Research Article
Volume 3 Issue 1 - 2019
Radiculitis an Agony and Present Approach
1MBBS (MGIMS), MD (Internal Medicine), DNB (E&M), PhD Postgraduate in Endocrinology & Metabolism (AIIMS Delhi), Chairman National Institute of Health & Research Warisaliganj (Nawada) Bihar India
2BAMS (BRABU), MHA Director (Hon), Aarogyam Punarjeevan Ram Bhawan, Ara Garden Road, Jagdeopath, Baily Road Patna
3BAMS (BRABU), Ex Director Centre for Indigenous Medicine & Research Senior Research Fellow Regional Institute of Ayurveda, Itanagar Arunachal Pradesh
2BAMS (BRABU), MHA Director (Hon), Aarogyam Punarjeevan Ram Bhawan, Ara Garden Road, Jagdeopath, Baily Road Patna
3BAMS (BRABU), Ex Director Centre for Indigenous Medicine & Research Senior Research Fellow Regional Institute of Ayurveda, Itanagar Arunachal Pradesh
*Corresponding Author: Avinash Shankar, MBBS (MGIMS), MD (Internal Medicine), DNB (E&M), PhD Postgraduate in Endocrinology & Metabolism (AIIMS Delhi), Chairman National Institute of Health & Research Warisaliganj (Nawada) Bihar India.
Received: May 01, 2019; Published: June 21, 2019
Abstract
Radiculitis, an agonizing painful condition caused by inflammation of the spinal nerve root or roots in the region of neural foramen and its presentation is termed as Radiculopathy which commonly affect the cervical and lumbar region
Inspite of advancement in diagnostics i.e- CT scan and MRI and treatment with traction,surgical decompression and other adjuvant like neuro vitamin supplementation and analgesic antiarthritic supplementation satisfactory clinical response with improved quality of life reamain a challenge even after surgery ,thus a therapeutic regime constituting herbal neurotonic and neuro vigorative both as oral and transdermal application been evaluated in patients who failed to respond the conventional therapeutic measures i.e- conservative and even surgery
Objective of study: To assess the herbal neurogenic containing therapeutic regime in ensuring clinical relief and improving quality of life in patients of radiculitis.
Material and Method: Seven hundred eighteen already diagnosed and treated non responsive cases of radiculitis attending at Centre For Critical Care ,National Institute of Health & Research Warisaliganj (Nawada)Bihar been selected ,interrogated, examined clinically ,assessed and analysed their previous investigation reports ,therapeutics taken and their effect.
Irrespective of their clinical severity and previous therapeutic state all patients were advocated the prescribed regime and were followed for post therapy 2 years for which patients been given a follow up card to record the changes.
Result: Patients of mild, moderate and severe grade of clinical presentation shows grade I clinical response with improved quality of life in 100%, 80.2% and 88.4% patients respectively, though 0.9% and 1.9% of moderate and severe grade of clinical severity fails to prove worth.
No patients of either status had alteration in bio parameters or any adversity during therapy or 2 years of post therapy follow up.
