Research Article
Volume 1 Issue 1 - 2017
Intracoronary Infusion of Nicorandil Mixed with Contrast Through a Thrombus Aspiration Catheter Placed Distally in the Culprit Vessel Reduces Incidence of No-Reflow and Slow-Flow in Acute Myocardial Infarction Patients with a High Thrombus Burden.
CARE Banjara, Hyderabad, India
*Corresponding Author: Udaya Prashant Ponangi, CARE Banjara, Hyderabad, India.
Received: October 01, 2016; Published: June 27, 2017
Abstract
Aims: During primary angioplasty, infusing 2 mg of intravenous nicorandil mixed with radio-opaque contrast through a thrombus aspiration catheter placed distally in the culprit vessel, improves myocardial flow and reduces no-reflow in patients with a high thrombus burden.
Methods and Results: Between March 2013 and March 2015, 30 acute myocardial infarction (MI) patients with late presentation and having a large thrombus burden total occlusion in their culprit coronary arteries were included in the study. The angiographic and clinical outcomes of the novel group, where the intracoronary nicorandil mixed with contrast was infused into their distal arteries (number of patients 16), were compared to those patients who underwent primary angioplasty by the conventional methods which included multiple attempts of thrombus aspiration, pre dilatations and infusing vasodilators proximal to culprit lesion (number of patients 14). In the nicorandil group, Thrombolysis in Myocardial Infarction (TIMI) III flow was achieved in 12 patients when compared to 5 patients in the conventional group. (p = 0.03). The novel group also had better Thrombolysis in Myocardial Perfusion (TMP) scores (11 vs 3; p = 0.009) and ST-segment resolution (8 vs 3; p = 0.029) after intervention when compared to the standard approach group. Mortality at the end of 30 days was lesser in the novel method group but was not statistically significant (2 vs 4; p = 0.26). These benefits were attributed to correct size stent selection with limited intracoronary manipulations of the clot due to better delineation of the entire length of total thrombotic occlusion and also the distal microvascular bed protection offered by nicorandil.
Conclusions: Our initial analysis favours the novel concept of infusing intracoronary nicorandil mixed with contrast solution beyond a totally occluded culprit vessel with a large thrombus burden in selective acute MI patients, helps to achieve improved myocardial flow and perfusion along with reduction in mortality
Keywords: Aspiration Catheter; Primary Angioplasty; No-reflow
Introduction
The phenomenon of no-reflow was first defined by Kloner as inadequate myocardial perfusion through a given segment of the coronary circulation without angiographic evidence of mechanical vessel obstruction [1]. Defined angiographically, no-reflow manifests as an acute reduction in thrombolysis in myocardial infarction (TIMI) coronary flow of grade 0-1, in the absence of dissection, thrombus, spasm, or high-grade residual stenosis at the original target lesion. Lesser degrees of TIMI flow impairment of grade 2 are generally referred to as “slow-flow and all are mainly due to intense microvascular obstruction [2]. The incidence of no-reflow during percutaneous interventions (PCI) is found to be 0.6 to 2% and more common during rotational atherectomy, interventions of thrombus containing lesions and is an independent predictor of mortality after percutaneous interventions [3]
During primary angioplasty in myocardial infarction (PAMI), occasionally good flows are not established in spite of repeated aspirations or infusion of glycoprotein 2b 3a inhibitors, or other pharmacological agents like nitroprusside, verapamil or adenosine (either through the guide or an intracoronary micro catheter) [4]. Sometimes tight mechanical obstruction within the lesion prevents the advancement of suction catheters and hence requires predilatation [5]. The concept of prevention of slow flow in acute MI by direct stenting was not new [6,7], and has been recognized since the time when primary angioplasty started becoming the established mode of treatment for MI [8]. Piscone et al found that in selected coronary lesions, direct stenting improves outcome in patients undergoing percutaneous coronary intervention, primarily reducing myocardial infarction incidence rather than conventional predilatation followed by stenting [9]. Also, the use of thrombus aspiration catheter after initial studies like TAPAS [10] and EXPIRA [11] became a standard method in the treatment of MI but larger studies, like TASTE [12], TOTAL [13] did not show similar benefit and thrombosuction lost its popularity.
