Ratajczak., et al. 2013).
The Role of PI3K/PKB signalling module in homing of HSCs
Correct regulation of the PhosphatidyLinositol-3-Kinase (PI3K)/Protein Kinase B (PKB/c- Akt) signaling module is essential for multiple processes during hematopoiesis. Phosphatidylinositol 4, 5 bisphosphate (PI (4, 5) P2), the most important substrate for PI3K, can be phosphorylated upon extracellular stimulation, resulting in the formation of phosphatidylinositol 3, 4, 5 trisphosphate (PI (3, 4, and 5) P3) (Hawkins and Anderson, 2006). PI (3, 4, and 5) P3 subsequently serves as an anchor for Pleckstrin Homology (PH) domain-containing proteins, like Protein Kinase B (PKB/c-akt). Activation of PI3K and its downstream effector Protein Kinase B (PKB/c-Akt) has been observed in leukemic cell lines stimulated with SDF-1 (Fuhler and Drayer, 2008). A positive role for PI3K/PKB in regulation of SDF-1 induced migration of hematopoietic stem cells was therefore suggested.
Correct regulation of the PhosphatidyLinositol-3-Kinase (PI3K)/Protein Kinase B (PKB/c- Akt) signaling module is essential for multiple processes during hematopoiesis. Phosphatidylinositol 4, 5 bisphosphate (PI (4, 5) P2), the most important substrate for PI3K, can be phosphorylated upon extracellular stimulation, resulting in the formation of phosphatidylinositol 3, 4, 5 trisphosphate (PI (3, 4, and 5) P3) (Hawkins and Anderson, 2006). PI (3, 4, and 5) P3 subsequently serves as an anchor for Pleckstrin Homology (PH) domain-containing proteins, like Protein Kinase B (PKB/c-akt). Activation of PI3K and its downstream effector Protein Kinase B (PKB/c-Akt) has been observed in leukemic cell lines stimulated with SDF-1 (Fuhler and Drayer, 2008). A positive role for PI3K/PKB in regulation of SDF-1 induced migration of hematopoietic stem cells was therefore suggested.
However, it has been shown that Protein Phosphatase 2A plays an important role in positively regulating SDF-1 mediated migration of human hematopoietic progenitors by inhibiting PKB activity (Basu and Ray, 2007). Similarly, inhibition of PKB activity in CD34+ cells for over 24 hours appears to be sufficient to reduce their adhesion to bone marrow derived stromal cells and to induce their basal migratory capacity (Buitenhuis and Van Dder Linden, 2010).
Transwell migration experiments through a confluent layer of human umbilical vein endothelial cells revealed that the observed reduction in firm adhesion does not ameliorate the induced migratory capacity of CD34+ cells pre-treated with a PKB inhibitor (Buitenhuis and Van Dder Linden, 2010). In addition, ectopic expression of constitutively active PKB in CD34+ cells conversely induced firm adhesion and reduced the basal level of migration.
Although it cannot be excluded that transient activation of PI3K/PKB activity by SDF-1 is important for induction of migration, these studies suggest that prolonged activation of PKB activity is detrimental for migration of CD34+ cells (Maehama and Dixon, 1998; Zhang and Grindley, 2006). SH2-containing inositol-5'-phosphatase (SHIP) and Phosphate and Tensin Homologue (PTEN) are critical negative regulators of PI3K signaling in bone marrow regulation (Davis and Singer, 2005; Desponts and Hasen, 2006; Buitenhuis., et al. 2008).
Several studies demonstrated that correct regulation of PI3K/PKB is essential for migration of hematopoietic stem and progenitor cells to the bone marrow after transplantation, which is essential for optimal engraftment and hematopoietic recovery (Buitenhuis and Van Dder Linden, 2010; Desponts and Hasen, 2006; Kharas and Okabe, 2010).
As described above, adhesion and migration of HSCs depend on correct integrin and selectin expression and regulation of integrin activity. PKB and its downstream effector GSK-3 have initially been shown to play an important role in recycling of the CD49e/CD29 and CD51/CD61 (αvβ3) integrins to the membrane in NIH 3T3 fibroblasts, resulting in enhanced cell spreading and adhesion (Roberts and Woods, 2004). Ectopic expression of PKB in human hematopoietic stem and progenitor cells has been demonstrated to enhance the level of CD49d, while inhibition of PKB activity conversely reduces expression of both CD49d and CD18 (Buitenhuis and Van Dder Linden, 2010), providing a potential mechanism by which PKB induces adhesion and inhibits migration. Although it is evident that integrins play an important role in adhesion and migration of cells, the importance of these molecules in PKB mediated inhibition of migration remains to be investigated. In addition, CXCR4 expression has been demonstrated to be reduced in SHIP deficient hematopoietic stem cells, suggesting that activation of PI3K also impairs their response to SDF-1(Zhang., et al. 2006).