Key Words: Radiculitis; Radiculopathy; Cervical; lumbar; CT; MRI; herbal neurogenic; Neuro vigorative; quality of life
Introduction
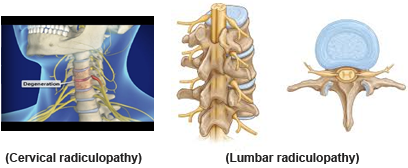
Radiculitis synonym of radicular pain i.e.- alteration in sensation or muscle power produced due to inflammation of spinal nerve root Or roots in the region of neural foramen and its presentation is termed as Radiculopathy Or Pinched nerve with common presentation as – Pain, weakness, numbness or difficulty in controlling specific muscles [1]. On basis of its common area of involvement i.e.- cervical and lumbar region it is also known as Cervical and lumbar Radiculitis or radiculopathy
The incidence of low back pain is estimated to be 5% to more than 30% with a lifetime prevalence of 60% to 90%. Approximately 50% of cases will resolve within one to two weeks. 90% of cases will resolve in six to 12 weeks. The incidence of radicular symptoms in patients presenting with low back pain ranges from 12% to 40%. While an annual incidence of cervical radiculopathy of 107.3 per 100,000 for men and 63.5 per 100,000 for women with a peak at 50 to 54 years of age. [2,3]
It is mechanical compression of nerve root usually at the exit foramen or lateral recess secondary to degenerative disc disease, osteo arthritis, facet degeneration or hypertrophy, ligamentous hypertrophy, spondylolisthesis or its combination though rarely also caused by radiation, diabetes mellitus, neoplastic disease Or any meningeal disease. [4,5,6]
| Common presentation | Preceding factors |
| Agonising pain in the back | Accidental injury |
| Pain during walking | Heavy weight lifting |
| Pain during changing posture | Recurrent fever & debility |
| Pain in neck | Diabeties mellitus |
| Tingling numbness in the extremity | Post parturition in female |
As per American College of Radiology projectional radiography is an appropriate tool for initial study, Magnetic resonance imaging (MRI) of the portion of the spine. Electrodiagnostic testing, consisting of NCS (nerve conduction study) and EMG (electromyography), are more significant and specific diagnostic tool to ascertain nerve root injury. Needle EMG is considered most sensitive tool to reveal active denervation in the distribution of the involved nerve root, and neurogenic-appearing voluntary motor units in more chronic radiculopathies [7,8,9]
Present therapeutics i.e.- traction, cervical collar or abdominal belt, transdermal steroid injection, epidural injection, analgesics, calcium supplementation ,vitamin D3 supplementation ,fails to ensure cure in all the cases thus a therapeutic regime containing herbal neuro rejuvenator been evaluated for its clinical efficacy and safety profile. [10-14]
Objective of the study
To assess the herbal neurogenic containing therapeutic regime in ensuring clinical relief and improving quality of life in patients of radiculitis
To assess the herbal neurogenic containing therapeutic regime in ensuring clinical relief and improving quality of life in patients of radiculitis
Duration of study
January 1014 to December 2016 with 2 years rigorous follow up from January 2017-December 2018 for post therapy symptom withdrawal or any drug adversity.
January 1014 to December 2016 with 2 years rigorous follow up from January 2017-December 2018 for post therapy symptom withdrawal or any drug adversity.
Material and Methods
Material
Patients of radiculopathy treated and non responsive to present therapeutics attending Centre For Critical Care National Institute of Health & Research Warisaliganj were selected for evaluation of the present therapeutic regime clinical efficacy and safety profile.
Patients of radiculopathy treated and non responsive to present therapeutics attending Centre For Critical Care National Institute of Health & Research Warisaliganj were selected for evaluation of the present therapeutic regime clinical efficacy and safety profile.
Methods
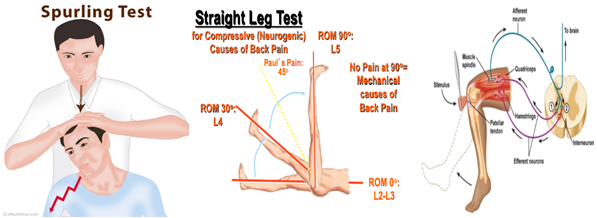
Selected patients and their attendants were thoroughly interrogated for onset of disease, clinical presentation, therapeutics taken and their response, any untoward effect or exacerbation of clinical presentation, preceding factors, clinically examined (Sparling’s test for Cervical radiculitis and Straight leg raising test (SLR) for lumbar radiculitis. In addition, deep tendon reflex (Stretch reflex) was also elucidated. [15,16]
Selected patients and their attendants were thoroughly interrogated for onset of disease, clinical presentation, therapeutics taken and their response, any untoward effect or exacerbation of clinical presentation, preceding factors, clinically examined (Sparling’s test for Cervical radiculitis and Straight leg raising test (SLR) for lumbar radiculitis. In addition, deep tendon reflex (Stretch reflex) was also elucidated. [15,16]
The Spurling test is a medical maneuver to assess nerve root pain (also known as radicular pain). The examiner turns the patient's head to the affected side while extending and applying downward pressure to the top of the patient's head. A positive Spurling's sign is when the pain arising in the neck radiates in the direction of the corresponding dermatome ipsilaterally. It is a type of cervical compression test
The straight leg raise, also called Lasègue's sign, Lasègue test or Lazarević's sign, is a test done during a physical examination to determine whether a patient with low back pain has an underlying herniated disc, often located at L5 (fifth lumbar spinal nerve).
