Case Report
Volume 2 Issue 2 - 2018
Symptomatic Intestinal Malrotation in the Adulthood
1General Surgery Department, Hospital do Espírito Santo, Évora, Portugal
2General Surgery Department, Hospital do Espírito Santo, Évora, Portugal
3General Surgery Department, Hospital do Espírito Santo, Évora, Portugal
4General Surgery Department, Hospital Pedro Hispano, Matosinhos, Portugal
2General Surgery Department, Hospital do Espírito Santo, Évora, Portugal
3General Surgery Department, Hospital do Espírito Santo, Évora, Portugal
4General Surgery Department, Hospital Pedro Hispano, Matosinhos, Portugal
*Corresponding Author: Ânia Laranjeira, General Surgery Department, Hospital do Espírito Santo, Évora, Portugal Largo Senhor da
Pobreza 7000-811 Évora.
Received: June 27, 2018; Published: July 04, 2018
Abstract
The intestinal malrotation is defined as an anomalous rotation and fixation of the primitive midgut. Because of its rarity and non-specific symptoms, the diagnosis of intestinal malrotation in adult patients is often delayed and therefore associated with increased morbidity.
A 32-year-old male patient was referred to our department due to recurring episodes of postprandial abdominal pain and biliary vomiting dated back to childhood. Throughout his life he undergoes several imaging studies that revealed non-specific features and was treated for erroneous disorders such as functional disorder and gastroesophageal reflux until he performed an abdominal-CT scan which documented an anomalous morphology of the duodenal arch and the characteristic whirpool sign. These findings suggested the definitive diagnosis of intestinal malrotation. The patient undergoes the so-called Ladd procedure. He had an uneventful postoperative period and was discharged on the fourth postoperative day. Until this date he remains asymptomatic.
Keywords: Intestinal malrotation; congenital malrotation; Midgut; pediatric surgery; Ladd procedure
Abbreviations: CC: Cecocolic; CT: Computed tomography; DJ: Duodenojejunal; IM: Intestinal malrotation; SMA: Superior mesenteric artery; SMV: Superior mesenteric vein; TSIV: Total small intestinal volvulus; UGE: Upper gastrointestinal endoscopy; UGI: Upper gastrointestinal
Introduction
Intestinal malrotation (IM) occurs when the normal rotation of the embryonic midgut around the axis of the superior mesenteric artery (SMA) fails to occur or is incomplete. [1,2] The incidence of IM has been estimated at 0.2% in adult population. [3] While most patients present during the neonatal period or the first year of life, some present as older children or adults. Total small intestinal volvulus with malrotation occurs during the first month of life in 80% of the cases and is a very unusual finding in adult patients. The clinical presentation of IM in adults is more variable and approximately 50% of patients with IM present chronic symptoms or are asymptomatic. [4] The presence of chronic symptoms prior to a TSIV often results in a misdiagnosis and delayed treatment. [1] The diagnosis of IM should be considered in adults who present with suspect clinical features or who have incidental findings in the imaging studies. An upper gastrointestinal series and a contrast-enhanced abdominal computed tomography are the best modalities. The definitive treatment of patients with IM remains the standard Ladd procedure both in children as in adults. The authors present a case of a young man with symptomatic IM misdiagnosed since childhood.
Materials and Methods
A 32-year-old male patient was referred to our department due to chronic recurring episodes of postprandial biliary vomiting and abdominal pain. He had no family or personal medical history of interest. His social history was remarkable for active smoking and sporadic alcohol consumption. He did not take regular medication. The patient was observed several times on the emergency department due to these periodic crises characterized by nausea and postprandial biliary vomiting associated with retrosternal, epigastric and right hypochondrium pain. Complaints were aggravated by dietary intake. He described these episodes as dated back to his early childhood, sometimes with a monthly frequency and of self-limited duration of 2 to 3 days. He denied other complaints such as fever, bowel habits changes, blood loss or weight loss. In the course of the latest of these episodes, dehydration and acute renal failure were detected. On physical exam the patient was hemodynamically stable with skin and mucous membranes stained, moisturized and anicteric. The abdomen showed no distension, pain, abnormal masses or organomegaly. Rectal exploration was normal.
Routine laboratory tests showed no alterations. However, reference was made to some episodes of acute renal failure in the setting of these periodic crises with maximum values reached of blood urea nitrogen of 92 mg/dL and creatinine of 0.34 mmol/L. Urinalysis alterations were not identified, namely haematuria or proteinuria. He performed a renal US that showed no renal disease. He also performed an abdominal Ultrasound which revealed a gallstone of 2.6 mm but no other hepatic or gallbladder changes neither free intraperitoneal fluid.
