Case Report
Volume 4 Issue 1 - 2020
Role of Low Level LASER Therapy (LLLT) in Lymphoedema- Our Experience
1Senior Resident, Department of Plastic Surgery, Jawaharlal Institute of Postgraduate Medical Education and Research (JIPMER), Pondicherry, India
2Professor, Department of Plastic Surgery, Jawaharlal Institute of Postgraduate Medical Education and Research (JIPMER), Pondicherry, India
*Corresponding Author: Ravi Kumar Chittoria, Professor, Department of Plastic Surgery, Jawaharlal Institute of Postgraduate Medical Education and Research (JIPMER), Pondicherry, India.
Received: October 14, 2019; Published: January 28, 2020
Abstract
Lymphoedema is a chronic problem with various skin changes that lead to impaired care for the affected limb. These skin changes also lead to recurrent infections. The difficulty in care and the subsequent neglect leads to further spread of the infection and increased risk of future infections. Prevention of infections and prevention of progress of the skin changes is one of the main components of the treatment of the lymphoedema. There are various modalities available to enhance the healing of the knobs and fissures secondary to lymphoedema. We would like to present our case report on the usage of Low level laser therapy (LLLT) in a patient with stage 7 skin changes of lymphedema.
Key Words: Lymphoedema; Low Level LASER therapy; Chronic wounds
Introduction
Lymphedema is a devastating problem both for the patient and society[1]. India has the highest number of patients with lymphedema of infective etiology. The majority of these patients are from low socioeconomic status and usually present in advanced stages of the disease stage 6-7 according to WHO[2] or stage 3 according to the International Society of lymphology [ISL]. These stages have significant skin changes with a higher risk of infection.
According to the Fifth WHO Expert Committee on Filariasis, lymphoedema can be classified as follows:
- Grade I lymphoedema: mostly pitting edema; spontaneously reversible on elevation.
- Grade II lymphoedema: mostly non-pitting edema; not spontaneously reversible on elevation.
- Grade III lymphoedema (elephantiasis): a gross increase in volume in a grade II lymphoedema, with dermatosclerosis and papillomatous lesions.
The 7 stages of classification as given below are clinically based [2]
Stage 1
The feature of stage 1 lymphoedema is:
- Swelling is reversible overnight.
Stage 2 Swelling is not reversible overnight.
The main difference between stage 2 lymphoedema and stage 1 is that the swelling does not disappear without lymphoedema management.
Stage 3 Swelling is not reversible overnight. The principal feature of stage 3 lymphoedema is the presence of one or more shallow skin folds
Stage 4 Swelling is not reversible overnight.
The main feature of stage 4 lymphoedema is the presence of knobs lumps, lumps, or protrusions on the skin.
Stage 5 Swelling is not reversible overnight.
The presence of one or more deep skin folds is the main feature of stage 5 lymphoedema
Stage 6
Swelling is not reversible overnight. On the surface of the foot (especially the toes), very small elongated or rounded small knobs can be clustered together, giving rise to the peculiar appearance of “mossy foot”.
Patients with stage 6 lymphoedema) have acute attacks. Almost all these patients
have entry lesions between the toes and bad odour. Wounds in the skin are frequently present.
Stage 7
The features of stage 7 lymphoedema are:
Swelling is not reversible overnight. The patient is unable to adequately or
independently perform routine daily activities such as walking, bathing, cooking, etc.
Lymphoedema treatment requires a multimodal approach including non-operative management and surgical management.
Non-operative management includes maintenance of local hygiene, prevention and cure of entry lesions, elevation, exercise, compression bandaging, complex decongestive therapy, low-level laser therapy etc.
Surgical management includes reconstructive procedures like nodo-venous shunts, vascularised nodal transfer and debulking procedures like liposuction, Thompson procedure, Charles procedure.
However, prior to any definitive intervention, the infection and possible sites of entry of the secondary infections have to be controlled. One such attempt is reported in this article as the use of Low level laser therapy (LLLT) in an advanced case of lymphedema.
Materials and Methods
This is a case report of a 29yr female, from Calicut, Kerala with h/o swelling of the left lower limb since 16 years was admitted in our centre in the month of August 2019.
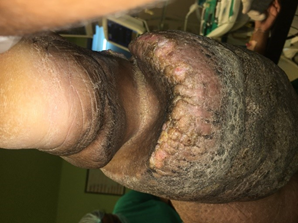
On assessment and through evaluation,the patient was diagnosed with chronic primary lymphedema of left lower limb with secondary grade 7 skin changes [WHO grading] [figure 1] with multiple fissures over the affected limb.
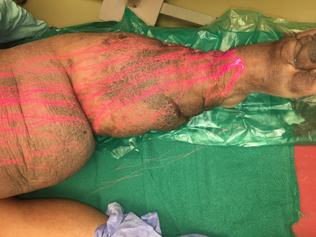
She also had foul smelling serous discharge from the limb. Patient underwent five applications of Low level LASER therapy (LLLT) once every three days [figure 2,3] along with a multimodal treatment of the affected limb including regular limb washes, limb elevation, compression dressings, over a period of 15 days. We used Gallium Arsenide (GaAs) diode red laser of wavelength 650 nm, frequency 10 kHz and output power 100 mW. It was a continuous beam laser with an energy density of 4 J/cm2. Machine delivers laser in scanning mode (non contact delivery) with 60 cm distance between laser source and wound. Each wound was given laser therapy for duration of 125 second every time[3]. Therapy was repeated until the wound epithelialized completely.