As selected patients were already under gone for various investigation X-ray of the region, MRI, Test for tuberculosis, blood sugar and other haematological test hence basic bio parameters were repeated to adjudge the drug adversity on haematological, hepatic and renal parameters
The selected patients were classified in three groups as per their severity i.e. mild, moderate and severe
| Severity Grade | Characteristics |
| Mild | Pain in the affected region (Shoulder/back) |
| Moderate | Pain, tingling and numbness, inability to move upper Extremity |
| Severe | Agonizing pain, tingling and numbness, inability to walk And raise upper extremity |
Patients irrespective of their severity grade in addition to –
- Advise of remain pure vegetarian to avoid any hyperlipidaemia
- Exercise to maintain the joint mobility
Prescribed the following therapeutic regime containing –
- Inj. Calcium Gluconate 1 ampoule every 15th day intravenous very slow
- Inj. Methyl cobalamin 1000mcg, Niacin 100mg, Pyridoxin 100mg and D Panthenol 50mg plus Betamethasone 2mg intravenous every 4th day
- Syr. NEUROVIT 10 ml every 12 hours orally
- Local application of MYONEUROL oil for transdermal absorption
- Anti arthritic analgesics (Acceclofenac Sodium) 100mg with muscle relaxant 12 hourly Orally
- Cap Vitamin D3 (Cholecalciferol) 60K every week
| Each 5ml of Neurovit syrup constitutes | |
| Acorus calamus | 100mg |
| Herpestis monneiri | 100mg |
| Evolvulus Alsenoides | 100mg |
| Nardostachys Jatamansi | 100mg |
| Cassia acuitifolia | 100mg |
| Each 30ml of Myoneurol Oil constitutes active constituents of | |
| Dhatura fastuosa (Dhatura) | 2gm |
| Boerhavia diffusa (Punarnava) | 1gm |
| Moringa pterygosperma (Sahjan) | 1gm |
| Paederia foetida (Gandh prasarni) | 1 gm |
| Allium sativa (Lahsun) | 1gm |
| Strychnos nuxvomica (Kuchla) | 1 gm |
| Nardostachys jatamansi(Jatamanshi) | 1 gm |
| Plumbago zeylanicum(Chitrak) | 1 gm |
| Vigna mungo (Mashkalayee) | 1gm |
| Zingiber officinale (Shunthi) | 4gm |
| Cuscuta reflexa (Amarlata) | 0.5gm |
| Withania somnifera (Ashvagandha) | 1gm |
| Saussuria lappa(Kuth) | 1gm |
| Brassica niger (Mustard)oil | Qs |
