Case Report
Volume 1 Issue 3 - 2017
An Unusual Cause of Optic Atrophy in Childhood
1W.K. Kellogg Eye Center, Michigan Medicine, Ann Arbor, USA
2Department of Biomedical Engineering, University of Michigan, Ann Arbor, USA
3University of Edinburgh, Edinburgh, Scotland
4Department of Ophthalmology, Queen Margaret Hospital, Dunfermline, Scotland
5Global health Implementation, University of St Andrews School of Medicine, St Andrews, Scotland
2Department of Biomedical Engineering, University of Michigan, Ann Arbor, USA
3University of Edinburgh, Edinburgh, Scotland
4Department of Ophthalmology, Queen Margaret Hospital, Dunfermline, Scotland
5Global health Implementation, University of St Andrews School of Medicine, St Andrews, Scotland
*Corresponding Author: Andrew Blaikie, Senior Lecturer, Global Health Implementation, University of St Andrews School of Medicine, St Andrews, Scotland.
Received: September 14, 2017; Published: September 26, 2017
Abstract
Purpose: To report a rare and interesting cause of bilateral optic atrophy secondary to hemolytic uremic syndrome (HUS).
Case Report: A 6-year-old asymptomatic child was referred with bilateral pale optic discs. She was otherwise healthy, with no known family history of any eye problems. On detailed questioning, it was revealed that she had HUS secondary to E. coli diarrheal infection at the age of 2.5 years, with renal failure that necessitated treatment with dialysis. Retinal nerve fiber analysis confirmed poor reserves with fewer axons in both eyes. The patient was followed up and discharged when there were no signs of progression.
Conclusion: Ocular involvement in HUS although rare, depicts a severe form of HUS, and may develop as sequelae to ischemic or toxic insults. Ophthalmology referral is required especially in preverbal patients with HUS to exclude potential vision-endangering consequences.
Keywords: Optic atrophy; Hemolytic uremic syndrome; Ophthalmology; Children; Dialysis
Abbreviations: HUS: Hemolytic Uremic Syndrome; OCT: Optical Coherence Tomography;
Introduction
We present a very unusual cause of optic atrophy that was identified on detailed clinical history.
Case Report
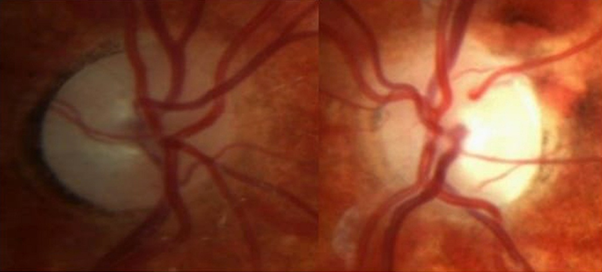
A 6-year-old female patient was referred by the optometrist to our local Ophthalmology department with bilateral pale optic discs. The patient did not report any ophthalmological problems. She denied any headaches, photophobia, malaise or night blindness, and did not have any problems with contrast sensitivity. Her birth history was unremarkable. On thorough questioning, it was revealed that she had hemolytic uremic syndrome (HUS) secondary to E. coli diarrheal infection at the age of 2.5 years, with renal failure that necessitated a short period of hemodialysis. She was otherwise healthy, and there was no family history of any eye related problems. Her visual acuity was 20/40 in the right eye and 20/20 in the left. She had no refractive errors. There was no afferent pupil defect, and her intraocular pressures were normal. Dilated fundoscopy showed pale, cupped discs in both eyes, which was worse in her right eye [Figure 1a and 1b].
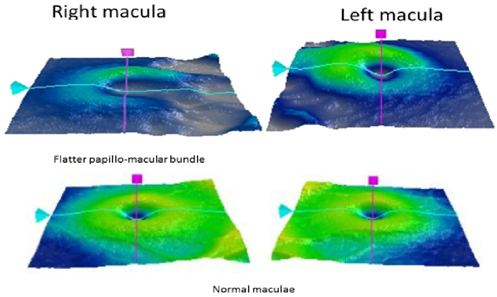
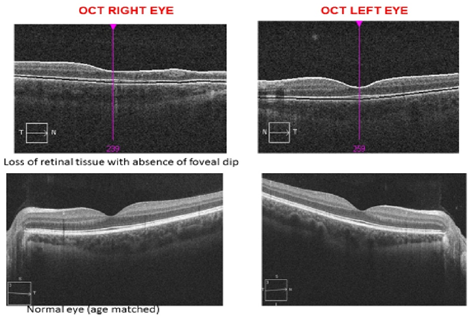
There was no evidence of retinal ischemia or neovascularization. Her parents and siblings had normal eye examinations. Her optical coherence tomography (OCT) confirmed a flatter papillo-macular bundle [Figure 2] with loss of foveal dip in the right eye [Figure 3]. OCT of her left eye was better in appearance [Figures 2 and 3].
