Case Report
Volume 1 Issue 3 - 2018
Nipple Adenoma: Report of two Cases and Review of the Literature
Breast Surgery Division, King Fahd Hospital of the University, Al khobar Imam Abdulrahman Bin Faisal University, Dammam, Kingdom of Saudi Arabia
*Corresponding Author: Maha Abdel Hadi, Professor/Consultant General & Breast surgeon, King Fahd hospital of the University, P.O.Box 40293 Al-Khobar 31952 Kingdom of Saudi Arabia.
Received: March 26, 2018; Published: April 10, 2018
Case 1
A 34 years old Saudi single female presented with an ulcerated left nipple of two years duration. Patient gave no history of associated co-morbidities. It was sudden in onset with no predisposing factors. She was a regular visitor to many dermatology clinics and history of chronic use of topical creams and ointments with brief relieve and recurrence once the treatment was discontinued. On clinical examination general examination revealed an anxious young female otherwise unremarkable. Local examination revealed an ulcerated bleeding nipple with obvious fissures. The remaining examination of both breast was within normal limits. Ultrasound was reported as normal. Wedge excision of the medial aspect of the nipple and areola was performed and was reported as Nipple Adenoma with no evidence of malignancy. Local treatments were not effective, patient refused the suggested nipple excision. Patient was followed up for three months and then lost follow up.
Case 2
A 43-year-old Saudi female with no reported comorbid conditions presented with thickened, cracked right nipple and bloody discharge of 4 years duration. It was sudden in onset associated with discomfort but no pain. She gave no history of palpable breast masses or other local or systemic symptoms. The patient noticed progressive thickening of the nipple associated with persistent ulceration not responding to local or systemic antibiotics and anti-inflammatory treatments. Family history for similar lesion or breast cancer is negative.
On examination: general examination was unremarkable. Local examination revealed an ulcerated flattened right nipple with bloody discharge from its surface. (Figure I) the surrounding was indurated with a small palpable retro areolar nodule measuring about 1x1 centimeter in diameter. There were palpable axillary lymph nodes could. Left breast was unremarkable. Paget’s disease was the clinical diagnosis at presentation.
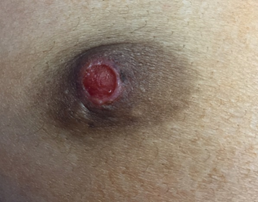
Figure I: demonstrates the replacement of the
nipple with a sharp margin ulcer with deformity of
the nipple areolar complex denoting chronicity.
Mammography and Ultrasound revealed elements of duct ectasia bilaterally with no suspicious masses. Consistent with BI-RADS II findings. (Figure II)
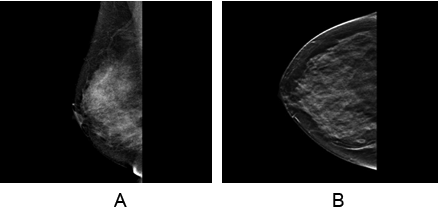
Figure II (a & b): The mediolateral and craniocaudal views demonstrate
the normal glandular breast tissue with no evidence of suspicious lesions
or retro-areolar architectural distortion.
In view of the chronic and persistent lesion and the suspicious of Paget’s disease a wedge biopsy was performed under local anesthesia and was reported as proliferative epithelial lesion with features suggestive of nipple adenoma with no malignancy. The discrepancy between the clinical manifestation and the and histopathology report mandated another biopsy under general anesthesia and was reported as the same histopathological findings. Dermatology consultation and local treatment was again initiated with mild improvement of the symptoms. Patient underwent total nipple excision and pathology report revealed microscopic examination of the excised nipple shows a relatively well circumscribed lesion composed of compacted proliferative ducts and tubules in the dermis and nipple stroma. The overlaying epidermis showed ulceration and granulation tissue formation. On higher magnification, the ducts showed a spectrum of hyperplastic changes ranging from mild papillary hyperplasia to florid ductal hyperplasia. The lining ductal cells lack cytological atypia. Calponin and p63 highlight the myoepithelial layer surrounding each duct. These features were diagnostic of nipple adenoma\ florid papillomatosis of the nipple. (Figure III) At three months follow up the patient was satisfied with complete healing of postoperative site.
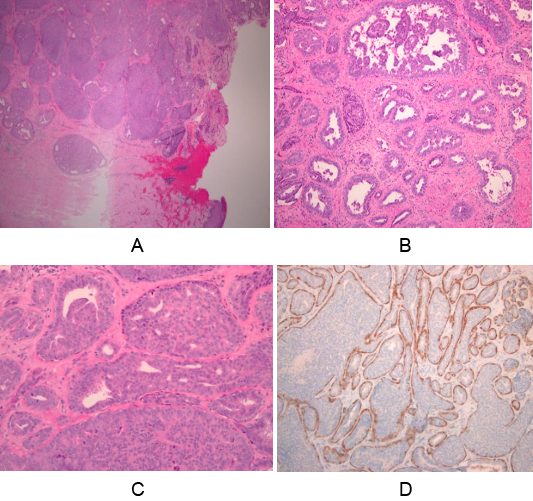
Figure III (a-d): The mediolateral and craniocaudal views demonstrate
the normal glandular breast tissue with no evidence of suspicious lesions
or retro-areolar architectural distortion.