Patients were evaluated for duration required for relief in clinical presentation and to adjudge safety profile bio parameters were repeated every 3 months and at the end of therapy. In addition each patients were give a follow up card to enter the date of relief of presentation and nay untoward effects.
Based on the clinical improvement therapeutic efficacy was graded as
| Clinical grade | Characteristics |
| Grade I | Complete absence of presenting feature in 6 months of therapy without any untoward effects, drug adversity or withdrawal |
| Grade II | Complete absence of presenting symptoms and sign needing > 1 yr of therapy without any untoward effects, adversity Or withdrawal |
| Grade III | Only symptomatic relief with withdrawal presentation |
Result
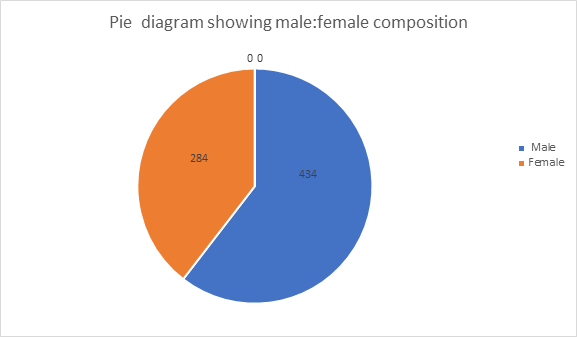
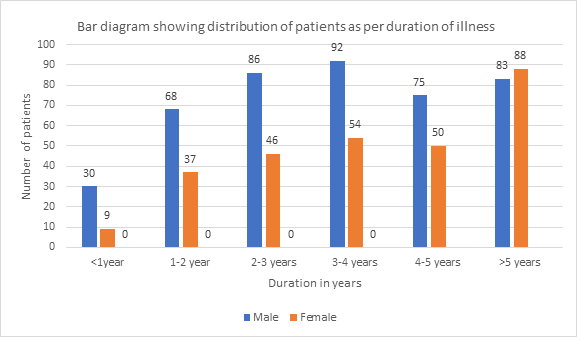
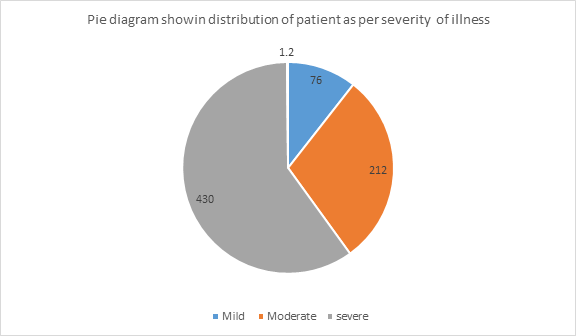
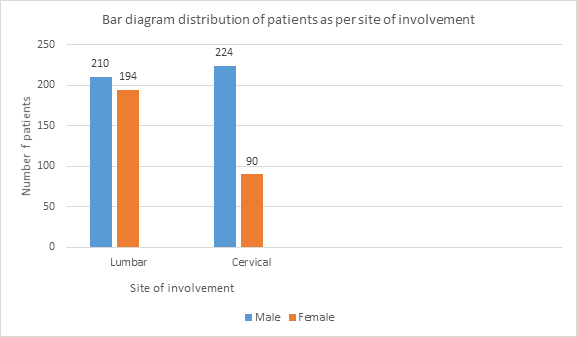
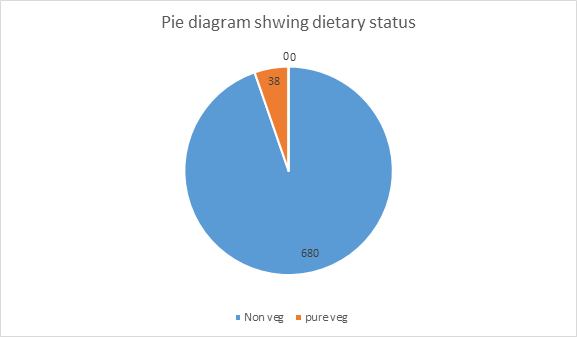
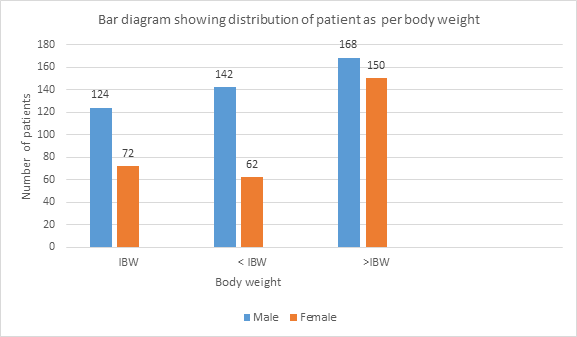
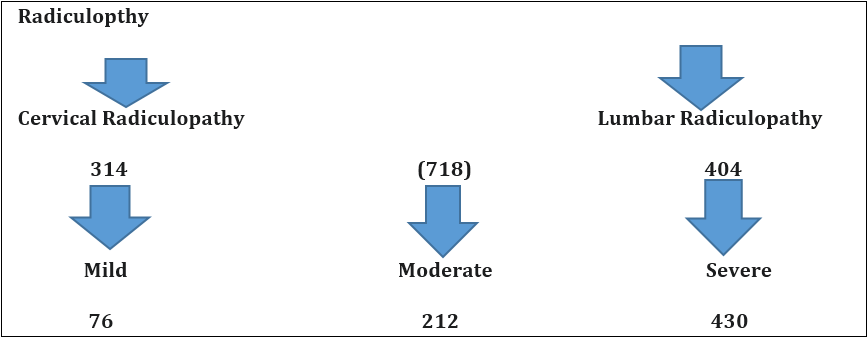
Selected patients were of age group 15-above >50 yrs out of them 2.22% were of 15-20 years while 27.8% were of age >50 years (Table-1) and 434(60.4%) were male and 284(39.6%) female (Figure 1) Out of all 5.4%(39) were suffering since < 1year while 23.8%(171) were since >5 years (Figure -2); 76(10.6%), 212 (29.5%) and 430(59.9%) were of mild ,moderate and severe degree presentation respectively (Figure -3). 404 (210 male and 194 female) were suffering with lumbar radiculitis and 314 (224 male and 90 female)with cervical radiculitis (Figure -4); 94.7% (680) were non vegetarian and 5.3%(38 ) were pure vegetarian (Figure -5); 204 (28.4% ) were with < IBW and 318 (44.3%) with >IBW (Figure-6)
| Age group (in years ) | Number of patients | |||
| Male | Female | Total | Percent | |
| 15-20 | 10 | 06 | 16 | 2.22 |
| 20-25 | 20 | 12 | 32 | 60.4 |
| 25-30 | 30 | 18 | 48 | 39.6 |
| 30-35 | 32 | 14 | 56 | |
| 35-40 | 70 | 42 | 112 | |
| 40-45 | 68 | 40 | 108 | |
| 45-50 | 88 | 58 | 146 | |
| >50 | 116 | 84 | 200 | 27.8 |
| 434 | 284 | |||
Table 1: Number of patients.
