Review Article
Volume 1 Issue 5 - 2017
Advances in Local Anesthesia Drug Delivery Systems –A Review
1PG student, Meenakshi Ammal Dental College and hospital, Chennai, India
2Reader, Meenakshi Ammal Dental College and Hospital, Chennai, India
2Reader, Meenakshi Ammal Dental College and Hospital, Chennai, India
*Corresponding Author: Ditto Sharmin, Reader, Meenakshi Ammal Dental College and Hospital, Chennai, India.
Received: August 26, 2017; Published: October 04, 2017
Introduction
Pain is an unpleasant sensory and emotional experience associated with actual or potential tissue damage, or described in terms of such damage [1]. Pain management, also called algiatry, employs an interdisciplinary approach for easing the suffering and improving the quality of life of those experiencing pain [2]. Because of the fear of pain in dental injections, some people avoid, cancel or do not appear for dental appointments [3]. Although Cook invented the modern dental syringe more than one hundred years ago, only recently many innovations have been added to the traditional methods of drug delivery systems. These include computer controlled local anaesthetic delivery systems, the wand, vibrato tactile devices like VibraJect, Accupal, Dental Vibe, Syringe micro vibrator, Jet injections, Intra osseous anaesthesia systems like Stab dent, X tip, Interflows, Safety dental devices, Dent patches etc. This review will discuss the above mentioned devices and their applications in the field of dentistry.
Computer Controlled Local Anesthesia Delivery Systems
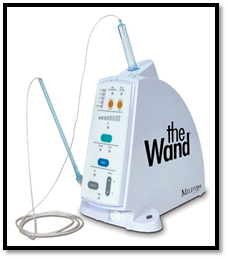
Milestone Scientific (Piscataway, NJ, USA) introduced the first C-CLAD system in the United States in 1997. Originally known as the Wand and then subsequently the versions were sequentially renamed as the Wand Plus and then Compu Dent which is currently being used [4].
Milestone Scientific (Piscataway, NJ, USA) introduced the first C-CLAD system in the United States in 1997. Originally known as the Wand and then subsequently the versions were sequentially renamed as the Wand Plus and then Compu Dent which is currently being used [4].
The CompuDent system has 3 components–a base unit, a foot pedal and a disposable handpiece assembly. The base unit has a microprocessor and connects to both the foot pedal and the handpiece assembly. The microprocessor controls a piston that expresses local anesthetic by pushing the plunger into the cartridge. The anesthetic solution is then forced through the microbore tubing, Wand handpiece and attached needle into the tissues [5].
The lightweight hand piece is held in a pen grasp that provides the user with greater tactile sensation and control compared to a traditional syringe. The available flow rates of local anesthetic delivery are controlled by a computer and thus remain consistent from one injection to the next. The greater control over the syringe and the fixed flow rates of the local anesthetic drug are responsible for a significantly improved injection experience, as demonstrated in many clinical studies conducted with CCLAD devices in dentistry. LA solution from the cartridge passes through the microbore tubing in the Handpiece assembly and attached needle into the target tissue. Rate of Injection: foot pedal controls the rate of injection and if aspiration feature is enabled, it prevents inadvertent intravascular injections. Flow rates for these devices are categorised as-
- Slow: 0.005ml/s – needle insertion, PDL injection, and Palatal administration
- Fast: 0.03ml/s – buccal infiltrations, nerve block
- Turbo: 0.06ml/s. [6-10]
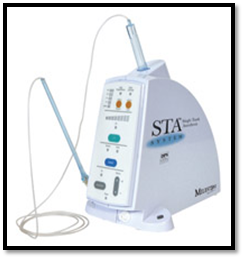
“Single Tooth Anesthesia System – STA System” was introduced by Milestone Scientific in 2007. Its advantages include „Dynamic Pressure Sensing – DPS‟ which provides continuous feedback to the user about the pressure at the needle tip to identify the ideal needle placement for PDL injections. It runs of 3 modes of flow rates,, which are -
- STA mode: Single, slow rate of injection
- Normal mode: emulates the Compudent device
- Turbo mode: faster rate of injection – 0.06ml/s
Vibratotactile Devices
These devices are aimed at easing the fear of the needle by taking advantage of the gate control theory of pain management. Vibrotactile stimuli are used to relieve pain of injection. Vibrations or pressure act as non-noxious stimuli, which modify or interfere with pain signals by closing the neural gate of cerebral cortex. This reduces the perception of pain as cerebral cortex gets focused on the vibration hence the perception of “pain” from the pressure of the liquid entering the tissue is decreased due to distraction [10]. Inui and colleagues suggested that pain reduction due to non-noxious touch or vibration results from tactile induced pain inhibition within the cerebral cortex itself and that the inhibition occurs without any contribution at spinal level, including descending inhibitory actions on spinal neurons [11].
