Mini Review
Volume 2 Issue 3 - 2018
Ultrasonography as a Diagnostic Tool for Salivary Gland Disorders
Oral Medicine Department, Faculty of Dentistry Universitas Padjadjaran, Bandung-Indonesia
*Corresponding Author: Nanan Nur’aeny, Oral Medicine Department, Faculty of Dentistry Universitas Padjadjaran, Bandung-Indonesia.
Received: January 01, 2018; Published: January 11, 2018
Abstract
Backgroud: Diagnosis of the patients with salivary gland disorders such as sialolithiasis (salivary stones), mucocele, ranula, and Sjogren’s syndrome can be made based on symptoms, past and present medical history, clinical examination, and supporting examination such as salivary gland imaging. Ultrasonography as one of the salivary gland imaging that is noninvasive and cost-effective especially for biopsy guidance and mass detection.
Purpose: This paper will discuss about the use of ultrasonography in establishing the diagnosis of salivary gland disorders.
Reviews: An ultrasonography uses sound waves, the echoes of the sound waves create a picture of the inside of the body. The advantages of ultrasonography can be useful for parotid and submandibular gland disorders but has limited only for the superficial locations, but is best to differentiate between intra- and extra glandular masses, as well as between cystic and solid lesions. Solid benign lesions present as well-circumscribed hypo echoic intra glandular masses. Ultrasonography can also demonstrate the presence of an abscess in an acute inflamed gland, as well as sialothiasis with echogenic densities that shows acoustic shadowing.
Conclusion: There are many salivary gland imaging that can be used to help in making the diagnose of salivary gland disorder, but as a dentist we should consider to use the ultrasonography eventhough still widely unknown however its benefits are rewarding.
Key words: Ultrasonography; Diagnosis; Salivary gland disorders
Introduction
Diagnosis of the patients with salivary gland disorders such as sialolithiasis (salivary stones), mucocele, ranula, and Sjogren’s syndrome can be made based on symptoms, past and present medical history, clinical examination, and supporting examination such as salivary gland imaging. There are two type of salivary gland imaging, radiation and non radiation imaging. Ultrasonography as one of salivary gland non radiation imaging that is noninvasive and cost-effective especially for biopsy guidance and mass detection. [1,2] The information about diagnostic tools in Dentistry especially for oral mucosal disease is still not much, so author will present the topic about the use of ultrasonography as a diagnostic tool for salivary gland disorders.
Review
In the early of 1950's, sonography was introduced in the Medical field. [3] USG uses high frequency sound waves (2-15 MHz) with wavelengths of 0,6-0,01 mm2 If sound strikes the interface between media, the energy reflects as an echo. The echoes of the sound waves create a picture of the inside of the body. [3] USG is best to differentiate between intra- and extraglandular masses, as well as between cystic and solid lesions. [1,5] The disadvantages of USG are limited visibility of deeper portions of gland, the result depends on the operator’s skill. [1,5]