In our study, we aimed to define the best clinical settings and adopt innovative methods of thrombosuction catheters for achieving better outcomes in the selected group of patients presenting with acute MI.
Methods
It is a case controlled study of selected primary angioplasty cases between March 2013 and March 2015. An institutional review committee approved the retrospective study and the subjects gave informed consent for primary PCI and subsequent data analysis. 30 ST-elevation myocardial infarction (STEMI) patients above 18 years of age presenting to CARE Hospitals Banjara Hills, satisfying the criteria for primary angioplasty and who had no flow or TIMI I flow after an attempt of thrombus aspiration by Export (Medtronic, USA) thrombosuction catheter were included. The patients had chest pain for at least 12 hours duration or between 12 hours to 24 hours and had persistent symptoms with evidence of ongoing ischemia. Diagnosis of MI was made with ECG criteria of ST elevation of 1 mm in two contiguous electrocardiography leads or a new onset of left bundle branch block with history of prolonged chest pain (> 30 min) and documentation of MI in the catheterization laboratory (with evidence of high-grade coronary stenosis and associated LV wall-motion abnormalities).
They were divided into 2 Groups
- In the first group, the thrombus aspiration catheter is placed distal to culprit lesion and intracoronary nicorandil mixed with contrast is infused slowly. (N = 16)
- In the second group, the thrombus aspiration catheter was used in a conventional way along with other drugs and stents (N = 14)
Exclusion Criteria
Patients with a significant left main disease, bifurcation lesions, highly calcific and tortuous arteries, thrombosis or SVG thrombosis, pre-existing renal failure or bleeding/coagulation disorders were all excluded from the study.
Patients with a significant left main disease, bifurcation lesions, highly calcific and tortuous arteries, thrombosis or SVG thrombosis, pre-existing renal failure or bleeding/coagulation disorders were all excluded from the study.
The primary end point was achieving TIMI III flow and ≥ 2 TMP score at the end of the procedure. The secondary endpoint was all-cause mortality at the end of 30 days.
Standard semi-quantitative TIMI flow definitions were used to assess the angiographic results based on the Thrombolysis in Myocardial Infarction (TIMI) trial [14]. TIMI 0 is no antegrade flow beyond the occlusion, TIMI I is faint antegrade flow with an incomplete filling of the distal bed, TIMI II is delayed or sluggish flow with complete filling of distal bed and TIMI III is normal flow or filling of a vessel in 3 cardiac cycles with complete filling of distal territory.
Standard TMP scoring system was used to assess distal perfusion after angioplasty, TMP Grade 0 is defined when there is either minimal or no ground-glass appearance or blush of the myocardium. TMP Grade 1 when the myocardial blush fails to clear in next infection (~30 seconds) injection TMP Grade 2 when the myocardial blush persists strongly even after 3 cardiac cycles. TMP Grade 3 When the dye appears and clears normally in the myocardium within 3 cardiac cycles [15]
Two independent and blinded interventional cardiologists viewed the stored angiogram cines and gave their opinion on final TIMI flows and TMP grades. Complete ST segment resolution after the procedure was defined as > 70% reduction in the ST-segment elevation of the lead with the highest elevation on admission
In the first group, we crossed the thrombus containing lesion and placed the aspiration catheter in the distal vessel and infused slowly 2 mg of intravenous nicorandil solution diluted in 5 ml of 0.9% normal saline mixed with 5 ml of iodine contrast in a 10 ml syringe over 1–2 minutes. The second group had conventional angioplasty done after predilatation and stenting of coronary arteries that were totally occluded at the time of PAMI.
The proportions were compared using a Pearson Chi-square test and if any cell value was less than 5 Yates correction was performed. For non-significant ratios, p values were calculated by one-tailed Fisher Exact probability test. Continuous variables were compared using an unpaired t-test. All statistical analysis was done using SPSS software.