These devices are aimed at easing the fear of the needle by taking advantage of the gate control theory of pain management. Vibrotactile stimuli are used to relieve pain of injection. Vibrations or pressure act as non-noxious stimuli, which modify or interfere with pain signals by closing the neural gate of cerebral cortex. This reduces the perception of pain as cerebral cortex gets focused on the vibration hence the perception of “pain” from the pressure of the liquid entering the tissue is decreased due to distraction [10]. Inui and colleagues suggested that pain reduction due to non-noxious touch or vibration results from tactile induced pain inhibition within the cerebral cortex itself and that the inhibition occurs without any contribution at spinal level, including descending inhibitory actions on spinal neurons [11].
Vibraject
It is a battery operated attachment that fits on to the standard dental syringe. It produces a mild vibrating sensation which helps override the pain signals from the needle. When vibration and pain are combined, it is believed that vibration message carried out by the nerves, predominates over pain based on the gate control theory of pain by Melzack and Wall. So the patient experiences only vibrations and not pain. In a study conducted by Nanitos., et al. titled “The effect of vibration on pain during local anaesthesia injections” subjects were asked to rate anticipated and actual pain from regional anaesthetic injections in the oral cavity.
It is a battery operated attachment that fits on to the standard dental syringe. It produces a mild vibrating sensation which helps override the pain signals from the needle. When vibration and pain are combined, it is believed that vibration message carried out by the nerves, predominates over pain based on the gate control theory of pain by Melzack and Wall. So the patient experiences only vibrations and not pain. In a study conducted by Nanitos., et al. titled “The effect of vibration on pain during local anaesthesia injections” subjects were asked to rate anticipated and actual pain from regional anaesthetic injections in the oral cavity.
A second study compared, within subjects, pain from injections with and without a simultaneous vibration stimulus. Both infiltration and block anaesthetic injection techniques were assessed. In each subject, two similar injections were given and with one, a vibration stimulus was randomly allocated. Injection pain was assessed by visual analogue scale and McGill pain descriptors. The results suggest that vibration can be used to decrease pain during dental local anaesthetic administration. [13]
Dental Vibe
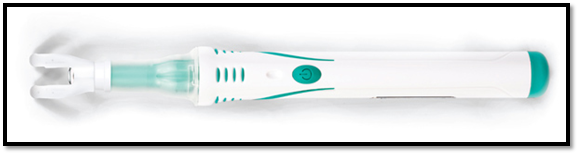
Dental vibe is a cordless hand held device which gently stimulates the sensory receptors at the injection site causing the neural pain gate to close. The advantage of this is, the tissues are vibrated before the needle penetrates same as the principle Vibraject works on. But the disadvantage is, it is not directly attached to the syringe and a separate unit is required, so both hands are engaged. Dental vibe and syringe micro vibrator uses micro-vibration to the site where an injection is being administered [15].
Dental vibe is a cordless hand held device which gently stimulates the sensory receptors at the injection site causing the neural pain gate to close. The advantage of this is, the tissues are vibrated before the needle penetrates same as the principle Vibraject works on. But the disadvantage is, it is not directly attached to the syringe and a separate unit is required, so both hands are engaged. Dental vibe and syringe micro vibrator uses micro-vibration to the site where an injection is being administered [15].
Accupal
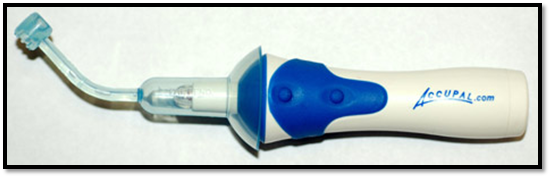
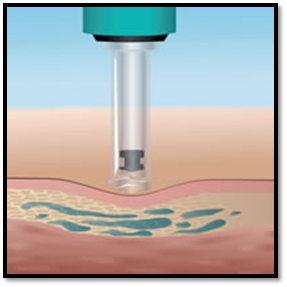
The Accupal (Hot Springs, AR, USA) is a cordless device that uses both vibration and pressure to precondition the oral mucosa. Accupal provides pressure and vibrates the injection site 360° proximal to the needle penetration, and these vibrations shuts the “pain gate,” according to the manufacturer. After placing the device at the injection site and applying moderate pressure, the unit light up the area and begins to vibrate. The needle is placed through a hole in the head of the disposable tip, which is attached to the motor16. Using these vibrations, the pain sensation is drastically reduced for the patient.