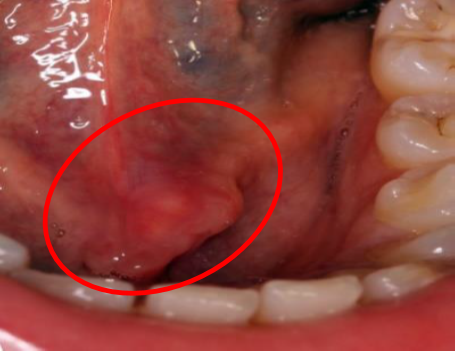
Sialolithiasis ia a condition of obstructive disorders of salivary gland. [4] Ccalcified organic matter that forms within the secretory system of the major salivary glands. [1] The material forms a mucinous plug that is comprised of viscous glycoproteins, bacteria, and epithelial debris. [6] (Figure 1)
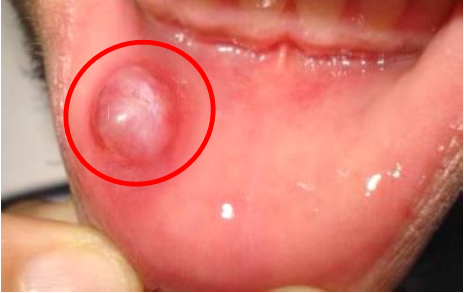
Mucocele is a swelling caused by pooling of saliva at the the site of injured minor salivary gland.4 Clinical feature of mucocele as a soft, fluctuant, and is walled-off by a rim of connective tissue yielding a cystic appearance. [4,5] most located on the lower lip (labial mucosa). [5] (Figure 2)
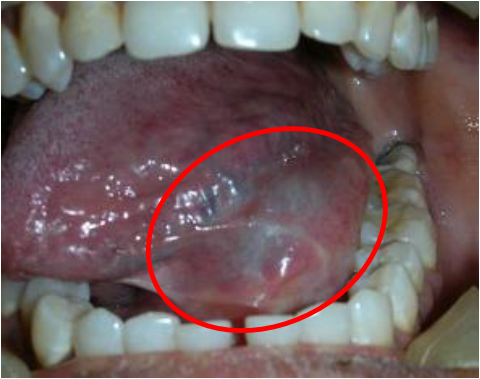
Ranula is a large mucocele occuring in the floor of the mouth, in association with ducts of submandibular or sublingual glands. [4] Ranula can occur as congenital or acquired condition. [9] There are two types of ranula i.e, superficial that associated with trauma of the sublingual glands, and plunging (ramifies deply into the neck). [4] (Figure 3)
Sjogren’s Syndrome (SS) is a chronic inflammatory disease that predominately affects salivary, lacrimal, and other exocrine glands. [4] SS classified as primary (without another autoimmune condition) and secondary (with the presence of connective tissue disorder. [1,11]
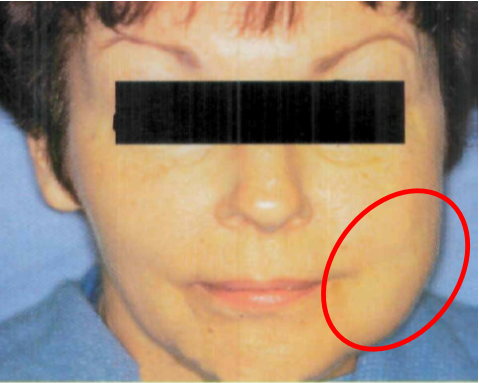
Figure 4: Clinical presentation of chronic unilateral parotid salivary gland enlargement in patient with Sjogren's syndrome. [1]
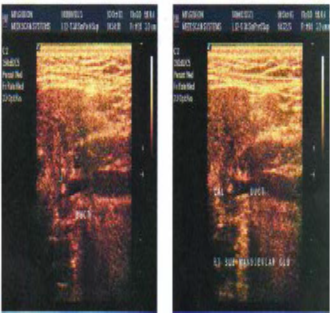
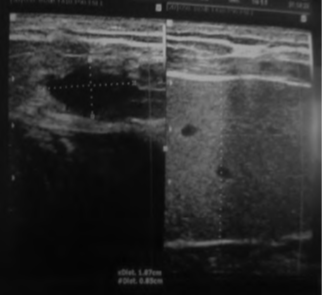
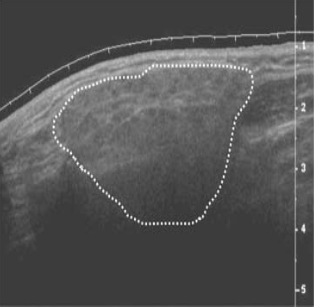
Salivary gland diseases are diverse ranging from the minor inflammatory conditions to a diverse group of benign and malignant neoplasms. [12] The value of Ultrasonography is well recognized in inflammatory soft tissue conditions of the head and neck region and superficial tissue disorders of the maxillofacial region. USG can provide the content of the lesion before any surgical procedure, both solid and cystic contents could be identified in USG. Sialoliths in parotid, submandibular and sublingual salivary glands can be detected by USG which appear as echo-dense spots with a characteristic of acoustic shadow. [3] (Figure 5) Mucocele and ranula also can be identified from USG imaging, it can revealed a space occupying mass, which was cyst like with capsule (Figure 6). It contained concentrated liquid. There was no blood vessel. The cyst was across the midline slightly and had a pressure effect on surrounding structures. From these findings, solid tumors such as pleomorphic adenoma and monomorphic adenoma could be rejected. [13] In Sjögren’s Syndrome the affected glands become less well defined, appear slightly darker (hypo echoic) than a normal gland, loose their uniform (homogenous) structure to show numerous, dark circular areas (Figure 7). The number and size of these dark areas appears to match the severity of the condition. Typically the foci vary in size but are usually round or ovoid, about 2-5 mm in diameter and are non-vascular. Foci larger than this, suggest more extensive damage and require careful follow up or monitoring. [11]