Results
The baseline characteristics between two groups (Table 1) are matched. The mean age of presentation was 56 years and males compromised of 53% of cases. The most common initial ECG diagnosis was anterior wall MI (57%) followed by inferior, posterior and right ventricular MI (26%) and least common was inferior with lateral wall MI cases (17%). The average window period of the presentation was 10 ± 2 hours. Only 2 cases were failed thrombolysis, one received Tenecteplase and the other Streptokinase in outside centers before referring to our hospital. 10 cases (33%) had multivessel involvement and others were single vessel disease. The average ejection fraction (EF) before the intervention was 39 ± 8%. 26% of cases had a cardiogenic shock at presentation and all of them had inotropes started and Intra-aortic balloon pump (IABP) inserted at the time of the procedure.
| Patient Characteristics | Number | Group I (16) | Group II (14) | P value. |
| Males | 16 (53%) | 10 | 6 | 0.282 |
| Females | 14 (47%) | 6 | 8 | 0.281 |
| Hypertension | 16 (53%) | 10 | 6 | 0.28 |
| Diabetics patients | 14 (47%) | 9 | 6 | 0.464 |
| Smokers | 8 (20%) | 5 | 3 | 0.544 |
| Dyslipedemia | 13 (43%) | 8 | 5 | 0.88 |
| History of previous infarction | 4 (13%) | 2 | 2 | 0.495 |
| Anterior wall MI | 17 (56%) | 9 | 8 | 0.37 |
| Inferior and lateral wall MI | 5 (17%) | 3 | 2 | 0.86 |
| Inferior posterior and right ventricular MI | 8 (26%) | 2 | 6 | 0.06 |
| Average Door to Balloon time | 10 ± 2 hrs | 11+/-2 | 10+/-2 | 0.37 |
| Rescue angioplasty no of cases. | 2 (7%) | 1 | 1 | 0.4 |
| Average EF of patients | 39 ± 8% | 38 ± 8% | 39 ± 6% | 0.78 |
| Initial Cardiogenic shock | 8 (26%) | 5 | 3 | 0.86 |
Table 1: Patient characteristics.
The procedural outcomes are summarized in Table 2. The patients in both groups with multivessel involvement, LAD, RCA as culprit artery were similar except left circumflex vessel where the novel method could not be used and conventional method was adopted, 2 patients. 6 patients (20%) had significant conduction abnormalities and required a temporary pacemaker (TPI) insertion, but none of them required long-term pacemaker support. Nearly 80% patients were administered with glycoprotein-2b3a inhibitors as all of them had high thrombus burden. Following the use of thombosuction catheter, interventionist proceeded with angioplasty in the usual manner. DES and BMS stents were used in both the groups and there were no significant differences in either of the groups with regards to the type of stents used.
| Primary PCI | Group I (16) | Group II (14) | P value. |
| Multi vessel involvement | 6 | 4 | 0.89 |
| Culprit artery LAD | 8 | 8 | 0.68 |
| LCx | 0 | 2 | 0.021 |
| RCA | 8 | 4 | 0.4 |
| IABP | 6 | 7 | 0.48 |
| TPI | 4 | 2 | 0.78 |
| Gp2b3a inhibitors used | 12 | 12 | 0.231 |
| DES | 12 | 11 | 0.307 |
| BMS | 5 | 3 | 0.85 |
| Immediate TIMI III flow | 12 | 5 | 0.03 |
| TMP ≥ 2 | 11 | 3 | 0.009 |
| Persistent ST elevation | 3 | 8 | 0.029 |
| Reinfarction and target vessel revascularization | 3 | 2 | 0.56 |
| Major Bleeding | 2 | 3 | 0.43 |
| All cause mortality at the end of 30 days | 2 | 4 | 0.26 |
Table 2: Comparison of results between the intracoronary Nicorandil group and control group where routine primary angioplasty was performed.