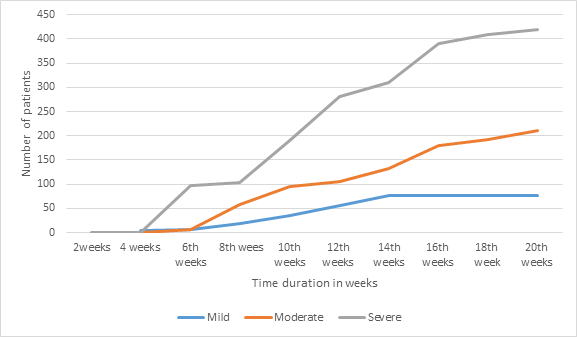
Clinical improvement was observed by 4th week in 4 patients of mild, while by 6th week in 6 and 97 patients of moderate and severe grade of severity. All patients of mild grade by 14th week while 210 and 420 patients of moderate and severe grade by 20th week of therapy (Figure -7)
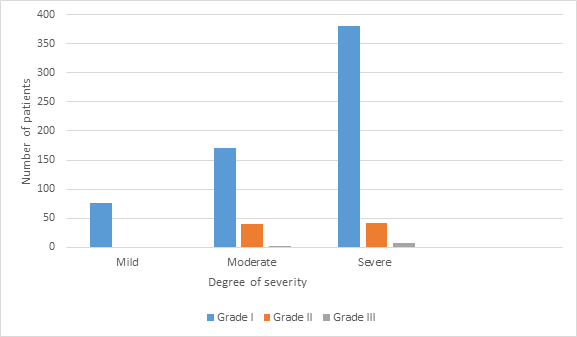
All of mild grade severity achieved grade I clinical recovery while only 170 and 380 of moderate and severe grade of clinical severity respectively (figure -8). All cases of either mild moderate and severe grade of clinical severity had radiological improvement except 02 and 08 cases of moderate and severe grade remain unchanged. No patients of either status had any change in bioparameters during therapy and 2 years of post therapy follow up. (Table- 2)
| Particulars | Number of patients | ||
| Clinical severity → | Mild | Moderate | Severe |
| Complete relief of presentation | 76 | 210 | 422 |
| Withdrawal presentation : | - | 2 | 8 |
| Radiological status : | |||
| Improved : | 76 | 210 | 422 |
| Un altered : | - | 2 | 8 |
| Worsen : | - | - | - |
| Post therapy bio parameters | |||
| Hepatic profile: | |||
| SGOT | |||
| <35IU | 76 | 212 | 430 |
| SGPT | |||
| <35IU | 76 | 212 | 430 |
| Alkaline phosphatase | |||
| <100 | 76 | 212 | 430 |
| Renal parameters : | |||
| Blood urea | |||
| <26mg% | 76 | 212 | 430 |
| Serum creatinine | |||
| <1.5mg% | 76 | 212 | 430 |
| Urine: | |||
| Albumin –Negative | 76 | 212 | 430 |
| RBC-Negative | 76 | 212 | 430 |
| Haematological : Haemoglobin | |||
| >10gm% | 76 | 212 | 430 |
| Clinical grade: | |||
| Grade I | 76 | 170 | 380 |
| Grade II | - | 40 | 42 |
| Grade III | - | 02 | 08 |
Table 2: Showing outcome of the study.