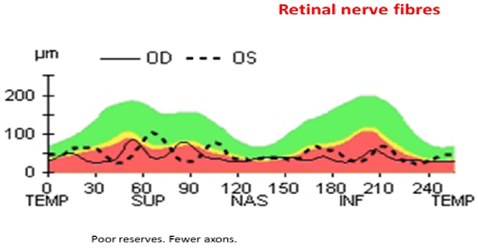
Retinal nerve fiber analysis supported poor reserves with fewer axons in both eyes [Figure 4]. The patient had serial examination by the same Ophthalmologist (AB). Her visual acuity, optic disc appearance, and OCT findings remained unchanged, and the patient was discharged from the eye clinic.
Discussion
Hemolytic-uremic syndrome, first defined in 1955, is a predominantly childhood disease characterized by a triad of microangiopathic hemolytic anemia, consumptive thrombocytopenia, and renal insufficiency. [1] HUS is the most common cause of acquired acute renal failure in childhood, with a 5 to 10% mortality rate. [2] The overall incidence of HUS in the United States is estimated at 2.1 cases per 100,000 persons/year, with a peak age incidence between six months and four years, and its incidence is increasing worldwide. [3] HUS is usually preceded by a prodrome of bloody diarrhea. Several causative agents have been implicated – the most common is Shiga-like toxin-producing E. coli HUS (STEC-HUS), triggered by E. coli O157:H7. [4] Most children with post diarrheal HUS, have a good chance of spontaneous recovery, with hospital observation and hemodialysis where indicated. Acute renal failure occurs in up to 70% of patients with STEC-HUS, although almost 85% recover their renal function. [2]
We report an unusual case of bilateral optic atrophy in pediatric case with HUS following E. coli infection. Ocular involvement in HUS although rare, depicts a severe form of HUS. Purtscher retinopathy, subhyaloid hemorrhage, chorioretinitis, ischemic signs and serous retinal detachment are serious eye conditions that are infrequently present in early stages of disease, and may be missed by the general pediatrician. [5-7] Bilateral optic atrophy is seen only in exceptional cases and may develop as sequelae to ischemic or toxic insults. [8,9] Anemia, hypoproteinemia, and intradialytic hypotension are known predisposing risk factors for anterior ischemic optic neuropathy. [9] However, the elevated blood viscosity and hematocrit during dialysis, may result in reduced blood flow and further increased risk of ischemia. Blindness from uremic optic neuropathy may occur, due to compromised vascular circulation, with potential reversibility with immediate dialysis. [10]
Conclusion
Ophthalmology referral is warranted especially in preverbal patients with HUS to exclude potential sight- threatening ramifications. Ophthalmologists also need to be vigilant in associating the patient’s ocular findings (which may be an early presentation of HUS) with serious underlying systemic disease such as vasculitis.
References
- Walsh PR and Johnson S. “Treatment and management of children with haemolytic uraemic syndrome”. Archives of Disease in Childhood (2017): 311377.
- Garg AX., et al. “Long-term renal prognosis of diarrhea-associated hemolytic uremic syndrome: a systematic review, meta-analysis, and meta-regression”. JAMA 290.10 (2003): 1360-1370.
- Corrigan JJ Jr and Boineau FG. “Hemolytic-uremic syndrome”. Pediatrics in Review 22.11 (2001): 365-369.
- Grisaru S. “Management of hemolytic-uremic syndrome in children”.International Journal of Nephrology and Renovascular Disease 7 (2014): 231-239.
- David R., et al.“Resolution of ocular involvement with systemic eculizumab therapy in atypical hemolytic-uremic syndrome”. Eye 27.8 (2013): 997-998.
- Sturm V., et al. “Ocular involvement in paediatric haemolytic uraemic syndrome”. Acta Ophthalmologica 88.7 (2010): 804-807.
- Nieto-Rios JF., et al. “Atypical haemolytic-uraemic syndrome in a young patient with renal, neurological, ocular and cardiovascular involvement”. Nefrologia 36. 1 (2016): 82-85.
- Siegler RL., et al. “Ocular involvement in hemolytic-uremic syndrome”. The Journal of Pediatrics 112.4 (1988): 594-597.
- Wortmann T., et al. “Bilateral anterior ischemic optic neuropathy following EHEC sepsis and hemolytic-uremic syndrome”. Der Ophthalmologe 110.7 (2013): 668-670.
- Seo JW., et al. “A case of end-stage renal disease initially manifested with visual loss caused by uremic optic neuropathy”. Hemodialysis International 15.3 (2011): 395-398.
Citation:
Andrew Blaikie., et al. “An Unusual Cause of Optic Atrophy in Childhood”. Ophthalmology and Vision Science 1.3 (2017): 125-
128.
Copyright: © 2017 Andrew Blaikie., et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.



































 Scientia Ricerca is licensed and content of this site is available under a Creative Commons Attribution 4.0 International License.
Scientia Ricerca is licensed and content of this site is available under a Creative Commons Attribution 4.0 International License.