When the novel method was used 12 out of 16 achieved good angiographic results as opposed to 5 out of 14 cases where the standard technique was used (p = 0.03; Odds Ratio (OR) 5.4; 95% Confidence Intervals (CI) 1.1-26). The number of patients of who achieved ≥ 2 TMP scores were 11 in the first group and 3 in the second group (p = 0.009; OR 8.06; 95% CI 9.2-42.3). Persistent ST elevation was seen in 8 patients with conventional method whereas it was observed only in 3 patients with novel method and it is statistically significant (p = 0.029; OR 0.17; 95% CI 0.03-0.89) The overall 30 day mortality was also lower in the nicorandil group, though it did not achieve statistical significance (p = 0.26; OR 0.3; CI 0.05–2.3). In the first group given 2 out of 14 patients succumbed, while in the second group 4 out of 14 patients died at the end of 30 days.
Figure 1 is an example of a typical case where this method was used successfully. She was a 42-year-old lady, recently diagnosed to be diabetic and presented to us with AWMI of 10 hours duration. Figure 2 shows PAMI cine sequences of a 32-year-old gentleman with acute inferior, posterior and right ventricular MI of 18 hours in cardiogenic shock and complete heart block (CHB). Figure 3 depicts angiography sequences of a 62-year-old male patient who had AWMI and presented to us in cardiogenic shock with a window period of 8 hours. The lesion was predilated multiple times before the stent deployment and even though TIMI III flow was achieved, there was no distal perfusion and the patient died after 36 hours due to refractory cardiogenic shock and multiorgan failure.
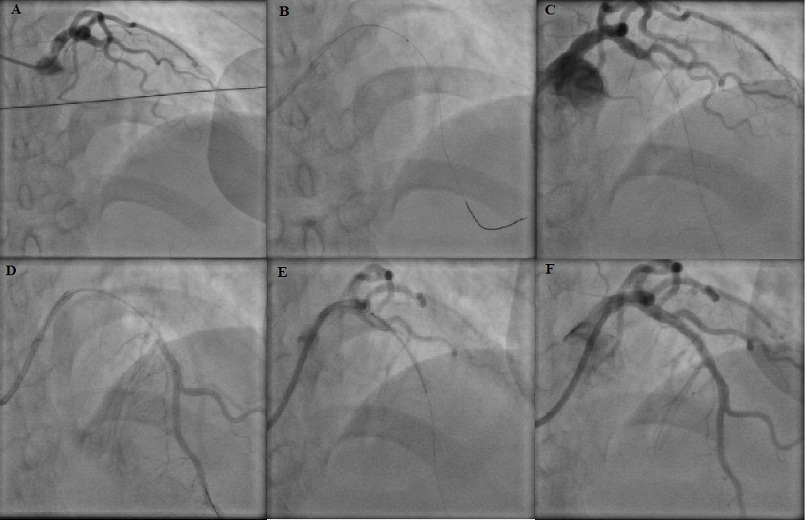
Figure 1: A) LAD proximal total occlusion. B) Thrombosuction of totally occluded thrombotic lesion. C) Result after thrombosuction. D) Distal vessel visualized by our novel technique. E) Stent across the culprit lesion. F) Final TIMI III flow with good perfusion result.
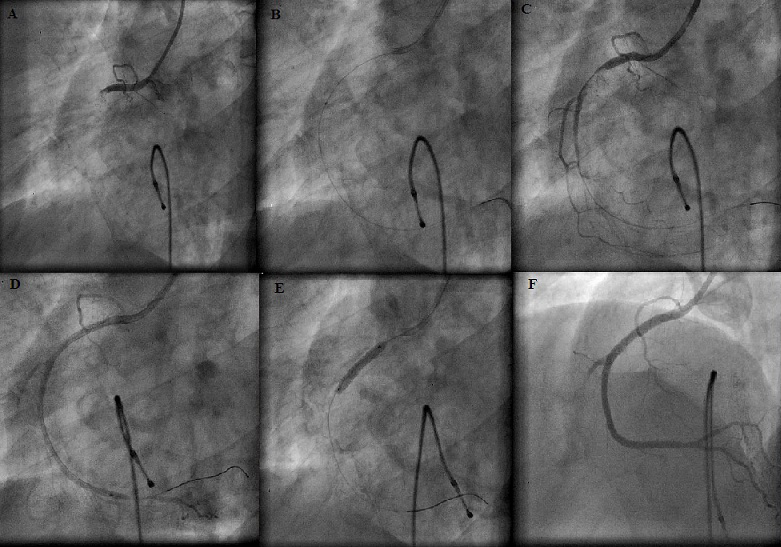
Figure 2: A) RCA proximal total occlusion. B) EXPORT catheter across the culprit lesion C) Result after thrombosuction D) Distal vessel visualized using our novel techniques and crux of RCA had significant spasm E) Stenting of culprit lesion F) Final TIMI III and TMP 3 result.