The Accupal (Hot Springs, AR, USA) is a cordless device that uses both vibration and pressure to precondition the oral mucosa. Accupal provides pressure and vibrates the injection site 360° proximal to the needle penetration, and these vibrations shuts the “pain gate,” according to the manufacturer. After placing the device at the injection site and applying moderate pressure, the unit light up the area and begins to vibrate. The needle is placed through a hole in the head of the disposable tip, which is attached to the motor16. Using these vibrations, the pain sensation is drastically reduced for the patient.
Jet Injections
Jet injection technology is based on the principle of using a mechanical energy source to create a release of pressure sufficient to push a dose of liquid medication through a very small orifice, creating a thin column of fluid with enough force that it can penetrate soft tissue into the subcutaneous tissue without a needle [17]. Especially indicated for when the local anesthetic can be deposited subcutaneously. The advantage is that this is a needleless injection system, hence patient compliance is better as there is no needle.
Jet injection technology is based on the principle of using a mechanical energy source to create a release of pressure sufficient to push a dose of liquid medication through a very small orifice, creating a thin column of fluid with enough force that it can penetrate soft tissue into the subcutaneous tissue without a needle [17]. Especially indicated for when the local anesthetic can be deposited subcutaneously. The advantage is that this is a needleless injection system, hence patient compliance is better as there is no needle.
Syrijet
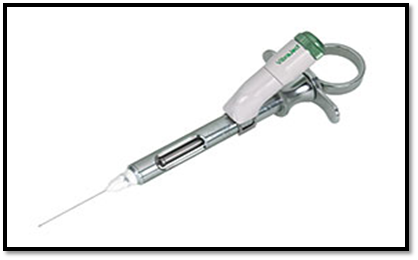
Syrijet is a needleless injector that reduces patient apprehension by eliminating painful and unsightly needles. Syrijet is a precision instrument designed for simple, reliable operation. It saves time and effort, and eliminates unnecessary patient discomfort and needle apprehension.
Syrijet is a needleless injector that reduces patient apprehension by eliminating painful and unsightly needles. Syrijet is a precision instrument designed for simple, reliable operation. It saves time and effort, and eliminates unnecessary patient discomfort and needle apprehension.
Syrijet assures reliable anesthesia for successful operative and surgical procedures in both upper and lower anterior areas, and for all procedures on deciduous teeth. The Syrijet instrument comes with rubber covers to ensure infection control and easy cleaning (autoclavable). The sleek looking injector is made of aluminium for even weight distribution and easy handling. It uses standard 1.8 cc local anesthetic cartridges with a volume control ranging from .05 to 20cc.
Intra Osseous Injections
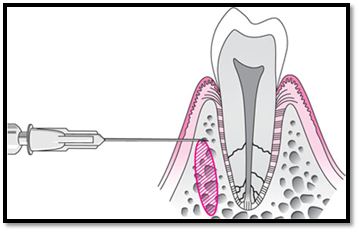
Aim of intra-osseous anesthesia is to inject local anesthesia solution into cancellous bone adjacent to the apex of the tooth by piercing buccal gingiva and bone in relation to the tooth to be anesthetized. It can be used as a supplemental technique with mandibular nerve blocks to enhance deep pulpal anesthesia or as a primary technique so that patients do not experience numb lips or tongues postoperatively [19]. Limitation of this is that, is can be used only as a supplemental anesthesia option for deep pulpal anesthesia.
Aim of intra-osseous anesthesia is to inject local anesthesia solution into cancellous bone adjacent to the apex of the tooth by piercing buccal gingiva and bone in relation to the tooth to be anesthetized. It can be used as a supplemental technique with mandibular nerve blocks to enhance deep pulpal anesthesia or as a primary technique so that patients do not experience numb lips or tongues postoperatively [19]. Limitation of this is that, is can be used only as a supplemental anesthesia option for deep pulpal anesthesia.
Stab dent
A slow‑speed hand piece with a latch contra‑angle for the perforator and a standard dental anesthetic syringe for the needle. It has a solid 27-guage wire with a bevel end that when activated, drills a small hole through the cortical plate. The main disadvantage of the device is that the perforation needs to be made in a reasonably accessible and visible location in the attached gingiva distal to the tooth to be anesthetized. If the penetration zone is located in alveolar mucosa that moves once the perforator is withdrawn, it can be extremely difficult to locate the perforation site with the anesthetic needle [18].