Source: Caocci., et al. 2017
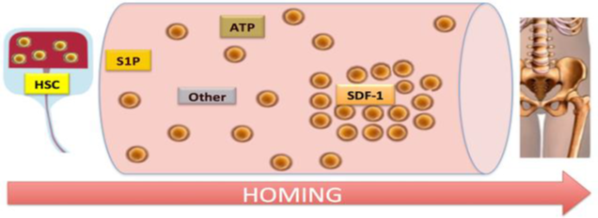
Figure 2: Schematic representation of HSC homing. HSCs infused into blood are more responsive to stromal cell-derived factor (SDF)-1 gradient between bone marrow and blood compared to other factors that are upregulated after transplantation conditioning regimen (S1P, ATP).
Figure 2: Schematic representation of HSC homing. HSCs infused into blood are more responsive to stromal cell-derived factor (SDF)-1 gradient between bone marrow and blood compared to other factors that are upregulated after transplantation conditioning regimen (S1P, ATP).
Discussions and Conclusion
Correct regulation of HSC homing to bone marrow after transplantation is required for normal long-term hematopoiesis. It was revealed that homing of HSCs into their specialized niches requires tightly regulated interactions between the progenitors and the microenvironment that provides a suitable condition for their final anchorage (Clements and Traver, 2013). Likewise, subsequent trafficking of human CD34+ stem cells reported to be regulated by adhesion molecules, chemokines, cytokines and proteolytic enzymes (Zhang and Grindley, 2006).
The initial tethering and rolling of hematopoietic stem and progenitor cells along the endothelial wall of blood vessels are primarily regulated by specific selectins, various integrins have been shown to be involved in regulation of the next stages in this process; firm adhesion to the endothelial wall and trans-endothelial migration (Merzaban and Burdick, 2011). Directional migration toward the hematopoietic stem cell niche in the bone marrow requires a chemokine gradient. A chemokine SDF-1 is found to be the most powerful chemoattractant that stimulate rapid and potent HSC adhesion and serve as a directional migration guider (Asri., et al. 2016).
Thus, SDF-1 has been demonstrated to induce the activity of integrins which allows interaction with their substrates. Hence, both CD49d/CD29 and CD11a/CD18 integrins appeared to be involved in mediation of SDF-1 induced directional migration of CD34+ cells through the basal lamina (Buitenhuis and Van Dder Linden, 2010). In fact, regulation of SDF-1 activity by a variety of proteolytic enzymes has been demonstrated to play an important role in migration of hematopoietic stem cells to and from the bone marrow.
Hence, the molecular mechanism underlying SDF-1 mediated regulation of HSC migration has been investigated extensively (Ratajczak., et al. 2013). Various studies showed that ICAM-1 and VCAM-1 play an important role in adhesion of hematopoietic stem and progenitor cells to endothelial cells and subsequent trans-endothelial migration (Peled and Kollet, 2000). Although activation of PI3K and its downstream effector Protein Kinase B has been observed in leukemic cell lines stimulated with SDF-1, suggesting a positive role for PI3K/PKB in regulation of SDF-1 induced migration of HSCs. Several studies described the PI3K/PKB signaling module in playing a critical role in negatively regulating migration of HSCs and bone marrow homing (Buitenhuis and Van Dder Linden, 2010). Despite the many questions that still need to be answered, all these molecules could support a rationale for the development of innovative strategies aimed at improving HSC engraftment.
In conclusion, this review highlighted the molecular basics in BM homing of HSCs which is very essential for better understanding to design novel therapeutic strategies and to apply enhancement of homing properties of other stem cell types which share common migration mechanisms.
References
- Adamiak M., et al. “Evidence for the involvement of sphingosine-1-phosphate in the homing and engraftment of hematopoietic stem cells to bone marrow”. Oncotarget 6.22 (2015):18819-18828.
- Asri A., et al. “Homing in hematopoietic stem cells: focus on regulatory role of CXCR7 on SDF1a/CXCR4 axis”. EXCLI Journal 15 (2016): 134-149.
- Basu S and Ray NT. “Protein phosphatase 2A plays an important role in stromal cell- derived factor-1/CXC chemokine ligand 12-mediated migration and adhesion of CD34+ cells”. Journal of Immunology 179.5 (2007): 3075-3085.
- Bautz F and Denzlinger C. “Chemotaxis and trans-endothelial migration of CD34(+) hematopoietic progenitor cells induced by the inflammatory mediator leukotriene D4 are mediated by the 7-transmembrane receptor CysLT1”. Blood 97.11 (2001): 3433-3440.
- Boehmler AM., et al. “The CysLT1 ligand leukotriene D4 supports alpha4beta1- and alpha5beta1-mediated adhesion and proliferation of CD34+ hematopoietic progenitor cells”. Journal of Immunology 182.11 (2009): 6789-6798.