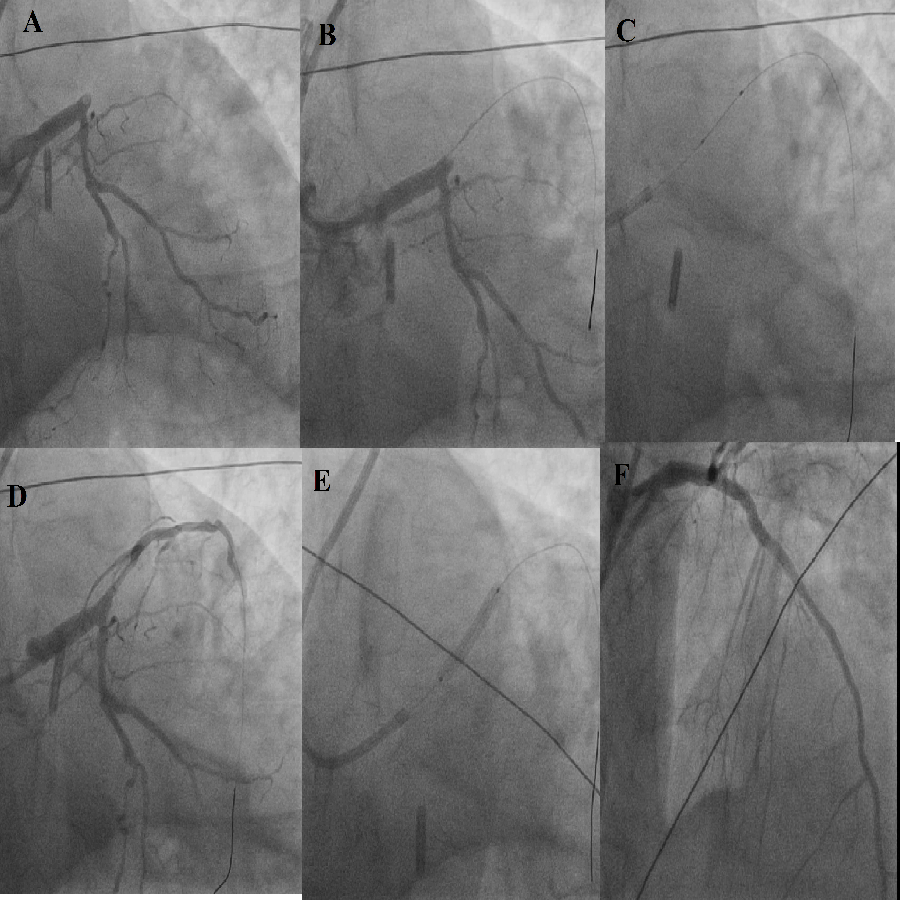
Figure 3: A) LAD proximal occlusion had tight stenosis B) Lesion crossed with PTCA wire C) Multiple predilatations of the culprit lesion D) After predilatations E) Stent deployment across the culprit lesion F) Final TIMI III result but no perfusion.
Discussion
No-reflow or slow-flow during percutaneous coronary interventions (PCI) is one of the dreaded complications associated with poor clinical outcomes and high mortality [3]. Some of the different predictors of slow flow or no reflow are elderly population, smoking, prolonged door to balloon/needle times, left ventricular ejection fraction, advanced Killip's class at presentation, diabetes mellitus, serum creatinine and others. Among these relevant to this study are interval to treatment times [16] and thrombotic loads.