Conclusion
There are many salivary gland imaging can be used including radiation and non-radiation imaging. Ultrasonography (USG) is a non-radiation imaging, inexpensive, and readily available imaging technique that can be used to make diagnosis of salivary gland disorder such as sialolithiasis, mucocele, ranula, and Sjogren's syndrome. As a dentist we can consider to use ultrasonography eventhough is still widely unknown but their benefit are rewarding.
References
- Fox PC and Ship JA. “Salivary Gland Disease in Burket’s Oral Medicine. 11th edition”. Hamilton: BC Decker Inc. (2008): 191-213.
- Scully C. Oral and Maxillofacial Medicine, 2nd edition. Edinburgh: Churchill Livingstone Elsevier. (2008): 279-287.
- Kumar S and Mahahob N. “Ultrasound in Dentistry-A Review”. Journal of Indian Academy of Dental Specialist Researchers 1.4 (2010): 44-45.
- Ghom AG. Textbook of Oral Medicine. 1st edition. New Delhi: Jaypee Brothers Medical Publishers (P) Ltd. (2005): 561-583.
- Bradley and Lichius G. “Salivary Gland Disorders and Diseases: Diagnosis and Management”. George Thieme Verlag KG (2011): 58-59.
- Silverman S., et al. Essential of Oral Medicine.Hamilton: BC Decker Inc. (2002): 260-276.
- Maljkovic V and Gaspirc B. “Case Report: Laser-Assisted Treatment of Sialolithiasis”. Journal of the Laser and Health Academy 1 (2014): 45-46.
- Shamim T. “Oral Mucocele (Mucous Extravasation Cyst)”. Journal of Ayub Medical College Abbottabad 21.1 (2009): 169.
- Singh BG., et al. “A Rare Case of Congenital Simple Cystic Ranula in a Neonate”. Case Reports in Otolaryngology (2013): 1-3.
- Hallur N., et al. “Management of Ranula”. International Journal of Dental Clinics 3.3 (2011): 79-80.
- Rout J. “Radiographic Diagnosis of Sjӧgren's syndrome”. British Sjӧgren's Syndrome Association 24.4 (2009): 1-3.
- Sindhar T and Gnanasundaran N. “Ultrasonograpic Evaluation of Salivary Gland Enlargement: A Pilot Study”. International Journal of Dental Sciences and Research 102 (2013): 28-35.
- Sheiki M., et al. “Plunging Ranula of the Submandibular Area”. Dental Research Journal 8. S1 (2011): 114-118.
Citation:
Nanan Nur’aeny and Riani Setiadhi. “Ultrasonography as a Diagnostic Tool for Salivary Gland Disorders”. Oral Health and
Dentistry 2.3 (2018): 393-397.
Copyright: © 2018 Nanan Nur’aeny and Riani Setiadhi. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.



































 Scientia Ricerca is licensed and content of this site is available under a Creative Commons Attribution 4.0 International License.
Scientia Ricerca is licensed and content of this site is available under a Creative Commons Attribution 4.0 International License.