Case Report
Volume 4 Issue 1
Management of Obstructive Sleep Apnea an Overview and Case Report
1Postgraduate resident in the specialty Program of Prosthodontics and Implantology, Department of Prosthodontics, Center for Dentistry, Oral Medicine, and Maxillofacial Surgery, Tuebingen University Hospital, Germany
*Corresponding Author: Abdulmajeed Okshah, Postgraduate resident in the specialty Program of Prosthodontics and Implantology, Department of Prosthodontics, Center for Dentistry, Oral Medicine, and Maxillofacial Surgery, Tuebingen University Hospital, Germany.
Received: December 18, 2019; Published: January 03, 2020
Abstract
Obstructive sleep apnea is prevalent in the general population with multifactorial etiology, therefore there are variety of treatment modalities. One of the management options is the use of mandibular devices, which seems to be preferred by many patients due to its comfortable fit, ease of transfer and cost effectiveness.
Keywords: Obstructive sleep apnea; dental sleep medicine; mandibular advancement device
Introduction
Obstructive sleep apnea (OSA) is the most common sleep-related breathing disorder which defined as a respiratory disorder characterized by partial and/or complete obstruction of the upper airway for more than 10 seconds [1]. It is a prevalent syndrome in general population with a prevalence rate range from 9%-38%. Although, the aetiology of OSA is believed to be multifactorial, it takes place usually due to collapse of upper airway. In spite of other predisposing factors it is mainly anatomical disorder [2].
Diagnosis of OSA should only be carried in medical setting by a specialized physician. The role of the dentist is either to recognize the problem and refer to the physician or to help with construction of oral appliances when needed [3]. The gold standard method of diagnosis is polysomnography. The American Academy of Sleep Medicine defined apnea/hypopnea index (AHI) as the number of apnea/hypopnea epi¬sodes per hour of sleep and classified OSA into mild from 5 to 15 apnea/hypopnea episo¬des per hour of sleep, moderate from 16 to 30, and severe over 30 [4].
There are two main treatment modalities of OSA treatment; namely surgical and non-surgical approaches. The selection of the treatment option depends mainly on the severity of the apnea. The aim of the therapy is to maintain the upper airway patency [5]. In 1995, the American Sleep Disorders Association Standards of Practice Committee has accepted the oral appliances treatment modality. This approach shows more preference and adherence by the patients because its simplicity, effectiveness in treating such disorders and the cost factor. The main idea behind such devices is to increase air flow through the oropharynx by repositioning the mandible downwards and forward [6].
Case Report
A 30 years old patient, in a medically fit status, was referred from Otolaryngologist for construction of oral appliance. According to the clinical and otorhinolaryngological evaluation, it was concluded that the patient had no significant anatomical alteration that could justify surgery, therefore the decision was made to use a mandibular repositioning appliance.
The physical examination showed that the general health status was good, the patient’s height was 1.85 m, and the weight was 80 kg.
Upon dental examination: the case was diagnosed of mild OSA acceding to his AHI score.
Polysomnography results were: AHI – 13.8/h; 86% minimum oxyhemoglobin saturation. The dental examination showed no pathology with satisfactory dental, peri¬odontal, and temporomandibular status. The AHI was classified as mild.
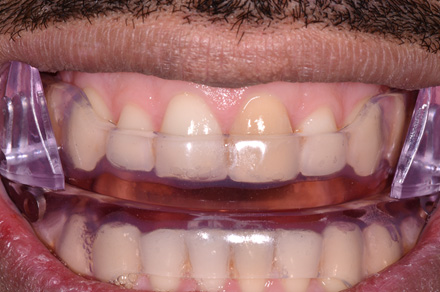
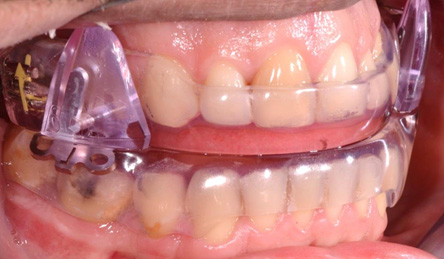
A mandibular advancement device MAD was constructed according to the manufacturer instructions. Figure 1 shows the appliance from the frontal point of view immediately after insertion and the degrees of protrusion of the mandible is illustrated in Figure 2.
Discussion
The treatment of OSA should be multidisciplinary because of its multifactorial aetiology. The treatment with MAD considered to be conservative and reversible therapy option. Patients who were treated with MAD showed enhancement of their quality of life as well as positive benefit of this method of therapy, namely its conservative approach [7].
Conclusion
Mandibular advancement devices MAD proved its effectiveness of reduction of the AHI score. And the patients showed better adherence and compliance with such devices. In the near future, the construction of such devices will be carried out with the modern digital technologies.
References
- Bixler EO., et al. “Prevalence of sleep-disordered breathing in women: effects of gender”. American Journal of Respiratory and Critical Care Medicine 163.3 (2001): 608-613.
- Senaratna CV., et al. “Prevalence of obstructive sleep apnea in the general population: A systematic review”. Sleep Medicine Reviews 34 (2017): 70-81.
- Quan SF and Schmidt-Nowara W. “The Role of Dentists in the Diagnosis and Treatment of Obstructive Sleep Apnea: Consensus and Controversy”. Journal of Clinical Sleep Medicine 13.10 (2017): 1117-1119.
- Jung DW., et al. “Apnea-hypopnea index prediction through an assessment of autonomic influence on heart rate in wakefulness”. Physiology & Behavior 169 (2017): 9-15.
- Zhou J and Liu YH. “A randomised titrated crossover study comparing two oral appliances in the treatment for mild to moderate obstructive sleep apnoea/hypopnoea syndrome”. Journal of Oral Rehabilitation 39.12 (2012): 914-922.
- Marklund M and Franklin KA. “Long-term effects of mandibular repositioning appliances on symptoms of sleep apnoea”. Journal of Sleep Research 16.4 (2007): 414-420.
- Aarab G., et al. “Long-term follow-up of a randomized controlled trial of oral appliance therapy in obstructive sleep apnea”. Respiration 82.2 (2011): 162-168.
Citation: Okshah A. “Management of Obstructive Sleep Apnea an Overview and Case Report”. Oral Health and Dentistry 4.1 (2020): 01-03.
Copyright: © 2020 Okshah A. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.



































 Scientia Ricerca is licensed and content of this site is available under a Creative Commons Attribution 4.0 International License.
Scientia Ricerca is licensed and content of this site is available under a Creative Commons Attribution 4.0 International License.