No definitive recommendations can be made for treatment of no-reflow once it has occurred because the proposed interventions have not been studied in randomized trials and none of them are uniformly successful. The PCI guidelines give a class IIa recommendation for administration of intracoronary vasodilators like adenosine, nitroprusside, verapamil and diltiazem [17]. Nicorandil was also found to be helpful in the treatment of no reflow [18,19]. Apart from vasodilators the other agents, which were found to be helpful in these situations were glycoprotein-2b3a inhibitors [20]. We have used this novel method initially to treat no reflow situations, but I adopted it as a standard approach to tackling difficult cases. After an initial one or two attempts of clot extractions, if there was no TIMI > 1 flow then we proceed straight to this method instead of wasting time by repeated thrombosuction attempts.
Direct stent implantation during PAMI avoids balloon-induced thrombus fragmentation and reduces distal embolization Thrombosuction catheters, which are used to reduce thrombus burden and establish flow, have recently found to go into disrepute after the publication of TASTE [12], TOTAL [13] trials leading to change in the recommendation of guidelines for acute MI management. Only initial trials like TAPAS [10], EXPIRA [11] have shown a benefit of the routine use of thrombosuction catheters. On the basis of the results of these studies, the prior Class IIa recommendation for aspiration thrombectomy has been changed and now given the Class III status for routine use of aspiration catheters during primary PCI [21]. Some of the negative results can be explained after use in all cases instead of selected cases and excessive manipulation through repeated attempts of thrombosuction producing a dottering effect leading to distal clot embolization.
Yu Jun Zhao., et al. injected nitroprusside and tirofiban through thrombosuction catheter after crossing the infarct related artery and compared their results with standard approach [22]. Patients with delayed presentation and cardiogenic shock were excluded from the study, whereas these are the group of patients, who will have significant thrombus loads and are prone to develop no reflow during interventions and derive maximum benefit by this novel technique. Also, nicorandil along with iodine contrast was used though we did not mix Glycoprotein 2b3a inhibitor and the purpose of it was two-fold. Besides preventing no-reflow by reducing the intracoronary thrombus microembolization, it also helps in choosing an appropriately sized stent and defines accurately the distal landing zone for stent deployment. If the chosen stent falls short of the lesion and deployed in the middle of the culprit lesion then it causes slow flow due to thrombus embolization and increased chances of stent edge dissection. If it is undersized then it leads to stent thrombosis.
This paper describes late presentation MI cases in cardiogenic shock as a high-risk clinical setting for the occurrence of no-reflow and infusing intracoronary nicorandil diluted with iodine contrast solution distally in the culprit vessel through a thrombosuction catheter effectively prevents this complication. Nicorandil produced least hemodynamic compromise in a setting of cardiogenic shock with high thrombus loads, so we preferred it over to nitroprusside or other vasodilators. Many studies prove that achieving TIMI III flow and TMP ≥ 2 flow with ST-segment resolution after PCI is important for achieving