In short observation can be summarized as-
| All by 14th week | 99% by 20th week | 97.4 % by 20th week |
| Started in 4th week | 6th week | 6th week |
| Grade I -76 | 170 | 380 |
| Grade II – 0 | 40 | 42 |
| Grade III- 0 | 02 | 08 |
Discussion
Radiculitis, an agonising painful condition due to pinching of spinal nerve root at the exit or in vertebral spine is increasing these days may be due to emergence of non nutrient in diet changing life style predisposing for cholecalciferol compromise resulting in degenerative process.
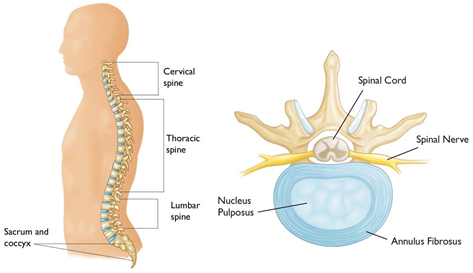
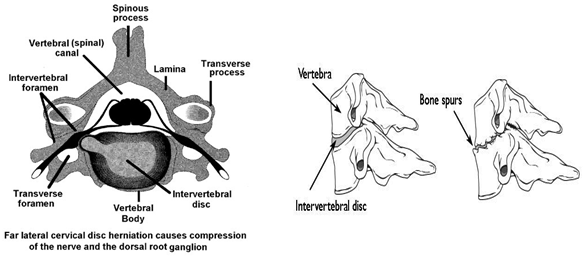
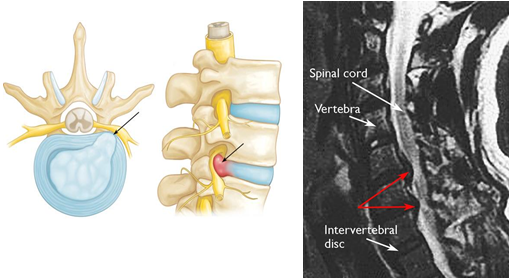
Our spine constitutes 24 bones termed as vertebrae and are stacked one over other and connect to create a canal to protect the spinal cord Spinal cord and nerves. An "electrical cables" travel through the spinal canal carrying messages between brain and muscles. Nerve roots branch came out from the spinal cord through openings in the vertebrae (foramen).
In between the vertebrae are flexible intervertebral discs which act as shock absorbers during movement or walking or running Intervertebral disks are flat, round, about 1.25 cm thick and are made up of two components:
- Annulus fibrosus. This is the tough, flexible outer ring of the disk.
- Nucleus pulposus. This is the soft, jelly-like center of the disk.
Thus any change in the intervertebral disc or adjacent bony part of vertebrae will compress the emerging nerve and cause inflammation of nerve resulting in agonizing pain full condition, also termed as Radiculopathy, which can affect cervical, thoracic and lumbar vertebral spine but out of them commonest are cervical and lumbar radiculopathy
The commonest investigation to confirm the lesion are X-ray, CT and MRI of the vertebral column. The common conventional treatment only ensure transient pain relief and 718 cases of all ready treated cases with persistent agonising state of mild, moderate and severe grade of clinical presentation shows grade I clinical response with improved quality of life in 100%, 80.2% and 88.4% patients respectively, though 0.9% and 1.9% of moderate and severe grade of clinical severity fails to prove worth.
No patients of either status had alteration in bio parameters or any adversity during therapy or 2 years of post therapy follow up. This clinical achievement of the present therapeutic regime can be explained as [17].
Betamethasone acting as anti inflammatory reduces neural edema synergized by Intravenous Calcium administration whose inclusion of one mole exit 2 mole of Sodium acting on Sodium potassium ATPase pump and facilitate decrease in neural edema and calcium ion improves neural conduction.