- Brenner S., et al. “CXCR4-transgene expression significantly improves marrow engraftment of cultured hematopoietic stem cells”. Stem Cells 22.7 (2004): 1128-1133.
- Broxmeyer HE., et al. “Rapid mobilization of murine and human hematopoietic stem and progenitor cells with AMD3100, a CXCR4 antagonist” Journal of Experimental Medicine 2010.8 (2005): 1307-1318.
- Buitenhuis M., et al. “Protein kinase B (c-akt) regulates hematopoietic lineage choice decisions during myelopoiesis” Blood 111.1 (2008): 112-121.
- Buitenhuis M., et al. “Protein kinase B (PKB/c-akt) regulates homing of hematopoietic progenitors through modulation of their adhesive and migratory properties” Blood 116.13 (2010): 2373-2384.
- Burger JA., et al. “CXCR4 chemokine receptors (CD184) and alpha4beta1 integrins mediate spontaneous migration of human CD34+ progenitors and acute myeloid leukaemia cells beneath marrow stromal cells (pseudoemperipolesis)”. British Journal of Haematology 122.4 (2003): 579-589.
- Caocci, Giovanni., et al. “Bone Marrow Homing and Engraftment Defects of Human Hematopoietic Stem and Progenitor Cells”. Mediterranean Journal of Hematology and Infectious Diseases 9.1 (2017).
- Clements WK and Traver D. “Signaling pathways that control vertebrate hae matopoietic stem cell specification”. Nature Reviews Immunology 13.5 (2013): 336-348.
- Davis DA., et al. “Identification of carboxypeptidase N as an enzyme responsible for C-terminal cleavage of stromal cell-derived factor-1alpha in the circulation”. Blood 105.12 (2005): 4561-4568.
- Desmond R., et al. “CD9 up-regulation on CD34+ cells with ingenol 3,20- dibenzoate does not improve homing in NSG mice”. Blood 117.21 (2011): 5774-5776.
- Desponts C., et al. “SHIP deficiency enhances HSC proliferation and survival but compromises homing and repopulation”. Blood 107.11 (2006): 4338-4345.
- Di Virgilio F., et al. “Nucleotide receptors: an emerging family of regulatory molecules in blood cells”. Blood 97.3 (2001): 587-600.
- Forde S., et al. “Endolyn (CD164) modulates the CXCL12-mediated migration of umbilical cord blood CD133+ cells”. Blood 109.5 (2007): 1825-1833.
- Fuhler GM., et al. “Reduced activation of protein kinase B, Rac, and F-actin polymerization contributes to an impairment of stromal cell derived factor-1 induced migration of CD34+ cells from patients with myelodysplasia”. Blood 111.1 (2008): 359-368.
- Glass TJ., et al. “Stromal cell-derived factor-1 and hematopoietic cell homing in an adult zebrafish model of hematopoietic cell transplantation”. Blood 118.3 (2011): 766-774.
- Hattori K., et al. “Plasma elevation of stromal cell-derived factor-1 induces mobilization of mature and immature hematopoietic progenitor and stem cells”. Blood 97.11 (2002): 354-360.
- Hawkins PT., et al. “Signalling through Class I PI3Ks in mammalian cells”. Biochemical Society Transactions 34.5 (2006): 647-662.
- Ibbotson GC., et al. “Functional alpha-4-integrin: a newly identified pathway of neutrophil recruitment in critically ill septic patients”. Nature Medicine 7.4 (2001): 465-470.
- Kahn J., et al. “Overexpression of CXCR4 on human CD34+ progenitors increases their proliferation, migration, and NOD/SCID repopulation”. Blood 103.8 (2004): 2942-2949.
- Kharas MG., et al. “Constitutively active AKT depletes hematopoietic stem cells and induces leukemia in mice”. Blood 115.7 (2010): 1406-1415.
- Kim CH., et al. “Conditioning for hematopoietic transplantation activates the complement cascade and induces a proteolytic environment in bone marrow: a novel role for bioactive lipids and soluble C5b-C9 as homing factors”. Leukemia 26.1 (2012):106-116.
- Kollet O., et al. “Osteoclasts degrade endosteal components and promote mobilization of hematopoietic progenitor cells”. Nature Medicine 12.6 (2006): 657-664.
- Lapidot T., et al. “How do stem cells find their way home?” Blood 106.6 (2005): 1901-1910.
- Liesveld JL., et al. “Response of human CD34+ cells to CXC, CC, and CX3C chemokines: implications for cell migration and activation”. Journal of Hematotherapy and Stem Cell Research 10.5 (2001): 643-655.
- Liles WC., et al. “Mobilization of hematopoietic progenitor cells in healthy volunteers by AMD3100, aCXCR4 antagonist”. Blood 102.8 (2003): 2728-2730.