good survival outcomes, less adverse cardiac events and preservation of EF later in acute MI patients [23,24]. The mortality benefit in our study was not statistically significant because of the small number of selected cases. In order to validate these conclusions, further large-scale, prospective, randomized and multicentric studies involving routine primary PCI patients who failed to develop adequate TIMI flow have to be included instead of a very sick subgroup of patients which were selected in the present study. An algorithmic approach that can be used in selecting the appropriate cases during primary angioplasty for this technique is illustrated in Figure 4
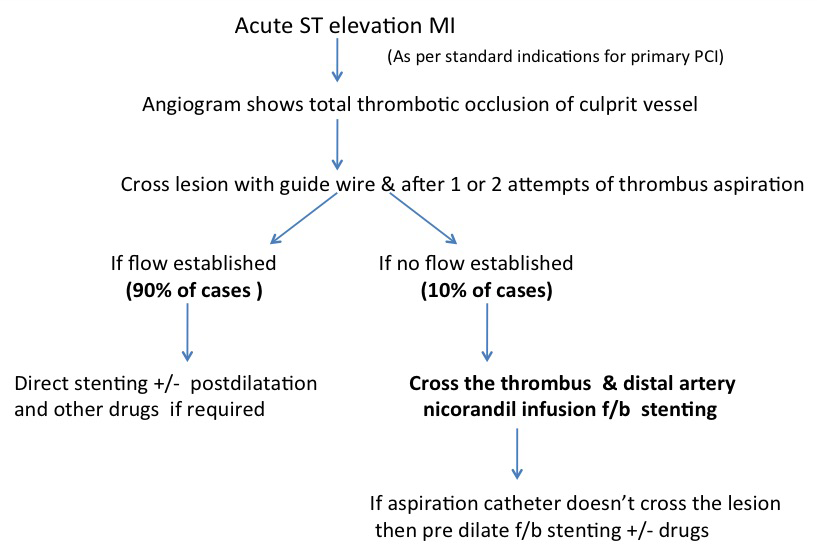
Figure 4: Algorithm approach outlining the case selection, best
suitable for this novel technique during primary angioplasty.
Conclusions
Our initial analysis favours the novel concept of infusing intracoronary nicorandil mixed with contrast solution beyond a totally occluded culprit vessel with a large thrombus burden in selective acute MI patients, helps to achieve improved myocardial flow and perfusion along with reduction in mortality
Acknowledgements
We would like to thank Dr Raghavaraju MD, DM; Dr Srinivas Raju MD, DNB and Mr. Ram Babu for their support and advice in conducting the study.
We would like to thank Dr Raghavaraju MD, DM; Dr Srinivas Raju MD, DNB and Mr. Ram Babu for their support and advice in conducting the study.
References
- Kloner RA., et al. “The ‘no-reflow’ phenomenon after temporary coronary occlusion in the dog”. The Journal of Clinical Investigation 54.6 (1974): 1496–1508
- Wilson RF., et al. “Intense microvascular constriction after angioplasty of acute thrombotic coronary arterial lesions”. Lancet 1(8642) (1989): 807–811.
- Resnic FS., et al. “No-reflow is an independent predictor of death and myocardial infarction after percutaneous coronary intervention”. American Heart Journal 145.1 (2003): 42-46.
- Ronen Jaffe., et al. “Prevention and treatment of microvascular obstruction-related myocardial injury and coronary no-reflow following percutaneous coronary intervention: a systematic approach”. JACC: Cardiovascular Interventions 3.7 (2010): 695–704.
- CL Grines., et al. “Stent Primary Angioplasty in Myocardial Infarction Study Group, Coronary angioplasty with or without stent implantation for acute myocardial infarction”. The New England Journal of Medicine 341.26 (1999): 1949–1956.
- Antoniucci D., et al. “Direct infarct artery stenting without predilation and no-reflow in patients with acute myocardial infarction”. American Heart Journal 142.4 (2001): 684-690.
- Chuang Li., et al. “Comparing Direct Stenting With Conventional Stenting in Patients With Acute Coronary Syndromes: A Meta-Analysis of 12 Clinical Trials”. ANGIOLOGY 67.4 (2016): 317-325.
- Grines CL., et al. “The Primary Angioplasty in Myocardial Infarction Study Group A comparison of primary angioplasty with thrombolytic therapy for acute myocardial infarction”. The New England Journal of Medicine 328.10 (1993): 673-679.
- Piscione F., et al. “Is direct stenting superior to stenting with predilation in patients treated with percutaneous coronary intervention? Results from a meta-analysis of 24 randomised controlled trials”. Heart 96.8 (2010): 588-594.
- Vlaar PJ., et al. Cardiac death and reinfarction at end of 1 year in the Thrombus Aspiration during Percutaneous coronary intervention in Acute myocardial infarction Study (TAPAS): a 1-year follow-up study”. Lancet 371.9628 (2008): 1915-1920.