He underwent an upper gastrointestinal endoscopy (UGE) that revealed an oesophagus-gastric junction at 40 cm from the dental arch, stomach with moderate biliary content and small and rare erosions at the antrum. Helicobacter pylori breath test was negative. The patient underwent a pH monitoring test and an oesophageal manometry. These exams revealed an hypotonic lower oesophageal sphincter with preserved peristalsis, biliary reflux but no acid reflux. There was no evidence of GERD as the patient had no typical or atypical symptoms and any endoscopic or pH monitoring findings were compatible with that disease. He was medicated with prokinetic agents, however, referring a little aggravation of the complaints of abdominal pain. He was referred to Gastroenterology department in order to exclude a functional pathology, food intolerance/allergy, irritable bowel syndrome or an inflammatory disease. Positive findings until that moment were biliary reflux and probably a biliary gastro-bulbitis. He was medicated with a proton pump inhibitor. He underwent an upper gastrointestinal (UGI) series that showed a discreetly hypotonic and hypokinetic stomach, with some hypersecretion fluid, permeable pyloric canal, duodenal bulb that adequately distended, duodenal arch without significant alterations, no hiatal hernia, or gastroesophageal reflux. (Figure 1)
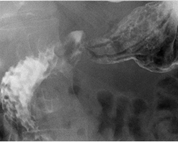
Figure 1: The upper gastrointestinal (UGI) series that showed a duodenal bulb
that adequately distended and a duodenal arch without significant alteration.
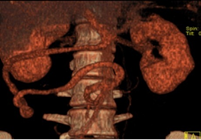
He performed an enhanced-contrast abdominal computed tomography (CT) – enterography – (Figures 2, 3 and 4) that revealed no current occlusion to the passage of oral contrast. It documented anomalous morphology of the duodenal arch with collapse of its third portion and with slight distension upstream. The duodenal arch was anterior to the SMA, slightly lateralized to the right. There was a reversed relative position of the associated vascular structures (whirpool sign), namely the superior mesenteric vein (SMV) and SMA. The SMV presented an anomalous path, circling the SMA clockwise.
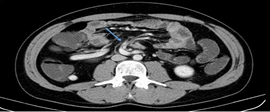
Figure 3: Enhanced-contrast abdominal CT (axial incidence) that
revealed a reversed relative position of the vascular structures (whirpool
sign), namely the superior mesenteric vein (SMV) and SMQ (arrow).
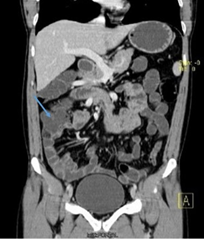
Figure 4: Enhanced-contrast abdominal CT (coronal incidence)
that revealed an anomalouse cecum position (arrow) at the right
upper abdomen and the entire small bowel on the patient’s right
side and the colon on the patient’s left side.
The patient was proposed for surgical treatment of his IM that caused repeated episodes of partial small bowel obstruction, which he accepted. The patient was advised that the Ladd procedure does not recreate normal rotation and that the risk of acute volvulus persists but is expected to be much lower following this procedure. He undergoes a Ladd procedure with cautery division of Ladd bands after a Kocher manoeuvre and lysis of ‘‘Pellerin’s mesenteric fusion’’ which are adhesions between the mesentery of the proximal jejunum and the mesentery of the terminal ileal loop. The patient presented the incomplete rotation variety, since the cecum was at the right upper abdomen and obstructing Ladd bands were present (Figure 5 and 6). It was also performed an incidental appendectomy and the bowel was placed in the corrected position of nonrotation with the small bowel on the right, the colon on the left and the cecum in the left upper quadrant. The procedure had no complications. He was discharged on the 4th postoperative day. Since surgery the patient did not have any complaints of vomiting or abdominal pain neither acute volvulus symptoms.
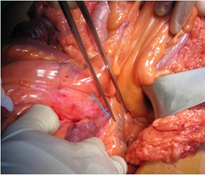
Figure 5: The duodenal arch was anterior to the superior mesenteric
artery (SMA) and there was a reversed relative position of
the superior mesenteric vein (SMV) and SMA (arrow).
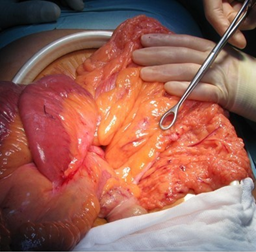
Figure 6: The entire small bowel was on the patient’s
right side and the colon was on the patient’s left side.