In addition supplementation of Calcium and cholecalciferol ensure baone repair by oesteogenesis and check degenerative changes. Methyl cobalamine, pyridoxine, Niacin and pantothenic acid support neural cells in its normal neural conduction and Neurovit a herbal composits i.e. Acorus calamus, Cassia angustifolia, Heerpestis monnieri, and Nardostachys jatamansi by its neurogenic activity helps in restoration of neural viability and vitality which combinely ensure relief in pain, neuropathic manifestation, Oral aceclofenac with muscle relaxant relieve agonizing pain while transdermal absorption of active constituent of Myoneurol oil helps ensure sustained pain relief. [18] Exercise facilitates mobility at the particular vertebral joints and sooth painful agony. Thus bioregulated osteogenesis and neural function by reducing neural edema and repairing joint facets, ensure sustained therapeutic out come and improved quality of life.
Conclusion
Present Herbal neuragen containg therapeutic regime i.e.ntravenous Calcium gluconate, Methyl cobalamine, pyridoxine, niacin and D panthenol with Betamethasone 2mg intravenous, Cholecalciferol, oral and transdermal neurotropc local application with active and passive exercise proves worth in management of Radiculopathy.
References
- MJ Hubeny. “Radiculitis”. Radiology 20.5 (1933).
- Hoy D., et al. “The Epidemiology of low back pain”. Best Pract Res Clin Rheumatol 24.6 (2010): 769-81.
- Radhakrishnan K., et al. “Epidemiology of cervical radiculopathy: a population-based study from Rochester, Minnesota, 1976 through 1990”. Brain 117(Pt 2) (1994): 325–335.
- Tarulli AW and Raynor EM. “Lumbosacral radiculopathy”. Neurol Clin 25.2 (2007): 387-405.
- Kennedy DJ and Noh MY. “The role of core stabilization in lumbosacral radiculopathy”. Phys Med Rehabil Clin N Am 22.1 (2011): 91-103.
- Urits I., et al. “Low Back Pain, a Comprehensive Review: Pathophysiology, Diagnosis, and Treatment”. Curr Pain Headache Rep 23.3 (2019): 23.
- Nguyen HS., et al. “Upright magnetic resonance imaging of the lumbar spine: Back pain and radiculopathy”. J Craniovertebr Junction Spine 7.1 (2016): 31-7.
- Al Nezari NH., et al. “Neurological examination of the peripheral nervous system to diagnose lumbar spinal disc herniation with suspected radiculopathy: a systematic review and meta-analysis”. Spine J. 13.6 (2013): 657-74.
- Miyoshi K. “[Dissociation of Anatomical (Neurological) Diagnosis and Imaging Diagnosis]”. Brain Nerve 71.3 (2019): 249-256.
- Wenger HC and Cifu AS. “Treatment of Low Back Pain”. JAMA 318.8 (2017): 743-744.
- Ament JD., et al. “Treatment of cervical radiculopathy: A review of the evolution and economics”. Surg Neurol Int 9 (2018): 35.
- Lukies MW., et al. “Safety of CT-guided cervical nerve root corticosteroid injections”. J Med Imaging Radiat Oncol (2019).
- Mattozzi I. “[Conservative treatment of cervical radiculopathy with 5% lidocaine medicated plaster]”. Minerva Med 106.1 (2015): 1-7.
- Carlesso LC., et al. “Treatment preferences amongst physical therapists and chiropractors for themanagement of neck pain: results of an international survey”. Chiropr Man, Therap 22.1 (2014): 11.
- Ramirez MM and Brennan GP. “Using the value-based care paradigm to compare physical therapy access to care models in cervical spine radiculopathy: a case report”. Physiother Theory Pract 18 (2019): 1-9.
- van der Windt DA., et al. “Physical examination for lumbar radiculopathy due to disc herniation in patients with low-back pain”. Cochrane Database Syst Rev 17.2 (2010): CD007431.
- Shankar A., et al. “Tropical spastic paraparesis and Ayurveda”. ARC Journal of Clinical Case Reports 5.2 (2019): 11-17.
- Shankar A., et al. “Pharmacological basis of indigenous therapeutics”. Bhalani Publication Mumbai 1st Edition (2019).
Citation:
Avinash Shankar., et al. “Radiculitis an Agony and Present Approach”. Medical Research and Clinical Case Reports 3.1 (2019): 24-35.
Copyright: © 2019 Avinash Shankar., et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.



































 Scientia Ricerca is licensed and content of this site is available under a Creative Commons Attribution 4.0 International License.
Scientia Ricerca is licensed and content of this site is available under a Creative Commons Attribution 4.0 International License.