A slow‑speed hand piece with a latch contra‑angle for the perforator and a standard dental anesthetic syringe for the needle. It has a solid 27-guage wire with a bevel end that when activated, drills a small hole through the cortical plate. The main disadvantage of the device is that the perforation needs to be made in a reasonably accessible and visible location in the attached gingiva distal to the tooth to be anesthetized. If the penetration zone is located in alveolar mucosa that moves once the perforator is withdrawn, it can be extremely difficult to locate the perforation site with the anesthetic needle [18].
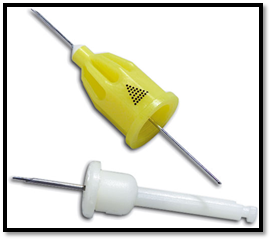
X Tip
In view of above difficulty of Stab dent system to locate the perforation hole, the X Tip solves this problem by making the pilot drill through which a 27‑gauge needle can pass. The initial drill stays in place, allowing the anesthetic to be placed without hunting for the hole that was just created. The X Tip has been reported to have more post‑operative pain in males, 1 to 3 days after the procedure, which may be contributed to by increased heat formation during perforation because of the X Tip’s wider diameter of the drill and guide sleeve [17]. It works in areas that lack attached gingiva or that lack easily visible access.
In view of above difficulty of Stab dent system to locate the perforation hole, the X Tip solves this problem by making the pilot drill through which a 27‑gauge needle can pass. The initial drill stays in place, allowing the anesthetic to be placed without hunting for the hole that was just created. The X Tip has been reported to have more post‑operative pain in males, 1 to 3 days after the procedure, which may be contributed to by increased heat formation during perforation because of the X Tip’s wider diameter of the drill and guide sleeve [17]. It works in areas that lack attached gingiva or that lack easily visible access.
Intra flow
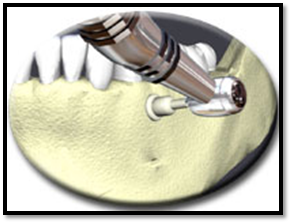
The Intra Flow (Pro Dex Medical Devices, Irvine, CA, USA) device is essentially a dental handpiece equipped with an injection system built into the body. The biggest advantage of the Intra Flow anesthesia system is that it allows entry into the penetration zone, injection, and withdrawal in one continuous step, without the need to relocate the perforation site. This single‑step method can be helpful in penetration zones that are difficult to visualize or access, such as the second and sometimes the first molar areas, or where there is horizontal bone loss or a limited band of attached gingiva in the desired penetration zone. One recent study found Intra Flow to provide reliable anesthesia of posterior mandibular teeth in 13 of 15 subjects, compared to 9 of 15 with an inferior alveolar nerve block [19].
The Intra Flow (Pro Dex Medical Devices, Irvine, CA, USA) device is essentially a dental handpiece equipped with an injection system built into the body. The biggest advantage of the Intra Flow anesthesia system is that it allows entry into the penetration zone, injection, and withdrawal in one continuous step, without the need to relocate the perforation site. This single‑step method can be helpful in penetration zones that are difficult to visualize or access, such as the second and sometimes the first molar areas, or where there is horizontal bone loss or a limited band of attached gingiva in the desired penetration zone. One recent study found Intra Flow to provide reliable anesthesia of posterior mandibular teeth in 13 of 15 subjects, compared to 9 of 15 with an inferior alveolar nerve block [19].
Safety Dental Syringes
Aim of these devices is to prevent from the risk of accidental needle stick injury occurring with a contaminated needle after local anesthesia administration. These syringes possess a sheath that locks over the needle when it is removed from the patient’s tissues preventing accidental needle stick injury [12]. Examples include, 1. Ultra safe syringe, 2. Ultra safety plus XL syringe, 3.hyposafety syringe, 4.safety wand 5. Rev Vac safety syringe.
Aim of these devices is to prevent from the risk of accidental needle stick injury occurring with a contaminated needle after local anesthesia administration. These syringes possess a sheath that locks over the needle when it is removed from the patient’s tissues preventing accidental needle stick injury [12]. Examples include, 1. Ultra safe syringe, 2. Ultra safety plus XL syringe, 3.hyposafety syringe, 4.safety wand 5. Rev Vac safety syringe.
Dent patches
The DentiPatch' is a mucoadhesive patch containing 46.1 mg of lidocaine (20% concentration). This patch is a site-specific drug delivery that purportedly maximizes the effect of lidocaine diffusing into a localized mucosal site to reduce the pain associated with injections. The onset of anesthesia may occur as early as 2.5 minutes after application, and the patch can be left in place for up to 15 minutes.