Results and Discussion
During embryologic development, the primitive gut is divided into the duodenojejunal (DJ) limb and the cecocolic (CC) limb. First, the intestinal loop herniates outside of the abdominal cavity and here the first 90° rotation occurs. If rotation is arrested at this stage the intestine will be connected by a wide ‘‘complete common mesentery’’. [3,4] The second 90° turn begins during the return of the intestine into the abdominal cavity. When rotation is arrested at this stage, the position of the intestine is termed ‘‘incomplete common mesentery’’ at 180°. The DJ junction lies to the right of the SMA and the “Ladd’s bands” which are attachments that bind the cecum to the posterior peritoneum may obstruct the duodenum [3,4]. This type of malrotation carries a higher risk of total small intestinal volvulus (TSIV) because the mesentery forms a narrow pedicle. [3,4] The third stage of the rotation continues during the 11th and 12th weeks. The normal primitive intestine has thus completed a 270° counterclockwise rotation divided in three separate 90° turns around the SMA, allowing the DJ limb to be positioned to the left of the SMA while the CC limb is on the right. [2-4] The duodenum becomes fixed to the posterior abdominal wall followed by the colon and the mesenteric root. These attachments form a broad base of support to the mesentery and the SMA, thus preventing twisting of the mesenteric root and kinking of the vascular supply. [5] At the end, the normal anatomy of the C-loop of the duodenum is posterior to the SMA and the transverse colon anterior to the SMA. [6]
There are distinct intestinal anomalies according to the phase at which the intestinal rotation arrests during embryogenesis. In nonrotation the DJ limb lies in the right hemi-abdomen with the CC limb in the left hemi-abdomen and TSIV and extrinsic duodenal obstruction are the most common consequences. In cases of incomplete rotation, normal rotation has been arrested at or near 180°. The cecum will usually be at the right upper abdomen and obstructing Ladd bands are present. With reversed rotation, an errant 90° clockwise rotation occurs, which leaves a winding transverse colon to the right of the SMA and the duodenum will take an anterior position. [3] Anatomically, the cecum is often situated lower and is more mobile in adult patients with malrotation, compared to children since it is the ascending colon rather than the cecum that is abnormally attached to the duodenum. [4]
The incidence of IM has been estimated at 1 in 6000 live births and at 0.2% in adult population. [3] Only 10-15% of adult patients present with TSIV, a potentially life-threatening condition. The clinical symptoms of IM are less specific in adults than in children. It is reported that 30-40% to 70% of symptomatic adults have a chronic course for several months or years characterised by nonspecific features during the postprandial period. [4] Intermittent bilious or nonbilious vomiting is the most common symptom (30%) followed by the intermittent abdominal pain (20%), failure to thrive/weight loss due to poor oral intake, early satiety, food intolerance, malabsorption or chronic diarrhoea. Like our patient, some adults report a chronic pattern of episodic vomiting and abdominal pain which is likely due to intermittent, self-limited obstruction. [1]
The imaging features can be suggestive but commonly not diagnostic of IM in adult patients. [1] The abdominal plain film might demonstrate a gasless abdomen or the evidence of duodenal obstruction with a double-bubble sign. [1,5] A barium enema can diagnose midgut volvulus associated with malrotation which is revealed by a beaked contour of the contrast. It usually demonstrates malposition of the cecum but it is normal in up to 20% of patients. [1,5]
At the abdominal CT, malrotation is suggested by the malposition of the duodenum and/or the cecum and by the “whirlpool” sign” which corresponds to the reversed relative position of the superior mesenteric vein (SMV) and SMA. [5] CT can also provide information about possible associated extraintestinal anomalies typical of paediatric population or complications such as intestinal volvulus. [1,2]
An UGI series is the “gold standard” for diagnosing IM. Normal rotation is indicated by the duodenal C-loop crossing the midline and a DJ junction located to the left of the spine. [5] Any anatomical variation may include a misplaced duodenum with the DJ junction on the right side of the abdomen; a “corkscrew” sign; signs of duodenal obstruction, the beaked duodenum if there is a volvulus and the ‘‘whirl-wind’’ sign, corresponding to the winding of the SMV around the SMA. The false-negative and false-positive rates of an UGI series in the diagnosis of IM are 6 to 14% and 7 to 15%, respectively. [1,2] Our patient presented a normal UGI which led to a delay in the correct diagnosis. It is essential the close communication between radiology and clinicians to perform an accurate and an efficient diagnosis. [6]
The Ladd procedure was described by William Ladd in 1936, and it still remains the standard surgical repair both in children and in adults. Patients who have IM with acute volvulus require emergency laparotomy with de-torsion of the volvulus to avert potential midgut bowel ischemia or necrosis. The treatment of patients with chronic presentation of IM is typically an elective Ladd procedure. The classical Ladd procedure has 4 parts: de-torsion of the midgut volvulus, if present; division of the Ladd bands; enlargement of the root of the mesentery by mobilising the duodenum and division of the adhesions along the axis of the SMA and incidental appendectomy. Some variations of the surgical technique have been reported in accordance with intraoperative findings. [2]
The Ladd procedure minimizes potential risks of volvulus by widening the base of the mesentery and placing the bowel in the corrected position of nonrotation with the small bowel on the right, the colon on the left and the cecum in the left upper quadrant. There is no recommendation to perform any pexy of the bowel loops. [1] The Ladd procedure can be performed open or laparoscopically but the midline laparotomy remains the preferred approach for treating IM because of its rarity in adult patient.