- Sardella G., et al. “Thrombus aspiration during primary percutaneous coronary intervention improves myocardial reperfusion and reduces infarct size: the EXPIRA (thrombectomy with export catheter in infarct-related artery during primary percutaneous coronary intervention) prospective, randomized trial”. Journal of the American College of Cardiology 53.4 (2009): 309–315.
- Fröbert O., et al. “Thrombus aspiration during ST-segment elevation myocardial infarction”. The New England Journal of Medicine 369.17 (2013): 1587-1597.
- Jolly SS., et al. “Randomized trial of primary PCI with or without routine manual thrombectomy”. The New England Journal of Medicine 372.15 (2015): 1389-1398.
- TIMI Study Group. “The Thrombolysis in Myocardial Infarction (TIMI) trial. Phase I findings”. The New England Journal of Medicine 312.14 (1985):932–936.
- C Michael Gibson., et al. “Relationship of TIMI Myocardial Perfusion Grade to Mortality After Administration of Thrombolytic Drugs”. Circulation 101.2 (2000): 125-130.
- Kloner RA., et al. “Impact of time to therapy and reperfusion modality on the efficacy of adenosine in acute myocardial infarction: The AMISTAD-2 trial”. European Heart Journal 27.20 (2006): 2400-2405.
- Eeckhout E and Kern MJ. “The coronary no-reflow phenomenon: a review of mechanisms and therapies”.European Heart Journal 22.9 (2001): 729-739.
- Ito H., et al. “Intravenous nicorandil can preserve microvascular integrity and myocardial viability in patients with reperfused anterior wall myocardial infarction”. Journal of the American College of Cardiology 33.3 (1999): 654-660.
- Ishii H., et al. “Impact of a single intravenous administration of nicorandil before reperfusion in patients with ST- segment-elevation myocardial infarction”. Circulation 112.9 (2005): 1284-1288.
- Montalescot G., et al. “Platelet glycoprotein IIb/IIIa inhibition with coronary stenting for acute myocardial infarction”. The New England Journal of Medicine 344.25 (2001):1895-903.
- Levine GN., et al. “2015 ACC/AHA/SCAI Focused Update on Primary Percutaneous Coronary Intervention for Patients With ST-Elevation Myocardial Infarction: An Update of the 2011 ACCF/AHA/SCAI Guideline for Percutaneous Coronary Intervention and the 2013 ACCF/AHA Guideline for the Management of ST-Elevation Myocardial Infarction”. Journal of the American College of Cardiology 67.10 (2016):1235-50.
- Zhao YJ., et al. “Intracoronary fixed dose of nitroprusside via thrombus aspiration catheter for the prevention of the no-reflow phenomenon following primary percutaneous coronary intervention in acute myocardial infarction”. Experimental and Therapeutic Medicine 6.2 (2013): 479-484.
- Giuseppe De Luca., et al. “Antman Time Delay to Treatment and Mortality in Primary Angioplasty for Acute Myocardial Infarction Circulation”. Circulation 109.10 (2004): 1223-1225.
- Sattur S., et al. “Correlation between markers of reperfusion and mortality in ST-elevation myocardial infarction: a systematic review”. Journal of Invasive Cardiology 26.11 (2014): 587-595.
Citation:
Udaya Prashant Ponangi., et al. “Intracoronary Infusion of Nicorandil Mixed with Contrast Through a Thrombus Aspiration
Catheter Placed Distally in the Culprit Vessel Reduces Incidence of No-Reflow and Slow-Flow in Acute Myocardial Infarction Patients
with a High Thrombus Burden.” Therapeutic Advances in Cardiology 1.1 (2017): 52-60.
Copyright: © 2017 Udaya Prashant Ponangi., et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.





























 Scientia Ricerca is licensed and content of this site is available under a Creative Commons Attribution 4.0 International License.
Scientia Ricerca is licensed and content of this site is available under a Creative Commons Attribution 4.0 International License.