- Lo Celso C., et al. “Live-animal tracking of individual haematopoietic stem/progenitor cells in their niche”. Nature 457 (2009): 92-96.
- Maehama T and Dixon JE. “The tumor suppressor, PTEN/MMAC1, dephosphorylates the lipid second messenger, phosphatidylinositol 3,4,5-trisphosphate”. Journal of Biological Chemistry 273.22 (1998): 13375-13378.
- Marchese A., et al. “The E3 ubiquitin ligase AIP4 mediates ubiquitination and sorting of the G proteincoupled receptor CXCR4”. Developmental Cell 5.5 (2003): 709-722.
- Merzaban JS., et al. “Analysis of glycoprotein E-selectin ligands on human and mouse marrow cells enriched for hematopoietic stem/progenitor cells”. Blood 118.7 (2011): 1774-1783.
- Nagasawa T. “Microenvironmental niches in the bone marrow for B-cell development”. Nature Reviews Immunology 6.2 (2006): 107-116.
- Orrù S., et al. “Recipient CTLA-4*CT60-AA genotype is a prognostic factor for acute graft-versus-host disease in hematopoietic stem cell transplantation for thalassemia”. Human Immunology 73.3 (2012): 282-286.
- Papayannopoulou T., et al. “The role of G-protein signaling in hematopoietic stem/progenitor cell mobilization”. Blood 101.12 (2003): 4739-4747.
- Peled A., et al. “The chemokine SDF-1 activates the integrins LFA-1, VLA-4, and VLA-5 on immature human CD34 (+) cells: role in trans-endothelial/stromal migration and engraftment of NOD/SCID mice”. Blood 95.11 (2000): 3289-3296.
- Pouget C., et al. “FGF signalling restricts haematopoietic stem cells specification via modulation of the BMP pathway”. Nature Communications 5 (2014).
- Ratajczak MZ., et al. “Innate Immunity Derived Factors as External Modulators of the CXCL12 - CXCR4 Axis and Their Role in Stem Cell Homing and Mobilization”. Theranostics 3.1 (20103): 3-10.
- Roberts MS., et al. “Protein kinase B/Akt acts via glycogen synthase kinase 3 to regulate recycling of alpha v beta 3 and alpha 5 beta 1 integrins”. Molecular Cell Biology 24.4 (2004): 1505-1515.
- Rossi L., et al. “The extracellular nucleotide UTP is a potent inducer of hematopoietic stem cell migration”. Blood 109.2 (2007): 533-542.
- Tashiro K., et al. “Signal sequence trap: a cloning strategy for secreted proteins and type I membrane proteins”. Science 261.5121 (1993): 600-603.
- Tokoyoda, K., et al. “Cellular niches controlling B lymphocyte behavior within bone marrow during development”. Immunity 20.6 (2004): 707-718.
- Vanhee S and Vandekerckhove B. “Pluripotent stem cell based gene therapy for hematological diseases”. Critical Reviews in Oncology/Hematology 97 (2016): 238-246.
- Voermans C., et al. “Adhesion molecules involved in trans-endothelial migration of human hematopoietic progenitor cells”. Stem Cells 18.6 (2000): 435-443.
- Wright DE., et al. “Hematopoietic stem cells are uniquely selective in their migratory response to chemokines”. Journal of Experimental Medicine 195.9 (2002): 145-154.
- Wu FY., et al. “Reduction of cytosolic p27 (Kip1) inhibits cancer cell motility, survival, and tumorigenicity”. Cancer Research 66.4 (2006): 2162-2172.
- Xia L., et al. “Surface fucosylation of human cord blood cells augments binding to P-selectin and E-selectin and enhances engraftment in bone marrow”. Blood 104.10 (2004): 3091-3096.
- Yin Tand Li L. “The stem cell niches in bone”. Journal of Clinical Investigation 116.5 (2006): 1195-1201.
- Zanjani ED., et al. “Homing of human cells in the fetal sheep model: modulation by antibodies activating or inhibiting very late activation antigen-4-dependent function”. Blood94.7(1999): 2515-2522.
- Zhang J., et al. “PTEN maintains haematopoietic stem cells and acts in lineage choice and leukaemia prevention”. Nature 441.7092 (2006): 518-522.
Citation:
Alemu Aylate. “A Review: Bone Marrow Homing Molecular Mechanisms of Stem Cells”. Clinical Biotechnology and
Microbiology 2.1 (2018): 289-297.
Copyright: © 2018 Alemu Aylate. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.






























 Scientia Ricerca is licensed and content of this site is available under a Creative Commons Attribution 4.0 International License.
Scientia Ricerca is licensed and content of this site is available under a Creative Commons Attribution 4.0 International License.