The DentiPatch' is a mucoadhesive patch containing 46.1 mg of lidocaine (20% concentration). This patch is a site-specific drug delivery that purportedly maximizes the effect of lidocaine diffusing into a localized mucosal site to reduce the pain associated with injections. The onset of anesthesia may occur as early as 2.5 minutes after application, and the patch can be left in place for up to 15 minutes.
Conclusion
Local anesthetics have made a great progress in the field dentistry and have changed patients’ perspectives towards dental procedures. Although there are great advances in the field of local anesthesia delivery systems, there is still room for the improvement of painless administration of local anesthesia. It is important for dentists to be familiar with all the available local anesthesia devices in the market and techniques available for dental procedures to achieve painless delivery of the solution.
References
- IASP Task Force on Taxonomy: Part III: Pain Terms, a Current list with Definitions and Notes on Usage In Classifiction of Chronic Pain_2 edition. Edited by Merskey H and Bogdunk N WA, Seattle; IASP Press (1994): 209-214.
- Hardy PAJ. “Chronic pain management: the essentials”. UK; Greenwich Medical Media; (1997):13.
- Milgram P., et al. “Four dimensions of fear of dental injections”. The Journal of the American Dental Association 128.6 (1997): 756-766.
- Ring ME. “The history of local anesthesia.” Journal of the California Dental Association 35.4 (2007): 275-282.
- Taylor M. Clark, John A. Yagiela. Dental Clinics of North America 54 (2010): 757-768.
- Gibson RS., et al. “The Wand vs. traditional injection: A comparison of pain related behaviors”. Journal of Pediatric Dentistry 22.6 (2000): 458-462.
- Nicholson JW., et al. “Pain perception anvisid utility: A comparison of the syringe and computerized local injection techniques”. General Dentistry 49.2 (2001): 167-172.
- Fukayama H., et al. “Efficacy of anterior and middle superior alveolar (AMSA) anesthesia using a new injection system: The Wand”. Quintessence International 34.7 (2003): 537-541.
- Perry DA and Loomer PM. “Maximizing Pain Control. The AMSA Injection can provide anesthesia with few injections and less pain”. Dimensions of Dental Hygiene 1 (2003): 28-33.
- Melzac R and Wall PD. “Pain mechanisms: A new theory Science”. Science 150.3699 (1965): 971-979.
- SS Sharma., et al. “Newer Local Anaesthetic Drugs and Delivery Systems in Dentistry – An Update”. IOSR Journal of Dental and Medical Sciences 1.4 (2012):10-16.
- Saxena., et al. “Advances in dental local anesthesia techniques and devices: An update”. National journal of maxillofacial surgery 4.1 (2013): 19-24.
- Invik k., et al. “Temporal analysis of cortical mechanism for pain relief by tactile stimuli in humans”. Cereb Cortex 16.3 (2006): 355-65.
- Ogle OE and Mahjoubi G. “Advances in local anesthesia in dentistry”. Dental Clinics of North America 55.3 (2011): 481-499.
- Nanitos E., et al. “The effect of vibration on pain during local anaesthesia injections”. Australian Dental Journal 54.2 (2010): 94-100.
- Blani J. “Vibraject from ITL dental”. Dental Economics 92 (2002): 90.
- M.P. Santhosh Kumar. Journal of Pharmaceutical Sciences and Research 7.5 (2015): 252-255.
- Available from: http://www.accupal.com (visited on 21/12/2016).
- Clark TM and Yagiela JA. “Advances technique and armamentarium for dental local anesthesia”. Dental Clinics of North America 54.4 (2010): 757-768.
- Remmers T., et al. “The efficacy of IntraFlow intraosseous injection as a primary anesthesia technique”. Journal of Endodontics 34.3 (2008): 280-283.
Citation:
Ditto Sharmin and Sravanthi Sistla. “Advances in Local Anesthesia Drug Delivery Systems –A Review”. Oral Health and Dentistry
1.5 (2017): 237-244.
Copyright: © 2017 Ditto Sharmin and Sravanthi Sistla. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.





































 Scientia Ricerca is licensed and content of this site is available under a Creative Commons Attribution 4.0 International License.
Scientia Ricerca is licensed and content of this site is available under a Creative Commons Attribution 4.0 International License.