Discussion
Breast Cancer is commonest malignancy affecting women worldwide and is the second most common female in Saudi Arabia [1]. The concerns of breast cancer in any breast complaint dictate the thorough clinical evaluation and focused investigations of all symptomatic breast patients. Nipple adenoma is a rare condition which is usually missed and unrecognized by many breast care specialties. [2]
It is proven histologically that it is a benign ductal proliferative disease of middle aged women. Patients may present with a palpable nodule, or commonly presents as nonhealing ulcer characterized by erosion and crusting. [3] The age, chronicity, the presence of ulceration and nipple destruction mimic the clinical manifestations of paget’s disease [4,5].
The standard imaging dependent on age groups, ultrasonography or mammography are the initial steps in diagnosis. The limitations of both modalities are noted due to the fact that nipple adenomas have the same density as the surrounding breast tissue with minimal architectural distortion. Few reports favored ultrasound despite its limited yield in detecting the echogenicity and hypervascularity which aid the diagnosis of adenoma [4,7,8].
Nipple adenomas are categorized under the benign ductal proliferative disease. Occurrence is in the middle age group with prolonged symptoms. [3]
The common presentation is non-healing ulcers, however a less commonly patients my breast with breast masses. [9] Pathology may show inflammatory reaction and benign ductal epithelial cells on the excised wedge with repeated negative cytology. [10]
The benign pattern of nipple adenoma should not be taken for granted is not always the case. Reports had shown the close association of nipple adenoma with malignant breast conditions [11,12]. It has also been reported at rare sites such as in an accessory breast [6]. Nipple adenoma is not an exclusive female disease as it had been seldom reported in males. [10,13].
Unilaterality is the usual presentation of this entity however it may occur as bilateral disease. [11]. Nipple adenoma might mimic wide range of benign and potentially malignant conditions. Thus, Biopsy of the nipple lesion is an essential tool for primary diagnosis [6,13].
Histologic appearance of benign adenoma shows 2 layers of epithelial cells and mypoepithelial cells which is the main component to differentiate it from malignancy [14].
Complete surgical excision of the nipple skin, underlying subcutaneous tissues and surrounding skin with histologic examination remains the gold standard for diagnosis and treatment [7,13,14].
However, others reported successful complete excision of the adenoma with preservation of the nipple [8,14]. The literature supported the good prognosis of this benign condition. However, the risk and relation to malignancy is still unknown and thus regular follow up is warranted [5,11,13].
These two rare presentations had posed challenges on both diagnosis and management. Biopsy followed by complete surgical excision of the nipple skin, underlying subcutaneous tissues and surrounding skin with histologic examination remains the gold standard for the management of nipple adenoma.
References
- Bazarbashi S., et al. “Cancer Incidence in Saudi Arabia: 2012 Data from the Saudi Cancer Registry.” Asian Pacific Journal of Cancer Prevention 18.9 (2017): 2437-2444.
- Wang C., et al. “Diagnosis and surgical treatment of nipple adenoma”. ANZ Journal of Surgery 85.6 (2015): 444-447.
- Eusebi V and Lester S. Tumours of the nipple (chapter 12) In: Lakhani SR, Ellis IO, Schnitt SJ, Tan PH, van de Vijver MJ, editors. WHO classification of tumours of the breast. 4. Lyon, France: IARC; (2012).
- Tsushimi T., et al. “Adenoma of the nipple, focusing on the contrast-enhanced magnetic resonance imaging findings: report of a case”. Surgery Today 41.8 (2011): 1138-1141.
- Ozaki S., et al. “Cytologic features of nipple adenoma: a report of four cases of adenoma of the nipple”. Diagnostic Cytopathology 43.8 (2015): 664–668.
- Fujii T., et al. “Adenoma of the nipple projecting out of the nipple: curative resection without excision of the nipple”. World Journal of Surgical Oncology 12 (2014).
- Shioi Y., et al. “Nipple adenoma arising from axillary accessory breast: a case report”. Diagnostic Pathology (2012).
- Wagner N., et al. “Superficial papillary adenomatosis of the nipple: a rare disease diagnosed by sonography and histopathologically confirmed by nipple-preserving total excision”. Journal of Ultrasound in Medicine 32.2 (2013): 373–374.
- Fujii T., et al. “Adenoma of the nipple projecting out of the nipple: curative resection without excision of the nipple”. World Journal of Surgical Oncology (2014).
- Salemis NS. “Florid papillomatosis of the nipple: a rare presentation and review of the literature”. Breast Disease 35.2 (2015): 153-156.
- Sasi W., et al. “Bilateral florid papillomatosis of the nipple: an unusual indicator for metachronous breast cancer development-a case report”. Case Reports in Oncological Medicine (2014).
- Lee C and Boughey J. “Case report of a synchronous nipple adenoma and breast carcinoma with current multi-modality radiologic imaging”. The Breast Journal 22.1 (2016): 105-110.
- Gina P Spohn., et al. “Nipple adenoma in a female patient presenting with persistent erythema of the right nipple skin: case report, review of the literature, clinical implications, and relevancy to health care providers who evaluate and treat patients with dermatologic conditions of the breast skin”. BMC Dermatology (2016).
Citation:
Maha Abdel Hadi., et al. “Nipple Adenoma: Report of two Cases and Review of the Literature”. Medical Research and Clinical
Case Reports 1.3 (2018): 76-80.
Copyright: © 2018 Maha Abdel Hadi., et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.



































 Scientia Ricerca is licensed and content of this site is available under a Creative Commons Attribution 4.0 International License.
Scientia Ricerca is licensed and content of this site is available under a Creative Commons Attribution 4.0 International License.