Results
At the end of the 5 sittings of LLLT the inspection of the limb revealed complete healing of the superficial ulcerations with no further discharge from the wounds [figure 4].
Discussion
LOW-LEVEL laser therapy (LLLT) is introduced by the work of Mester and colleagues as a therapeutic modality, who noted that with application of a low-energy (1 J/cm2 ) ruby laser there was improvement in wound healing.[4-6]
LLLT is defined by various parameters.
- The primary defining factor is power with a range of 10-3 to 10-1 W.
- Other parameters include
- A wavelength between 300 and 10,600 nm,
- A pulse rate of 0 (continuous) to 5,000 Hz,
- pulse duration of 1 to 500 milliseconds,
- An interpulse interval of 1 to 500 milliseconds,
- A total irradiation time of 10 to 3,000 seconds, an intensity (power/area) of 10-2 to 100 W/cm2,
- A dose (power irradiation time/area irradiated) of 10-2 to 102 J/cm2. [7]
Various substrates have been used to create the lasers used for LLLT. Substrates used in LLLT include inert gases, including helium neon (HeNe; 632.8 nm), ruby (694 nm), argon (488 and 514 nm), and krypton (521, 530, 568, and 647 nm), semiconductor laser diodes, including gallium arsenide (GaAs; 904 nm) and gallium aluminum arsenide (GaAlAs; 820 and 830 nm) devices. Recently GaAs[904nm] LASERs are the most commonly used[8].
The various effects are researched and given by Medrado et al who described that LLLT acts by diminishing exudation of the early phase of wound healing, the general effects due to cytokine release, local pain, and tumefaction are probably ameliorated.[9]
Our patient had the skin changes for the past 10 years which has been troublesome. The treatment with LLLT has helped in alleviating the pain, and healing of the fissures. International society of lymphology[ISL] also recommends the use of LLLT as one of the non-operative treatment modalities of lymphoedema. [10] The mechanism of action is not well defined, though it may be considered to cause reduction of pain and mobility of tissue than just pure lymphedema volume reduction.
Our use of LLLT has shown good improvement in the amount of discharge from the lesions and the healing of the fissures. This has further reduced the risk of secondary infection by helping in the treatment of the raw area and also its effect on micro-organisms which possibly prevented further infection.
Conclusion
Ours is a single case study which has shown favorable results with the use of LLLT.However, more studies with larger numbers of patients as randomized controlled trials are needed to confirm these findings. Further research is also required to definitively give the mechanism of action of Low level LASER therapy in lymphoedema.
References
- Avraham T., et al. “Cellular and Molecular Mechanisms of Lymphangiogenesis and Lymphedema”. Current Cancer Therapy Reviews 5.1 (2009): 28-36.
- Dreyer G., et al. “Lymphoedema staff manual: treatment and prevention of problems associated with lymphatic filariasis”. WHO/CDS/CPE/CEE/2001.26a.
- Gaida K., et al. “Low Level Laser Therapy--a conservative approach to the burn scar?”. Burns 30.4 (2004): 362-367.
- Mester E., et al. “The effect of laser irradiation on the regeneration of muscle fibers (preliminary report)”. Zeitschrift für experimentelle Chirurgie 8.4 (1975): 258-262.
- Mester E., et al. “The biomedical effects of laser application”. Lasers in Surgery and Medicine 5.1 (1985): 31-39.
- Mester E., et al. “Effect of laser rays on wound healing”. The American Journal of Surgery 122.4 (1971): 532-535.
- Schindl A., et al. “Low-intensity laser therapy: a review”. Journal of Investigative Medicine 48.5 (2000): 312-326.
- Basford JR. “Low intensity laser therapy: still not an established clinical tool”. Lasers in Surgery and Medicine 16.4 (1995): 331-342.
- Medrado AR., et al. “Influence of low level laser therapy on wound healing and its biological action upon myofibroblasts”. Lasers in Surgery and Medicine 32.3 (2003): 239-244.
- Executive Committee. “The Diagnosis and Treatment of Peripheral Lymphedema: 2016 Consensus Document of the International Society of Lymphology”. Lymphology 49.4 (2016): 170-84.
Citation: Ravi Kumar Chittoria., et al. “Role of Low Level LASER Therapy (LLLT) in Lymphoedema- Our Experience”. Medical Research and Clinical Case Reports 4.1 (2020): 01-06.
Copyright: © 2020 Ravi Kumar Chittoria., et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.





































 Scientia Ricerca is licensed and content of this site is available under a Creative Commons Attribution 4.0 International License.
Scientia Ricerca is licensed and content of this site is available under a Creative Commons Attribution 4.0 International License.