Some authors report a high rate of inappropriate surgical procedures which can be explained by the lack of familiarity with this disease and with the Ladd procedure and also by the frequent presentation at the emergency setting. Frasier emphasizes the importance of performing the Ladd procedure with the help of a paediatric surgeon. [4]
Operative mortality rates for IM ranges from 0 to 25% in adult patients depending upon the presentation being the highest in the setting of TSIV. Since the diagnosis is often delayed in adults, the postoperative morbidity rate can be high. [1]
Conclusion
In conclusion, IM in adults is difficult to diagnose, mainly due to the low incidence of this disorder and its nonspecific symptoms. Imaging tests such as the UGI series and abdominal-CT confirm the diagnosis of IM and its possible associated complications, but its characteristics can only be determined by surgery. The recommended surgical technique is the standard and modified Ladd procedure. The surgeon should re-position the intestine in the so-called ‘‘complete common mesentery’’ configuration as described by Ladd. TSIV is a very unusual finding in adult patients but the unfamiliarity with this diagnosis can lead to a potentially fatal extensive small intestinal necrosis. Thus, this diagnosis should be considered when an adult patient presents with atypical chronic abdominal pain or repeated episodes of partial small bowel obstruction.
In conclusion, IM in adults is difficult to diagnose, mainly due to the low incidence of this disorder and its nonspecific symptoms. Imaging tests such as the UGI series and abdominal-CT confirm the diagnosis of IM and its possible associated complications, but its characteristics can only be determined by surgery. The recommended surgical technique is the standard and modified Ladd procedure. The surgeon should re-position the intestine in the so-called ‘‘complete common mesentery’’ configuration as described by Ladd. TSIV is a very unusual finding in adult patients but the unfamiliarity with this diagnosis can lead to a potentially fatal extensive small intestinal necrosis. Thus, this diagnosis should be considered when an adult patient presents with atypical chronic abdominal pain or repeated episodes of partial small bowel obstruction.
Conflict of interest
No conflict of interest to declare.
No conflict of interest to declare.
References
- Buchmiller T. “Intestinal malrotation in adults”. – UpToDate (2017).
- Salamanca IMG., et al. “Unusual Intestinal Malrotation in an Adult”. Spanish Surgery 94.1 (2016): e21-3.
- M. Sidney Dasinger III; Samuel D. Smith; Chapter 31: Malrotation; Ashcraft's Pediatric Surgery, sixth edition (2014).
- Kotobi H., et al. “Total midgut volvulus in adults with intestinal malrotation. Report of eleven patients”. Journal of Visceral Surgery 154.3 (2017): 175-183.
- Christina Bales and Chris A. Liacouras; “Intestinal Atresia, Stenosis, and Malrotation”. Nelson Textbook of Pediatrics, Edition 20, Chapter 330, 1800-1804.e1
- John J Tackett., et al. “Malrotation: Current strategies navigating the radiologic diagnosis of a surgical emergency.” World Journal of Radiology 6.9 (2014): 730-736.
Citation:
Ânia Laranjeira., et al. “Symptomatic Intestinal Malrotation in the Adulthood”. Medical Research and Clinical Case Reports 2.2
(2018): 155-160.
Copyright: © 2018 Ânia Laranjeira., et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.



































 Scientia Ricerca is licensed and content of this site is available under a Creative Commons Attribution 4.0 International License.
Scientia Ricerca is licensed and content of this site is available under a Creative Commons Attribution 4.0 International License.